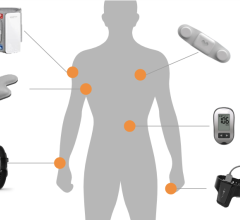
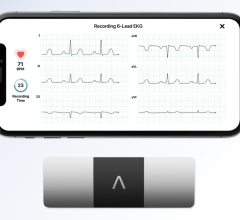
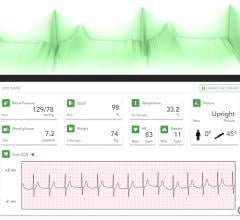
Via Christi Health System's eICU Central Command Center is staffed with intensivists and critical care nurses. The remote monitoring aids ICU staffs with extra eyes and expertise.
With the progression toward a seamless electronic health records (EHR), seamlessly connecting numerous medical devices to one hospital network is becoming as important as the devices themselves. The connectivity of vital signs monitors to hospital networks not only offers EHR and enterprisewide data efficiencies, but also offers telemedicine opportunities such as remote ICU monitoring.
Connectivity issues
The biggest issue with connectivity is manufacturers have developed their own proprietary computer programs and connectivity solutions that are not compatible with those from other makers. For this reason most hospitals purchase a complete system from one manufacturer, said Leeanne Cordisco, GE business manager for education services, who organizes IT classes through GE Healthcare for hospital biomed engineers.
“Any major vendor who sells monitoring devices will also sell a central nursing monitoring station,” she said.
While most hospitals purchase an entire system from one company that includes the monitoring devices, connection solutions and central monitoring stations, these networks may vary from department to depart. Many departments are given the freedom to purchase what it feels is best for its needs. In other cases, systems were purchased prior to a hospital's migration toward a seamless EHR system. Cordisco said this has led to connectivity issues where monitoring systems that work in the ER do not work with the monitoring systems in the OR or ICU. Many hospitals are increasingly going to enterprisewide networks, which allow the transfer of information from triage through discharge and billing. For these reasons manufacturers are trying to make devices easier to connect to one another.
“They are getting more compatible all the time,” she said.
To make monitoring devices more compatible, device manufacturers created the IHE (Integrating the Healthcare Enterprise) organization. The engineers from all these companies are working together so the next generations of devices will connect to central monitoring stations and other electronic health record (EHR) integrated systems, regardless of who made the hardware or software.
“That is the Holy Grail that IHE is working toward,” Cordisco said.
Working toward that goal, she said makers are starting to use universally agreed-upon healthcare computer language formats, including HL7 for data entry and transfer from department to department, and DICOM for the transfer of large volumes of information, such as radiology images.
However, in the meantime hospitals' best bet is to get a complete system from a single vendor, Cordisco said.
“Savvy hospitals are looking for the total package,” Cordisco said.
This usually includes the monitoring devices, central nursing station monitoring equipment, connections, training, technical support, repair, and allows for upgrades.
“Hospitals should ask themselves what is going to give them the most return on investment over the longest term,” Cordisco said. “That is essential today.”
Many hospitals are moving toward wireless networks to connect monitoring devices and nursing mobile computers. From a biomed engineer's perspective, hospitals need to consider three key factors when using Wi-Fi connections, Cordisco said. First, the security of a wireless system is paramount with a strong encryption to prevent Wi-Fi hacking of patient information.
Second, she said dropout (the loss of signal from a device) must be minimized. Wi-Fi signal coverage should be tested throughout the hospital to ensure telemetry is not cut off from the network when a patient is moved.
“Dropout with a medical system is very bad,” Cordisco said. “If a company's e-mail system goes down for half an hour it's an inconvenience, but if a biomedical device goes down for half an hour it can be life threatening.”
Thirdly, Cordisco said scalability in very important. Systems should be able to have additional monitors added in case of a department expansion, or in case of a major disaster when extra monitors are brought in to deal with a a sudden influx of patients.
Cordisco heads a new nonvendor-specific hospital IT biomed engineer training program offered by GE Healthcare. The hands-on courses are designed to help engineers troubleshoot connectivity issues with their networks, regardless of what manufacturer's equipment they use.
Outsourcing patient monitoring
Increased networking and connectivity of patient monitors now allows for remote monitoring of patients by clinicians hundreds of miles away via telemedicine. The growing trend of remote 24/7 ICU monitoring technology is offered by a few companies to help monitor high-acuity patients more economically, especially in rural areas.
The eICU Program developed by Visicu is being used by hospitals in the Philadelphia, Atlanta, Phoenix, Sacramento and Kansas. Board-certified doctors in a hospital 300 miles away can shadow nurses and doctors in the ICU where there are not enough resources to constantly keep an eye on all the patients. These remote colleagues can see, hear and monitor these patients for respiratory and blood pressure changes as if they were in the ICU. The remote doctors can alert the attending physician and nurses of any problems.
In a state known historically for its cattle drives in the days of the old western frontier, it is fitting that today this pioneering eICU technology frontier is being headed by a cowboy. Dr. Elizabeth Cowboy, M.D., FCCP, medical director of eCare-ICU with Via Christi Health System based in Wichita, KS, said the system can monitor up to 155 ICU beds in four hospitals spread over a radius of 300 miles. Her eICU program now helps watch 28 percent of the ICU patients in the state of Kansas.
Since implementing the system in April 2006, Dr. Cowboy said a comparison between pre- and post-implementation statistics shows more than 100 additional patients are alive today because of lower mortality rates since starting eICU monitoring.
“We have seen significant improvements in the mortality rate,” Dr. Cowboy said.
She attributes that success to the system's ability to allow intensivists to remotely monitor patients while clinicians in the ICU attend to patient's physical needs.
“It provides 24-hour access to clinicians skilled in critical care,” she said. “It's designed to be an assistant to the bedside team... It's similar to a doctor being at the end of the bed with their hands in their pockets and they can only advise staff based on what they see and hear to make decisions.”
This is especially important in smaller rural hospitals.
“The technology allows us to reach into areas where (hospitals) might not be able to recruit a full-time intensivist,” Dr. Cowboy said. “It helps improve the quality of healthcare and safety for the patient regardless of where they are at.”
She said this has helped the health system recruit and retain more qualified nurses and doctors in remote areas because they know they will have additional clinical support.
Another attribute is the speed at which knowledge can be spread to remote healthcare facilities using the system. She said this enabled Via Christi to implement consistent use of best practices across its hospitals.
The system allows patient vital signs from anywhere to be monitored in real time. When an alarm sounds or if the monitoring physician sees something wrong, they can instantly call-up the patient's chart. They can also switch on a video camera mounted over the patient to see what is going on. Dr. Cowboy said the cameras are high resolution and clearly show text on items like IV bags down to a four-point font. If an issue arises, the remote clinician can quickly notify the staff in the ICU to intervene. The remote intensivist can also help make clinical decisions and instruct the staff if needed. The system links into an intercom system in each room so the remote doctor can speak to the patient or to the on-site clinicians.
Dr. Cowboy said the system also figures prominently in the health system's disaster planning, where remote monitoring can be used to immediately shift extra medical staff to monitor patients at hospitals anywhere in Kansas, or around the country.
If implementing a remote monitoring ICU program, Dr. Cowboy suggests the hospital staff understand what their benchmarks will be and discuss how the technology can help advance medicine and patient care in their system. She said it is also important to review state laws on patient privacy and physician certification, which can differ by state and may be an issue when connecting doctors and hospitals from different states.


 September 16, 2025
September 16, 2025