
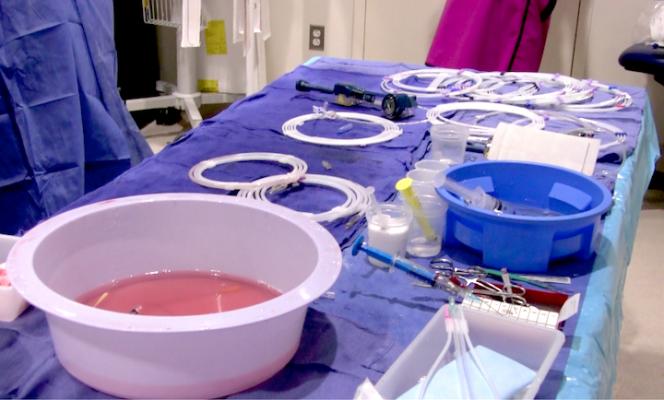
There are always a lot of guidewires used in CTO cases, but they all look the same so it can be confusing as to which is which as they are exchanged out and are all set on the same table. John Messenger, M.D., at the University of Colorado, likes to write the name of each wire on a towel and put the towel on top to keep them straight for himself and staff in the room. Photo by Dave Fornell.
Guidewire engineering has become more advanced over the past decade as interventional cardiologists have advanced their trade to tackle much more complex lesions, including chronic total occlusions (CTO). Operators have moved beyond simple, straightforward percutaneous coronary intervention (PCI) lesions and are now tackling harder-to-reach lesions. These lesions are often located in tortuous vessel anatomy and include revascularizing completely blocked CTO vessel segments. CTOs often require guidewires approaching the blockage both antegrade and retrograde, and at times using a subintimal approach. These procedures often require several types of guidewires and frequent exchanges, so these procedures have become the biggest growth area for new guidewire technology.
Choosing the Right Guidewire for CTO Procedures
These more complex lesions require a tool box of guidewires that have varying attributes to address specific access issues. However, there are many dedicated CTO guidewires on the market — too many for a single operator to become proficient with, explained Bill Lombardi, M.D., director of complex coronary artery interventions at the University of Washington, Seattle, and a top expert in CTOs. He said it is easy to get into “paralysis by analysis,” where there are just too many choices, information overload and confusion about what to pick. He said the idea of the hybrid CTO approach is getting rid of extraneous equipment in the lab and just keeping a handful of tools the operator can master.
 "It can get confusing," agreed Khaldoon Alaswad, M.D., a CTO expert and director of the cardiac catheterization lab at Henry Ford Hospital, Detroit. "We like to limit the number of devices used per procedure, not only from an economic standpoint, but also from an efficiency standpoint."
"It can get confusing," agreed Khaldoon Alaswad, M.D., a CTO expert and director of the cardiac catheterization lab at Henry Ford Hospital, Detroit. "We like to limit the number of devices used per procedure, not only from an economic standpoint, but also from an efficiency standpoint."
In his lab, he said they try to pick a limited number of wires that all the staff can become experts in using and have application across the department for different types of procedures. "With antegrade wire escalation you go from a soft tip polymer jacketed Fielder XT-A, XT or XT-R, to a pilot 200 and Confianza, and we have added harder tipped wires like the Hornet 14, Astato 20 and Astato 40. For retrograde access we use most of the micro catheters available, including the Mamba, Corsair, FineCross and Micro 14. Each one of us has their own workhorse wires and guide catheters we use. If you have a limited number of tools, devices and wires, you learn to master them."
“There are a lot of me-too devices out there, so don’t get lost in that, just focus on picking very different devices, but keep the number limited. Less choices is actually better,” Lombardi explained.
Lombardi said most CTO operators pick just three types of wires to concentrate on:
• Stiff polymer jacketed wire. An example would be the Pilot 200 (Abbott);
• A stiff penetrating wire, like a Confianza Pro 12 (Asahi) or a Hornet 14 (Boston Scientific); and
• A more steerable guide wire, like a Gaia series (Asahi), if the operator knows where they are going inside the vessel.
"In general, we follow the hybrid algorithm, where we try not to spend too much time on one particular method of crossing if it is not working," said Kevin Rogers, M.D., CTO expert and director of vascular medicine at the University of Colorado Hospital. "With wire escalation, the Pilot 200 is really our workhorse crossing wire. I Think Fielder XT is good if we need to go subintimal with a plan to re-enter the lumen, or if there is a micro channel. For septal crossing, Asahi Sion is what we go to first, but then Fielder XT. We typically go to a Confianza Pro 12 as our last-resort wire. It's good to have five wires you are really comfortable with and try to stay away from the really aggressive wires early on, especially if the anatomy is ambiguous at all."
Basic Guidewire Characteristics

There are dozens of different types of guidewires on the market with different performance characteristics designed to navigate the wire through vessels to reach a target lesion or vessel segment. Once the tip of the device arrives at its destination, it acts as a guide that larger catheters can rapidly follow for easier delivery of stents or balloons to treat the vessel.
Wires are characterized by their pushability, steerability, torque and opacity. Pushability is the amount of force needed to advance the wire. Steerability is the ability and responsiveness of the wire tip to navigate vessels. Torque is the response of the wire to turning by the operator when navigating vessels. Its opacity is its level of visibility under fluoroscopic X-ray angiography imaging.
Guidewires come in two basic configurations: solid steel or nitinol core wires, and solid core wire wrapped in a smaller wire coil or braid. Coiled or braided wires offer a large amount of flexibility, pushability and kink resistance. Some of Boston Scientific’s guidewires use a nitinol tube with micro-cut slots instead of braided wire to improve torque control.
Nitinol wire, used by itself or braided with stainless steel, helps increase flexibility and allows the wire to spring back into shape after navigating a tortuous vessel segment. Many guidewires have a floppy tip and a stiff body to enable easy tip navigation, with good pushability offered by the stiffer section of the wire.
Some wires are coated with a polymer, such as silicone or polytetrafluoroethylene (PTFE), to increase lubricity. Hydrophilic coatings reduce friction during deployment and make for easier movement in tortuous vessels.
Consolidation in the Guidewire Market
In December 2016, Teleflex Inc. purchased Vascular Solutions Inc. in a deal valued at about $1 billion. Vascular Solutions developed more than 90 device technologies for catheter-based coronary, peripheral vascular, venous, electrophysiology and interventional radiology use. The acquisition was expected to greatly boost the growth of Teleflex’s vascular and interventional businesses. Teleflex said at the time of the purchase it was also interested in Vascular Solutions' longer-term prospects for several products in the R&D pipeline, which include next-generation products to address complex interventions, radial artery catheterizations and embolization procedures.
The addition of Vascular Solutions greatly enhanced Teleflex’s presence in the interventional cardiology, interventional radiology and peripheral vascular markets. The combined company will offer more than 150 cardiac, vascular and interventional access products. Teleflex also inherited a direct U.S. sales force and international independent distributor network.
In October 2017, BTG acquired Roxwood Medical in a deal valued around $80 million. Roxwood's anchoring catheters (CenterCross, CenterCross Ultra, MultiCross) and microcatheters (MicroCross) offer options for physicians in the crossing of complex lesions and arterial blockages. By incorporating a self-expanding scaffold that stabilizes the delivery of a guidewire, Roxwood’s catheters provide positioning accuracy and support to facilitate the crossing of blockages, mitigating guidewire buckling and enabling treatments such as angioplasty, stenting or atherectomy.
FDA Developing New Rules on Guidewire Development
The U.S. Food and Drug Administration (FDA) is in the process of updating two guidance documents for vendors developing new coronary, peripheral and neurovascular guidewires. The FDA announced the draft documents in June 2018 and is still gathering comments on one of the documents. These documents will cover the performance testing, recommended labeling and lubricious coatings. The FDA said these guidance documents provide industry and FDA staff with recommendations on the least burdensome means of assessing the performance of catheters, guidewires and delivery systems submitted in premarket approval applications (PMAs) or 510(k) premarket notifications.
The “Coronary, Peripheral, and Neurovascular Guidewires - Performance Tests and Recommended Labeling” draft guidance provides draft recommendations for 510(k) submissions for certain guidewires intended for use in the coronary, peripheral and neurovasculature. This draft guidance includes recommendations for descriptive characteristics, labeling, biocompatibility, sterility, non-clinical testing and animal/clinical performance testing. When finalized, this guidance will supersede the 1995 Coronary and Cerebrovascular Guidewire Guidance.
The “Intravascular Catheters, Wires, and Delivery Systems with Lubricious Coatings - Labeling Considerations” draft guidance addresses labeling considerations for devices containing lubricious coatings used in the vasculature, some of which are also within the scope of the above-referenced guidewire guidance. The guidance recommendations are based on information received and analyzed by FDA concerning serious adverse events associated with hydrophilic and/or hydrophobic coatings separating from intravascular medical devices. For more details, see FDA Safety Communication for Lubricious Coating Separation from Intravascular Medical Devices issued on Nov. 23, 2015. This guidance document is intended to enhance the consistency of coating-related information in marketing submissions as well as promote the safe use of these devices in the clinical setting, the FDA said.
Nitinol Safety Concerns Raised by FDA
In April 2019, the FDA published a draft guidance titled, “Technical Considerations for Non-Clinical Assessment of Medical Devices Containing Nitinol,” which includes proposed recommendations on what manufacturers should include in their premarket submission of a device containing nitinol. Nitinol is an alloy of nickel and titanium that is commonly used in guide wires, stents and other medical devices. The recommendations include testing to evaluate susceptibility to corrosion, biocompatibility and performance under certain conditions of stress/strain or temperature, labeling — including language about the risk of potential allergic reactions to the metals — information on how the device is manufactured and other factors that could affect the breakdown of the material in the body.
Earlier this year, the FDA announced a broad effort to engage the public, scientists and industry stakeholders to gather information about medical device materials. The goal of the effort is to ensure the current state of the science is reflected in agency decision-making, to identify any critical gaps in the existing science that need to be addressed, and to determine what approaches should be considered to further understanding of the materials and improve the safety of devices for patients.
“The materials used in devices are important, both to the function of the device and to the safety of the device because of how the human body may respond to the materials used. That’s why we’ve committed to taking steps to advance the science underlying the effects of specific materials, including nitinol, to inform our evaluation of devices and support the development of screening tools to assess potential health risks to individual patients,” said Jeff Shuren, M.D., J.D., director of the FDA’s Center for Devices and Radiological Health. “Nitinol has unique properties that have led to an increase in its use in devices – particularly for orthopedic fracture fixation, cardiovascular stents, guidewires and other devices used in minimally-invasive medical procedures. Devices made with nitinol provide many important benefits to patients, but we need to be able to assess whether, among other things, there are any health risks when the material comes into contact with various parts of the body for extended periods of time."
Related Interventional Guidewire Content:
Understanding the Design and Function of Guidewire Technology
VIDEO: Selecting Workhorse CTO Wires — Interview with Interview with Kevin Rogers, M.D.
VIDEO: Basics of Interventional Guidewire Design and Function — Interview with Dimitri Karmpaliotis, M.D.
The Basics of Guide Wire Technology
VIDEO: The Evolution of Complex PCI at University of Colorado — Interview with John Messenger, M.D., and Kevin Rogers, M.D.
VIDEO: How to Treat CTOs and Complex PCI Cases — Interview with Khaldoon Alaswad, M.D.
Guidewire Product Comparison Chart — create free login to access
VIDEO: New Technology to Treat Chronic Total Occlusions (CTOs) — Interview with Farouc Jaffer, M.D.
VIDEO: Treating Chronic Total Occlusions — Interview with Bill Lombardi, M.D.





 May 13, 2026
May 13, 2026 









