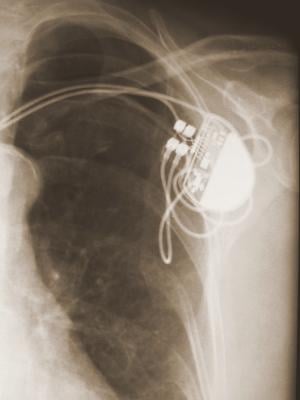
October 3, 2013 — Devices like pacemakers and defibrillators allow doctors to introduce electrical signals to set patients' hearts at regularly timed beats. However, these small mechanical devices come with risks.
"It's like using a cannon to kill an ant," said Leon Esterowitz, director of the National Science Foundation's Directorate for Engineering's Biophotonics program, which funds this research through the Living Matter Lab at Stanford.
Patients must undergo invasive surgical procedures to permanently implant the devices, which can cause cardiac tissue damage. There are other challenges too, such as lifestyle limitations and the occasional battery malfunction. Doctors and patients agree there must be a better solution.
"I think progress has to happen," said Ryan Aleong, cardiologist, University of Colorado Denver. "I think we all realize there's going to be a move for more translational medicine to solve some of these problems."
The Aid of Light
That's where Oscar Abilez, M.D., Ph.D., comes in. He's working with a team of Stanford scientists to develop a biological pacemaker that controls the human heart with light.
The project, Optogenetic Control of the Human Heart—Turning Light into Force, received $600,000 from the National Science Foundation last year. Along with NSF's Biophotonics program, the Biomechanics and Mechanobiology program and the Mechanics of Materials program in NSF's Engineering Directorate co-fund the research.
Abilez's research involves two seemingly disconnected and developing technologies: optogenetics and stem cells. Optogenetics uses techniques from both optics and genetics to control the activity of individual neurons in living tissue.
Optogenetics has huge implications for medicine. Researchers, for example, already have shown that they can stop a seizure, cure anxiety and even implant fake memories into the minds of mice using the technology.
Shining a Light on Someone's Chest
Abilez's would like to take stem cells from a person suffering from cardiac arrhythmia and convert the cells into light sensitive cardiomyocytes. The cardiomyocytes would then be grafted onto a person's heart, thus allowing doctors to control the whole heart's rhythm using light.
"The applications can be of very high reward," said Natalia Trayanova, Ph.D. and director of John Hopkins University's Computational Cardiology Lab. "Wouldn't it be nice to be able to shine a light on someone's chest and defibrillate them painlessly?"
Abilez’s next step is to test whether the lab-grown cells are accepted when coupled with a larger body of non-stem cell derived heart cells. If they are, then Abilez will be on his way to creating a less invasive, longer lasting and glitch-free treatment for arrhythmias.
Additionally, if Abilez can successfully couple light-sensitive cells with normal cells, then his method of creating light-sensitive stem cells could be used by other researchers to grow any type of light-sensitive cell they wanted, from neurons to pancreatic cells, magnifying the applications of optogenetics.
Optogenetic Hurdles
Cardiac optogenetics offers a relatively complication-free treatment for patients.
However, there still are risks involved in cardiac optogenetics. Such risks exist not with the treatment itself but with the feasibility of its development. That is to say, there are still major hurdles to overcome before any applications can be realized.
Ronald Berger, M.D., Ph.D. and professor of medicine at John Hopkins University, is concerned that biological pacemakers might not be able to coordinate electrical activity between the atria and the ventricles. Abilez acknowledges such risk and said there is a chance the team will discover their light-sensitive stem cells cannot control the heart as well as they hope. A large part of the research's difficulty is that the team is in uncharted waters—they have no prior research on which to base their efforts.
"We have to invent things along the way. We don't have any precedent," said Abilez.
Computer Models Reduce Uncertainty
Ellen Kuhl, Ph.D. and director of Stanford's Living Matter Lab is helping to take out some of the uncertainty by creating computer models that simulate the heart under different conditions. With her models, Kuhl has been able to predict optimal configurations for the gene expression of opsins, how much light needs to be shined on the cardiomyocytes and where in the heart, cells should be implanted. She can predict all of this for hearts of varied sizes and ages.
"Computational models can help interpret observations in the complex cardiac setting and can guide future developments," said Emilia Entcheva, Ph.D., professor of biomechanical engineering at Stony Brook University and colleague of Trayanova. "We can make physical or experimental models of arrhythmia and use those as a platform to test drugs to see which drugs are effective in stopping arrhythmias."
“While the applications of cardiac optogenetics are far-reaching, the field has been slow to develop. This is in part because interest in the technology started just as the scientific community began to feel the effects of the recession.”
"NSF support will be a great incentive for more cardiac researchers to focus on fundamental questions that can elevate the use of optogenetics in electrophysiology and cell signaling.”
The researchers estimate the main applications of cardiac optogenetics will be realized in the next ten years to fifteen years.

 April 24, 2026
April 24, 2026 









