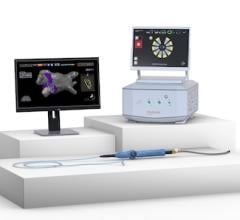
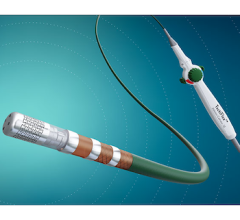
November 24, 2008 - Biosense Webster Inc. last week said the Circulatory System Devices Panel of the FDA unanimously recommended approval of the company’s pre-market approval (PMA) supplement for the NaviStar ThermoCool Catheter for the treatment of symptomatic paroxysmal atrial fibrillation.
The NaviStar ThermoCool Catheter is the first ablation catheter to be recommended by the panel for FDA approval.
Atrial fibrillation, or AFib as it is more commonly referred to, is the most prevalent cardiac arrhythmia and one of the most common causes of stroke.
Conditions for approval recommended by the review panel include a post-marketing registry and a physician education program about use of the product.
Currently, there are no ablation catheters approved for marketing by the FDA for the treatment of AFib in the U.S. Biosense Webster requested expanding the current label for the NaviStar ThermoCool Catheter to include an indication for drug refractory symptomatic paroxysmal AFib. The catheter is currently approved in the U.S. for the treatment of Type 1 atrial flutter, and recurrent drug/device refractory sustained monomorphic ventricular tachycardia due to prior myocardial infarction. Atrial flutter and ventricular tachycardia are two types of cardiac arrhythmia.
The panel’s unanimous recommendation was based on results from a multicenter study comparing catheter ablation to drug therapy for the treatment of Afib. In this randomized clinical trial, catheter ablation was shown to significantly outperform anti-arrhythmic drug (AAD) therapy for the treatment of symptomatic paroxysmal AFib. Patients receiving cardiac ablation with the NaviStar ThermoCool Catheter, manufactured by Biosense Webster were significantly more likely to be free of recurring AFib and experienced fewer serious adverse events than those receiving AAD therapy, the trial found.
This clinical trial was a randomized, unblinded and controlled evaluation of symptomatic, paroxysmal AFib patients who were refractory to at least one AAD and had at least three episodes of AFib in the six months prior to randomization. A total of 167 patients were enrolled from 19 sites throughout the world and the primary effectiveness endpoint (chronic success) was freedom from documented symptomatic AFib recurrence following procedural endpoint confirmation and absent new AAD use or repeat ablation outside of protocol-defined criteria.
The probability of chronic success was 62.7 percent for patients receiving NaviStar ThermoCool Catheter ablation at end of the nine-month effectiveness evaluation period, which is significantly superior to the 17.2 percent probability for the group of patients treated with AAD. The NaviStar ThermoCool Catheter ablation group also demonstrated a substantial reduction in symptomatic AFib recurrence compared with patients treated with AAD (75 vs 21 percent).
For more information: www.biosensewebster.com


 April 29, 2026
April 29, 2026