
Results from study of more than 14,000 patients across the United States show the heavy impact of cardiac disease on hospitalized COVID patients. COVID-19 patients with cardiovascular diseases have in-hospital mortality rates of between 25 to 38 percent.
November 18, 2020 — A late-breaking study at the 2020 American Heart Association (AHA) Scientific Sessions showed nearly 20,000 patients revealed that cardiovascular disease (CVD) risk factors in COVID-19 (SARS-CoV-2) patients dramatically increased the risk of in-hospital mortality. The risk of death was particularly high for older, nonwhite men.
To date, information on outcomes of patients hospitalized with COVID-19 has come from outside the United States or from single-institution case series, limiting the understanding in the broader community. Earlier estimates from the first wave of COVID last spring found patients with heart disease who contracted COVID had mortality rates of 10 percent or more, and heart disease appeared to be the co-morbitity with the highest mortality rate among COVID patients. This study confirms that heart disease is a major driver for greatly increasing in-hospital mortality.
Ann Marie Navar, M.D., Ph.D., reported she research team studied electronic health records from 54 health systems that use a COVID-19 database provided by Cerner, a health information technology firm.
The results, measured from January to May and shared in “Impact of Cardiovascular Disease on Outcomes Among Hospitalized COVID-19 Patients: Results From >14,000 Patients Across the U.S.,” showed that in-hospital mortality ranged from 28.5 percent for patients with hypertension to 28.6 percent for those with diabetes, 25.5 percent for those with coronary artery disease, and 38.4 percent for those with heart failure.[1]
Just 1.5 percent of the patients had a stroke while hospitalized for COVID-19, but the mortality rate was 56 percent among this group. Similarly, 5 percent of patients had a heart attack, and 55.5 percent of these individuals died during their hospital stay.
In this large analysis of COVID patient hospitalized at 50+ U.S. health systems, older age, male sex, non-white race, and prior CVD or CVD risk factors conferring the higher risks for in-hospital mortality. While CVD and thrombotic complications were infrequent, those with complications had extremely high risk of death.
“These data reflect what doctors and nurses on the front lines in hospitals across the U.S. are actually seeing, where more than 1 in 15 patients hospitalized with COVID-19 does not make it home,” Navar explained.
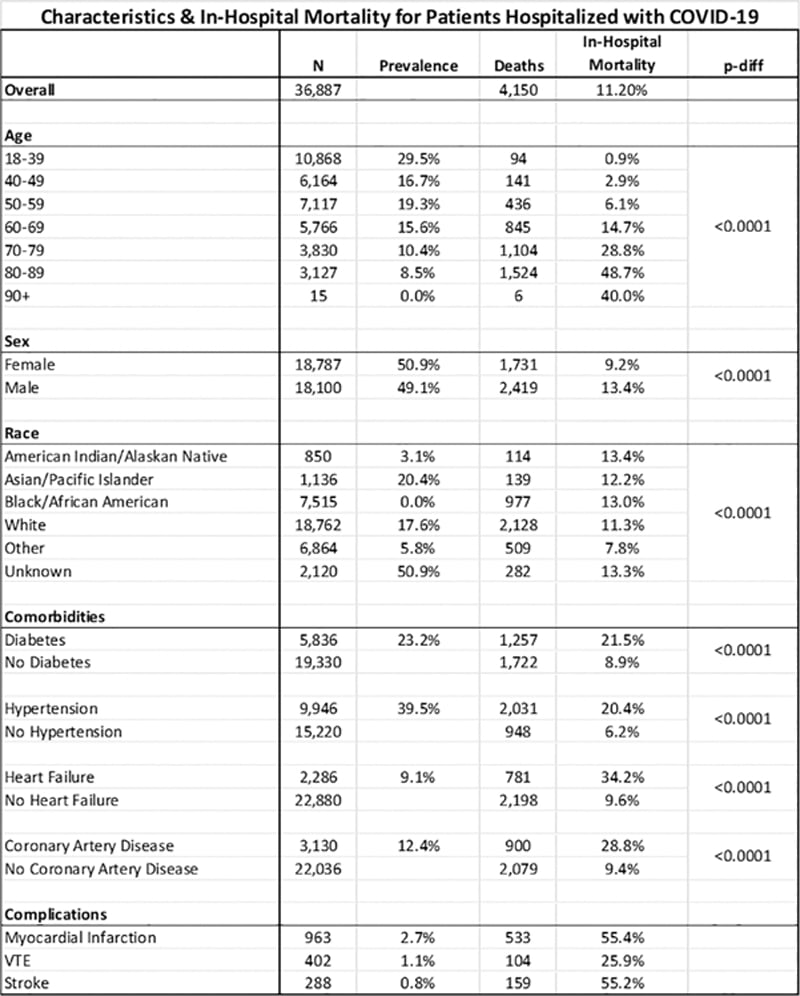
Study results of COVID in-hospital mortality rates by race, age, sex, complications and cardiovascular comorbidities. [1]
She conducted the research at the Duke Clinical Research Institute before joining UT Southwestern as an associate professor of internal medicine and population and data sciences.
Authors: Ann Marie Navar, Duke Clinical Res Inst, Durham, NC; Robert Taylor, Stacey Purinton, Qingjiang Hou, Cerner Corp, Kansas City, MO; Eric D Peterson, Duke Clinical Res Inst, Durham, NC
Navar is a consultant for Cerner and is an uncompensated research principal investigator with the firm.
Related Cardiac COVID-19 Content:
COVID-19 Cardiovascular Registry Details Disparities Among Hospitalized Patients — Another AHA 2020 late-breaking study
VIDEO: Lingering Myocardial Involvement After COVID-19 Infection — Interview with Aaron Baggish, M.D. on AHA discussion on this topic
COVID-19 Positive STEMI Patients Have Higher Mortality
VIDEO: How to Reduce COVID Exposure, Speed Exams and Cut Readmissions in Cardiology Departments— Interview with Keith Ellis, M.D.,
VIDEO: ECMO Hemodynamic Support Effective in Sickest COVID-19 Patients — Interview with Ryan Barbaro, M.D.
The Cardiovascular Impact of COVID-19
VIDEO: Telemedicine in Cardiology and Medical Imaging During COVID-19 — Interview with Regina Druz, M.D.
VIDEO: COVID-19 Precautions for Cardiac Imaging — Interview with Stephen Bloom, M.D.,
Find more cardiology related COVID-19 content
Reference:


 November 14, 2025
November 14, 2025 









