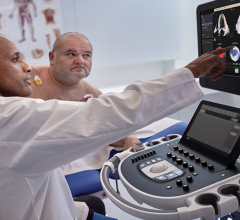
An example of artificial intelligence on the GE Healthcare Vivid E95 system shown at ASE 2019 where the AI automatically pulls in an exam, identifies the left ventricle and myocardial boards and then calculates all the strain measurements in less than 10 seconds. While AI automation can greatly speed workflow, there are questions about the accuracy of AI for the next step in making diagnoses.
Artificial intelligence (AI) is growing in all areas of medicine and was the topic of several advanced technology sessions at the American Society of Echocardiography (ASE) 2021 meeting. Speakers pointed out that more work is needed to increase the quality and amount of data use to train cardiac ultrasound AI algorithms.
"When we choose to use AI for clinical decision making, it is important that we recognize where we make errors in clinical decision making," explained Bart Bijnens, Ph.D., Universitat Pompeu Fabra, Barcelona, Spain, in an ASE session examining if AI is ready yet for aiding clinical decision support.
"If we can use artificial intelligence to help make better image acquisitions to start, we would avoid some of these issues," Bijnens said.
He said a stepping stone to AI decision support would be using AI to improve echo image acquisition first. Currently, ultrasound image exam quality is largely determined by the experience of the sonographer, and quality of exams can vary widely from one operator to at the next. Bijnens said AI algorithms already exist to help guide less experienced users to perform consistent, diagnostic quality exams.
Bijnens said factors that contribute to diagnostic errors include under interpretation of a finding, technical factors in the imaging, and incomplete examinations make up more than 60 percent of diagnostic mistakes in echocardiography exam reads.[1] He said AI can help overcome these issues by guiding the ultrasound machine user, and AI can help act as a second set of eyes to catch additional features in images that are worth review. Today, he said AI is already being integrated in many vendors' systems to help speed workflow.
"We are seeing some of these things now in clinical practice, where some of the manufacturers have started added machine learning for feature extraction for automated measurements on our machines," Bijnens said.
Read more about this type of AI technology in the article Northwestern Medicine Introduces Artificial Intelligence to Improve Ultrasound Imaging
Moving AI From Identifying Echo Landmarks to Actual Diagnostics
While AI can help identify ventricular walls of the heart and ideal imaging planes to make measurements, it is a further leap to have AI systems diagnose patients from these images. Bijnens showed an example of an AI algorithm trained to identify dilated hypertrophy. However, the AI marked a case of left ventricular hypertrophy as normal, because they AI needs more information to understand variations of clinical presentations. This may include additional, automated AI review of patient waveforms and other data that could help the AI be much more specific than just looking at imaging data and relying only on image feature matching alone.
"AI offers us an opportunity for personalized medicine that can be used for image data acquisition feature extraction, information integration and interpretation," Bijnens explained.
The Need for Data Repositories to Enhance Research and Train AI Algorithms
AI offers opportunities for more personalized care, but to train this type of algorithm, massive amounts of patient data are needed. Data to train AI can come from hospitals that capture it and are willing to share it for use in training algorithms. But, much larger, standardized sets of data are needed, which has been a major bottleneck in AI development. To accelerate AI development, the use of standardized registries may play a key role in the coming years.
Large data repositories that use the same data fields are needed to help reduce bias and enable more reproducible research results, explained Charitha Reddy, M.D., Lucile Packard Children's Hospital, Stanford University in a session at ASE 2021. In pediatric cardiology research, where there are very low numbers of patients to begin with, pooling data in repositories would greatly enhance research as well as training for AI algorithms to automatically identify and assess these rare conditions.
"Unlike single center studies, large data repositories would combine data from many hospitals, which can help identify and reduce inherent biases," Reddy said. "Repositories also would help with reproducibility of studies. Machine learning is an exciting new frontier in healthcare, but pediatric centers are lagging behind due to the lack of large data sets. Data sharing can help mitigate this."
She said hospitals each store data differently, some in the cloud, some on servers within the hospital. Data also comes from a multitude of sources, including various imaging modalities, ECG, wearables, genetic tests, blood tests, and point-of-care tests. The way the data pieces are integrated is often different at each hospital. HIPAA patient privacy concerns also can challenge the aggregation of patient data into larger registries.
From a technical standpoint, aggregating data into a central location can sometimes be difficult, even in just one hospital due to a combination of structured and unstructured data, missing data, and disparate formats that prevent the data from working in one or more computer system or applications. This also prevents data from being useful for later data interpretation. Reddy explained one example that is commonly encountered.
"Patient echocardiograms may exist in a specific PACS platform, but they are then converted into a PDF in that center's electronic health record," she said. "In addition, the data in echo reports can be both structured and unstructured, in terms of measurements and in terms of free text. There are limited methods to categorize this unstructured data."
Reddy also said there are technical issues with linking data together for a specific patient, such as assigning a patient identifier number that can link data across platforms or repositories. She said large data repositories can be built using a centralized site to dump data, but it is vulnerable to HIPAA privacy concerns and the data no longer resides at the hospital or health system of origin, which may raise legal issues as well.
Another model could be the use of a federated system, where data resides at each hospital or health system to increase control of what the data is used for and data privacy. This also could be less costly, Reddy said. Under a federated system, in order to use the data to train an AI algorithm, the algorithm would need to have access to the data one site at a time to maintain privacy.
A new concept in IT that may help with repository building and research is edge computing. She said this is where the data comes directly from machines creating it. This includes imaging systems, ECG, wearables, and labs. The AI training, computing and deployment is at the "edge" of the server, rather than pulling data from deep within and from throughout the server. This also decrease latency of data transfer, making responsiveness very fast.
Related Echo AI and ASE Coverage Content:
Artificial Intelligence Guided Point of Care Ultrasound by Novice Users
Development of Echo Blood Flow Dynamics Imaging
Development of Computer Generated Virtual Hearts Using Echocardiography
VIDEO: Artificial Intelligence Identifies High-Risk COVID Patients From Cardiac Ultrasound — Interview with Federico Asch, M.D.
New Technologies Featured at the American Society of Echocardiography 2021 Virtual Meeting
3 Studies Show How Echocardiography is a Key Tool in Women's Health
Echocardiography Related COVID-19 Research Presented at ASE 2021
Northwestern Medicine Introduces Artificial Intelligence to Improve Ultrasound Imaging
New Cardiac Diagnostic Tool Helps Automate Point-of-Care Ultrasound Screening
JAMA Cardiology Article Shows Effectiveness of AI-Guided Ultrasound Software
Mayo Clinic Uses Artificial Intelligence to Help Assess Cardiac Danger From COVID-19
Find more content on artificial intelligence in cardiology
Reference:


 May 04, 2026
May 04, 2026