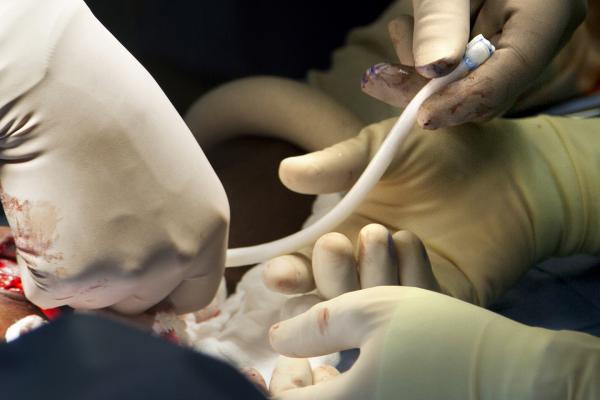
January 2, 2014 — An investigational, manmade blood vessel used in
vascular grafts for kidney dialysis patients may potentially show encouraging early results among study patients in Poland, according to preliminary data reported by a researcher at Duke Medicine.
Presented at the American Heart Association Scientific Sessions meeting in Dallas, the early findings of the interim patient data track 28 hemodialysis patients who received grafts using the investigational bioengineered vessel during a multicenter
study launched December 2012 in Poland.
The investigational bioengineered blood vessel was designed to be the first off-the-shelf product incorporating human tissue in the bioengineering process and provides blood flow in 100 percent of the study patients, reported Jeffrey Lawson, M.D., Ph.D., professor of surgery and pathology, Duke University School of Medicine. Eight patients later lost blood flow, but it was restored with interventions in each case.
Lawson said there is a significant need for alternative types of vascular technology. Current synthetic vascular grafts used for hemodialysis access provide initial blood flood in less than 50 percent of patients at six months, and with secondary interventions the success rates rises to 77 percent, Lawson said.
To date, preliminary interim analysis of the investigational bioengineered vessel currently being used for dialysis among the Polish patients has shown no infections, immune reactions or sign of structural degeneration.
“These early data are very encouraging,” said Lawson, who performed the first U.S. implantation of the blood vessel in June in a patient with end-stage kidney disease. “Longer term evaluations in a larger patient population are needed to confirm the early findings, but we are hopeful the technology continues to demonstrate potential benefit to dialysis patients.”
The investigational bioengineered blood vessel is manufactured by Humacyte Inc., a Duke University spinoff company from the lab of Laura Niklason, M.D., Ph.D., vice chair of anesthesia and professor of biomedical engineering, Yale University. Lawson has collaborated with Niklason and Humacyte for over 15 years to develop the bioengineered vessels.
The technology uses donated human tissue that grows on a biodegradable tubular scaffold, which gradually dissolves as the cells grow. The resulting vessel is then rinsed of its cellular properties, creating a collagen structure that does not appear in preliminary studies to trigger an immune response when implanted in humans. If established in future studies, the feature could enable the technology to be mass-produced without tailoring it to individual patients.
The investigational bioengineered vessel is being tested initially as a vascular graft for patients with end-stage kidney disease who need dialysis procedures. An estimated 380,000 people in the United States receive dialysis, and costs associated with vein access complications are significant.
Subject to review and approval from regulatory agencies, subsequent tests of the technology are planned for replacement or bypass of diseased and injured blood vessels.
For more information: www.dukemedicine.org, my.americanheart.org