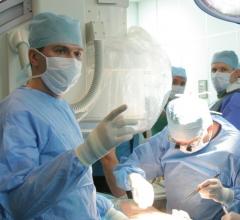
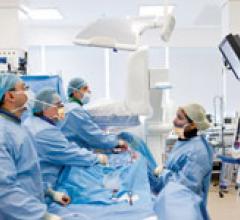
In the past decade, there has been a major push toward minimally invasive cardiac procedures. In the cath lab, interventionalists have found new catheter-based treatments in an attempt to reduce or eliminate the need for open heart surgery. In the operating room (OR), advances have been made with new tools and techniques to reduce patient trauma and speed recovery. These include port, or keyhole, surgeries, the introduction of the da Vinci surgical robot and beating heart surgeries to reduce the use of cardio/pulmonary bypass.
In the past, there was much discussion about turf wars between cardiac surgeons and interventionalists, but in recent years that discussion has increasingly turned to collaboration rather than competition. This is especially true since these specialties began serious comparative effectiveness studies and gathered solid, empirical data showing some patients fare better with surgery and others with interventional therapies. Also, as minimally invasive procedures become increasingly complex, surgeons have found a need to collaborate with the interventionalists for their tools, skills and their high-quality angiography imaging systems. Complex interventional procedures also call sometimes for a surgical cut-down or other surgical expertise, as needed during transapical, transcatheter aortic valve replacement procedures.
This convergence of expertise, deciding what is the best approach for patients and combining skill sets, imaging systems and tools of both interventionalists and surgeons, is the recent trend of hybrid ORs.
However, it is not enough to build a multimillion-dollar suite and expect it to draw new patients and allow new procedures. The key ingredient to make these numbers grow is actually the human element, not cutting-edge technology. Since I began covering hybrid ORs, clinicians with successful hybrids over and over again have said close collaboration and a team approach are essential.
There are some hospitals and physicians who don’t believe a hybrid OR is necessary. There are also those facilities that invested large sums to create a suite, only to find it was only being used as an additional OR, while the million-plus dollars’ worth of angiographic imaging equipment sat in the corner collecting dust. In these cases, I theorize the facilities did not have a real need for a hybrid, were not yet ready for such a facility, or lacked the key ingredient of multi-specialty collaboration that is necessary for success. Hybrid ORs are not about hopping on a bandwagon. Hospitals need to evaluate whether there is a real need and if their physicians are enthusiastic about working together in a closely coordinated manner.
Two stories regarding hybrid ORs are highlighted in the March-April 2012 issue: The Economics of Hybrid ORs and Mayo Clinic’s Valve Program Ranks Among the Most Innovative Heart Centers.


 October 02, 2020
October 02, 2020