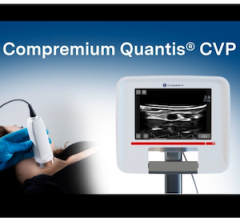
Cardiodynamics' BioZ impedance cardiography
Intensive care units are highly dependent on the efficient transfer of physiological data to multiple healthcare providers. In the delivery of healthcare in 2006 there exists a strong rationale for a tight relationship between critical care and information technology (Celi, Hassan, Marquardt, Breslow, & Rosenfeld, 2001).
First and foremost is patient safety. Our patient population is aging. Major events in this patient group (e.g., cardio-pulmonary arrest) can be predicted by abnormalities in patients' vital signs (Fieselmann, Hendryx, Helms, & Wakefield). Furthermore, severity of illness within intensive care remains high. Demand exceeds supply of both ICU healthcare providers and critical care beds. To complicate the matter further, there is increasing pressure to provide high-level intensive care in an era of increasing cost control.
Hospital Information Technology appears to offer a means to address these challenges. By increasing accessibility to information about our patients, our diverse, highly trained intensive care workforce may achieve advantages, addressing the challenges of supply and demand. Donabedian, in his sentinel work, emphasized the development of “structure, the implementation of effective care processes, and...adaptive quality assessments” in order to achieve progressive quality in healthcare (Donabedian, 1988).
Within critical care, the reality of connecting physiological monitors, essential life support devices such as mechanical ventilators and high-intensity-care units throughout a hospital are increasingly achievable. The benefits of this structure — enhancing critical information transfer — can only be obtained through deliberate planning. We must develop improved strategies to use the increased quantity of clinical data generated by our medical monitors and devices.
Intensivists, surgeons, critical care nurses and other healthcare providers use biomedical information from the ICU monitors to reverse abnormal physiology. Physiological information will become increasingly available to ICU physicians, both within and outside of the hospital. Early evidence supports using ICU monitoring data within a scope of clinical care, favorably improving hospital outcomes (Breslow et al.).
First-Hand Experience
Importantly, at the University of Iowa Hospitals and Clinics (UIHC), we are in the midst of a renaissance of IT capabilities within our intensive care practice. As a rural, tertiary level hospital, we do not have the capacity to have an intensivist at the patient's bedside 24/7 in all of our six ICUs. As a result of the efforts of our hospital IT department, intensivists can now “see” the majority of physiological vital signs (e.g., temperature, pulse, pulse oximetry, capnometry, arterial pressure, ventilator data and ICU alarms) on personal computers, both inside and outside of the hospital around the clock.
This practice has helped to extend limited intensivist resources. Remotely, the intensivists can read the medical record, review critical labs, and inspect relevant radiology. In the upcoming months, our intensivists will be able to confirm that appropriate processes of ICU care have been completed on a timely basis via the Internet (for example, hyperglycemia control).
Have these enhancements decreased nighttime journeys to the University Hospital for on-call intensivists? No — at least not yet. Our intensivist colleagues continue to strongly support the bedside evaluation of care that has developed over the years of traditional medical practice.
The new technology has, however, limited some worry and the number of phone calls by allowing the intensivist the option to monitor ICU patients remotely throughout the day and night. Some have reported early recognition and treatment of developing issues of patient care — this is encouraging but anecdotal. There is a significant need for an innovative, randomized, controlled trial that proves that this new high-level of connectivity clearly improves clinical outcomes in multiple clinical settings.
But challenges remain.
The cornerstones to building increased connectivity of ICU data — the “eICU” — must include ensuring communication of essential ICU devices necessary for clinical decision-making. Clinicians need to develop an understanding of the predictive value of ICU electronic data; we need to learn what the key eICU data elements are that can be used effectively to improve patient care.
Quality, Not Just Quantity
In the integration of data and devices it is not enough to collect the data and put it on a legal document. It needs to be presented in a way that enables accurate interpretation, evaluation and appropriate monitoring. Today's tools can enable practitioners to be data rich and, at times, information poor.
In prepping for the implementation of our critical care system, the proposed legal chart document reflected data points for one patient's 24-hour experience in the ICU, totaling 14 pages. Rich in data points, the proposed document would have failed to serve even a trial lawyer well.
Our challenge is to be both savvy and simple in our solutions, summarizing presentations based on the patient's condition so as to enable quick evaluation and a tuned sensitivity to changes in the patient's status.
Key to the success is an intelligent dashboard that, within seconds of review, enables the physician to assess patient acuity across the unit and triage their attention to those of priority need. Intuitively, these tools must guide the care team in best practices, as well as adequately collect appropriate data to support continual background evaluation.
The prudent consumer of each hospital device purchase will carefully consider its capabilities in connectivity within the overall scope of the virtual IT environment.
Speaking the Same Language
There is a strong need for standardization of languages to allow for the integration of biomedical devices. Automation forces collaboration between clinical entities. It forces the "apple to oranges" ambiguities that are tolerated in a paper world to be resolved. Not only do standard processes and languages serve to get the disparate entities on the same page, they serve back-end outcome evaluation and process improvement initiatives.
Finally, fundamental to improving healthcare is the continuous measurement of outcomes (Donabedian, 1988). Adapting and improving clinical practice requires ongoing measurements to identify both successful and challenged processes of care. This information, in turn, must be integrated into an institutional structure to refine clinical practices.
In 2001 the Institute of Medicine in Crossing the Quality Chasm emphasized the importance of building organizational supports for improving the delivery of healthcare (America, 2001). The integration of IT and ICU practice can be an important bridge, if deliberately planned and thoughtfully constructed. Through careful assembly of data, complete with appropriately targeted alerts and best-practice guidelines, intensivists will be better positioned to deliver high-level intensive care to our high-risk patients.
References:
Committee on Quality Care in America, C. o. Q. H. C. i. (2001). Crossing the quality chasm: a new health system for the 21st century. Washington, DC: National Academic Press.
Breslow, M. J., Rosenfeld, B. A., Doerfler, M., Burke, G., Yates, G., Stone, D. J., et al. Effect of a multiple-site intensive care unit telemedicine program on clinical and economic outcomes: an alternative paradigm for intensivist staffing. Crit Care Med. 2004 Jan;32(1):31-8.
Celi, L. A., Hassan, E., Marquardt, C., Breslow, M., & Rosenfeld, B. (2001). The eICU: it's not just telemedicine. Crit Care Med, 29 (* Suppl), N183-189.
Donabedian, A. (1988). The quality of care: how can it be assessed? Jama, 260, 1743.
Fieselmann, J. F., Hendryx, M. S., Helms, C. M., & Wakefield, D. S. Respiratory rate predicts cardiopulmonary arrest for internal medicine inpatients. J Gen Intern Med. 1993 Jul;8(7):354-60.
7th International Consensus Conference in Intensive Care Medicine
Hemodynamic Monitoring in Shock and Implications for Management
Sponsored in part by the Society of Critical Care Medicine (SCCM), an 11-person jury will convene in Paris, France April 27-28, 2006 to debate the following:
1. What are the epidemiologic and pathophysiologic features of shock in the ICU?
2. Should preload and fluid responsiveness in shock be monitored?
3. Should cardiac output in shock be monitored?
4. Should markers of regional circulation and oxygen consumption in shock be monitored?
5. Is there an evidence-based rationale for using hemodynamic monitoring in shock?
For more information visit www.srlf.org



 April 06, 2026
April 06, 2026