The cardiovascular service line, whether existing within the confines of an acute-care environment or outpatient setting, is a myriad of complex systems all delivering their own flavor of data used for diagnosis and treatment planning. While medical images are important to the workflow in this service line, they are used as a correlate to a variety of other types of data. I heard it best said that radiology primarily utilizes the visualization of the medical image while cardiology uses the merging of different data, with images being important but playing second fiddle.
This article is designed to provide an understanding of the different components of a modern cardiovascular information system (CVIS). We must start by differentiating between a CVIS and a cardiology picture archiving and communication system (CPACS) immediately. The point in the paragraph above defines the two as different in that a CPACS tends to be thought of as images first, where in the CVIS is data first. We will break this discussion down into sections for ease of readership, but all sections are of equal importance when considering the selection and implementation of a new-generation CVIS platform. The sections for this article will be:
- Clinical functionality and reporting modules of a CVIS;
- Integration of systems upstream and downstream;
- Electronic health record (EHR) cardiology modules vs. CVIS; and
- Vendor neutral archive (VNA) in support of CVIS image management.
Watch the video "What to Look for in a New Cardiovascular Information System." Sentara Health in Virginia is going through the process of choosing a new cardiovascular information system and implementing enterprise imaging. Sentara's IT leader shares information on what elements they are looking for and how they plan to wire their system to achieve a new level of interoperability for cardiology.
Clinical Functionality and Reporting Modules of a CVIS
Great effort is underway to minimize the numbers of independent “standalone” systems required to support service lines in the context of the coordinated care continuum. Cardiology is one service line where a variety of “best of breed” systems are thrown together often with very little integration of data. As a result, clinicians’ workflows require them to seek data from these individual systems where a wide range of integration levels can be found. Most often, clinicians trying to deliver coordinated cardiac care must utilize different workstations, graphical user interfaces and sign-on requirements. These are but a few of the workflow disadvantages that surface in a hybrid type of environment. cardiology information system vendors have been evolving the ability to provide the divisional elements of the cardiovascular service line onto a single or very tightly integrated system where all data can be visualized, interpreted and compared using a single sign-on and workstation. The ability for a clinician to sit or stand at “any” workstation to access and view data across the various departments in the CV service line is critical. This not only is true for workstations in and around a hospital, but the system should provide the same functionality to the clinicians remotely.
Vendors in the CVIS space should be able to accommodate, either through a single platform framework or through tight integration, the following viewing and reporting modules in a way that creates a single look. This includes:
- Cardiac and peripheral catheterization (including pediatric);
- Electrophysiology;
- Hemodynamics monitoring and reporting;
- Echocardiography (including pediatric);
- Fetal echocardiography;
- Vascular ultrasound (including pediatric);
- Nuclear cardiology;
- Electrocardiogram (ECG)/stress/Holter management and reporting; and
- Maternal fetal medicine module (if applicable).
Integration of Upstream and Downstream Cardiology Reporting Systems
Billions have been spent nationally on the implementation and use of the electronic medical record (EMR). It is impossible to engage in a CVIS strategy without vetting out the detailed integration requirements with the EMR systems, as both clinical and business data must flow bi-directionally. The integration levels with the EMR vary greatly as organizations determine the preferred data flow. For instance, how much data entered into the hemodynamic system during procedures (medications, etc.) does the organization want to populate into the EMR to ensure a single lookup and longitudinal record? Clinically, a high degree of integration diminishes the errors that accompany dual/manual entry of procedural information. From a business perspective, one should consider how they will need procedural, diagnosis, and other billing information to flow dynamically into the billing system
The CVIS on its own can meet the needs of the cardiovascular service line. But, we can no longer define systems functionality with such a narrow and specified viewpoint. Systems must be able to provide the data functionality required by specialists while facilitating interoperability with enterprise-wide platforms in a way that does not require “work around” processes. Consider the number, types and capabilities of systems up and downstream of the CVIS, which will require or should be considered for integration. Below are a few of the most common systems that would effectively utilize data collected and presented by a cardiac information system solution:
- EMR (both inbound and outbound "bi-directionally");
- Inventory systems for supply par-levels and “just in time” management;
- Billing systems (if not part of the EMR);
- Registry reporting systems (ACC, STS, radiation dose, others);
- Vendor neutral archive (VNA);
- Enterprise clinical reference viewers;
- Enterprise data analytics systems;
- XDS registries; and
- Health information exchanges (HIE).
When we speak of systems integration, we are not only referring to systems that use data developed in the CVIS. We also speak of third-party systems that facilitate advanced capabilities in collaboration with procedures and functions native to the CVIS. Advanced visualization and or analysis in most instances are not inherent to the CVIS although the data produced by these systems should be incorporated into the system and presented to clinicians for review and interpretation. Examples would be:
- Intravascular ultrasound (IVUS);
- 3-D/4-D echo;
- Strain analysis;
- MIP/MPR features (e.g. curved, oblique, orthogonal MPRs);
- Volume measurements; and
- Trending modules (e.g. stenosis, ejection fractions, etc.)
EMR Cardiology Modules vs. CVIS
As stated earlier in this article, organizations have spent billions on the purchase and deployment of the EMR. As such, justifying the costs of the system demands a high use factor and value add. Much discussion surrounds the use of a module or modules of the EMR to manage the reporting in sections of the cardiology service line. This thought is still yet to be fully vetted against the functionality of a full CVIS. The premise is that the documentation and procedural reporting can occur in the EMR rather than establishing an interface from the cardiac information system to the EMR. Populating the procedural report with discrete data into a structured report is not out of the realm of possibilities. This data, including DICOM structured reporting (DSR) data can be pulled as discrete data and populated into a procedural report. The use of structured reporting in cardiology must be a key consideration as it diminishes human-induced error rates and streamlines the flow of data into the procedural report, registry reporting systems and certification bodies such as ICAEL and ICAVL.
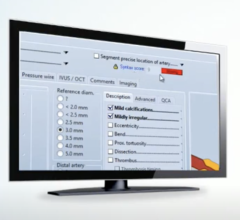
Let us not forget that cardiology uses both data and images to render an opinion and final report. It is not a problem for the EMR to query an image archive for viewing relevant image data. The difference is that a CVIS ensures the discrete data in a report correlates as a presentation state on the procedural image. For example, if the measurement of a stenosis during the diagnostic portion of a cardiac catheterization is measured at 90 percent occlusion, a CVIS reflects this measurement in the report and likewise as a presentation state on the image. Measurements following an intervention adhere to the same workflow. Upon completion of the procedure, a cardiologist will often conduct final review of the report data for approval. At times, the pre- and post-procedural measurements are amended by the cardiologist. If the data fields are amended in the cardiovascular information system, the images immediately reflect the change to ensure both the image and the report are synchronized with the same information. If a cardiologist visualizes the report generated in the EMR module and pulls the images from a separate system to correlate, do post procedural changes on the report trigger changes on the image? Can the EMR report module provide image object change management (IOCM) to ensure the report data matches the presentation state of the image data? This is a critical consideration as it is imperative that the report information perfectly matches the image presentation state.
Furthermore, questions must be raised as to the visibility the EMR will have to data generated by third-party systems or downstream systems such as registry reporting systems. Can the EMR provide rich management reports specific to the cardiovascular service line?
We understand the desire to drive as much activity to the EMR tas possible o justify the cost, but it is important to be diligent regarding the workflow ramifications and stay focused on ensuring the performance is at or above the functionality of a dedicated CVIS.
VNA in Support CVIS Image Management
Vendor neutral archives (VNA) have for some time now been a point of discussion for providing a single archival solution for medical images generated within the organization. The VNA is designed to facilitate the consolidation of disparate archives into an enterprise option. The image data generated from devices in the cardiology service line and used by the CVIS is no exception to this consolidated effort. Medical image data generated in the cardiovascular service line can be archived and managed at the VNA. This architecture simplifies image access through the EMR as a single integration point. Otherwise, visualization of image data would require developing multiple EMR integration points to the variety of image producing systems throughout the organization. The VNA also can be accompanied by a universal clinical viewer to facilitate viewing of the consolidated image data through the EMR.
The modern CVIS has made great strides to incorporate functionality across the entire service line into a single system. There will always be a component of third-party systems integration for either advanced visualization or post-processing software, but the days of “best of breed” are diminishing. Organizations are seeking to shrink the number of independently implemented and supported systems. The cardiovascular service line is one that can benefit from this consolidation. It improves clinician’s workflow, lowers the cost of individual systems care and feeding and creates a unified platform for integration to enterprise systems like the EMR and VNA.
Watch the video "What to Look for in CVIS and PACS Workflow Efficiency." This includes examples of technologies on the market and a discussion of what to look for in workflow efficiencies with Ascendian Healthcare Consultant Jef Williams. Editor Dave Fornell takes viewers on a tour of key workflow improvements offered by health IT vendors at HIMSS 2016.
Link to GE Healthcare's Interactive, Digital Guide for Centricity Cardio Enterprise
Editor’s note: Shawn McKenzie is the president and CEO of Ascendian Healthcare Consulting. He is a national speaker and frequent contributing author on the subjects of healthcare reform, policy, delivery shift and information technology. He can be contacted at [email protected].
Val Kapitula, RT(R), CRT, PMP, is a senior consultant at Ascendian Healthcare Consulting. He is a frequent contributor to publications and forums focused on cardiovascular operations, services and HIT innovation. (Update 2020, Val is now a consultant at Paragon healthcare IT consulting https://pcpimaging.com/about/.)


 November 06, 2025
November 06, 2025