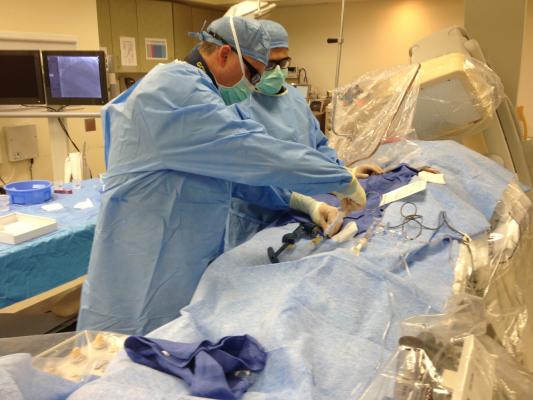
November 10, 2016 — A Henry Ford Hospital cardiologist is pioneering a promising new procedure to improve the success of mitral valve replacement.
Interventional cardiologist Adam Greenbaum, M.D., medical co-director of the Center For Structural Heart Disease at Henry Ford Hospital, believes the procedure — slicing a leaflet with an electrified wire through a tiny catheter before replacing a mitral valve — will save thousands of lives.
Greenbaum helped perform the first procedure in man on May 25, 2016 at Emory University in Atlanta and led the second procedure at Henry Ford Hospital on June 8. Since then, cardiologists have performed nine of the highly specialized procedures, six at Henry Ford Hospital.
“It’s in its infancy, but was successful in all patients,” said Greenbaum. “It’s extremely invigorating to say someone who had no options now has a beautifully working mitral valve, repaired in a safe manner with the use of only catheters. This could be life-saving for many people.”
The procedure is medically described as ‘laceration of the anterior mitral valve leaflet to prevent outflow track obstruction,’ and nicknamed with the acronym “LAMPOON.”
The LAMPOON procedure is designed for patients who need a new mitral valve. The mitral valve regulates the flow of blood between the left top and bottom chambers of the heart after it has been oxygenated in the lungs. The ventricle then squeezes the blood out through the aortic valve and into the body.
Doctors can replace a mitral valve two ways: through open-heart surgery, or by deploying a valve through a small catheter guided through blood vessels and into the heart if patients are felt to be too sick for open surgical repairs. But in up to 50 percent of patients, the heart’s anatomy can cause problems. In some people, when the cardiologist positions and opens the new mitral valve, the original valve leaflet gets pushed back and can block blood flow out of the heart. The complication is fatal.
In open-heart surgery, doctors cut away the blocking tissues. That is not an option for those too sick to undergo open-heart surgery, leading Greenbaum and his team to search for an alternative.
In the catheter-based LAMPOON procedure, the cardiologist weaves a catheter through the patient’s blood vessels and into the heart. The doctor then uses an electrified wire about the size of a sewing thread woven through the catheter to slice away the problem tissue.
“We don’t know how many people have been turned away due to their anatomic risk,” said Greenbaum. “Now we think we have conquered that obstacle.”
Greenbaum has been working with interventional cardiologist Robert J. Lederman, M.D., and fellow Jaffar Khan, M.D., at the National Heart, Lung, and Blood Institute, who first performed the technique in animals; and Vasilis C. Babaliaros at Emory University School of Medicine, who performed the first human procedure in May.
Greenbaum and Lederman also performed the first transcaval access procedure in man, a novel way to access the heart by connecting blood vessels in the abdomen. A multi-center study of the procedure recently reported a 98 percent success rate for the procedure.
For more information: www.henryfordhospital.com


 May 13, 2026
May 13, 2026 









