May 14, 2018 — A significant update to the PROGRESS-CTO (PROspective Global Registry for the Study of Chronic Total Occlusion Intervention) International Registry was presented as late-breaking clinical science at 2018 Society for Cardiovascular Angiography and Interventions (SCAI) Scientific Sessions. The study includes results of Chronic Total Occlusion Percutaneous Intervention (CTO PCI) for more than 3,000 patients across 20 centers in the United States, Europe, and Russia. The new data from the PROGRESS-CTO registry are representative of contemporary practice and outcomes.
The World Health Organization (WHO) estimates that 7.3 million deaths around the world are due to coronary heart disease making it the second cause of death in people under the age of 59 after HIV/AIDS, and reaching the first position in those 60 years and older.[1] Approximately 20 percent of such patients are known to have a complication from CAD called CTO, or complete blockages of the arteries that have typically been present for more than three months.[2] CTO PCI is a minimally invasive procedure that has been evolving with constant improvement of equipment and techniques.
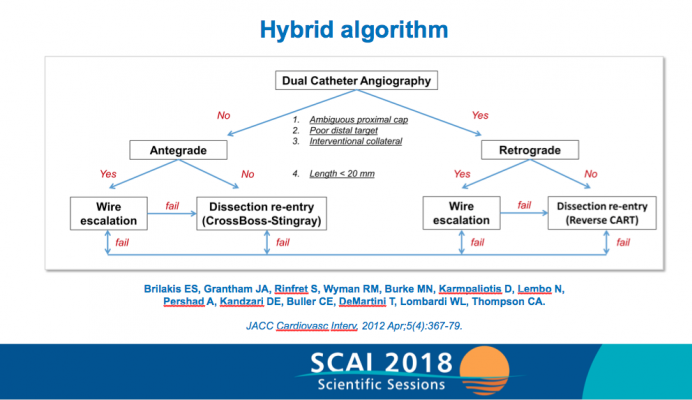
The authors outline contemporary outcomes of CTO PCI by analyzing the clinical, angiographic and procedural characteristics of 3,122 CTO interventions performed in 3,055 patients at 20 centers in the United States (17), Europe (2) and Russia (1). The researchers analyzed success rates of antegrade wire escalation, antegrade dissection and re-entry and the retrograde approach on CTO interventions performed.
The mean age was 65 (plus or minus 10 years) and 85 percent of the patients were men with high prevalence of diabetes (43 percent), prior myocardial infarction (MI) (46 percent), prior coronary artery bypass graft surgery (33 percent) and prior PCI (65 percent). The overall technical and procedural success rate was 87 percent and 85 percent, respectively. The rate of in-hospital major complications was 3 percent (composite of death 0.9 percent), acute MI (1.1 percent), stroke (0.3 percent), tamponade (0.9 percent), emergency surgery (0.2 percent) and re-PCI (0.4 percent). The success rates for the antegrade wire escalation, antegrade dissection and re-entry and retrograde approach were 87.3 percent, 89.7 percent and 83 percent, respectively.
“The high success and acceptable complication rates suggest that at experienced centers CTO PCI can provide significant clinical benefits to the patients,” said Peter Tajti, M.D., Abbott Northwestern Hospital, Minneapolis Heart Institute. “The study results can facilitate discussions with both patients and physicians about the risk to benefits of the procedure and guide decision making on CTO PCI.”
The authors are working on a new, multi-center study including centers from around the world to further assess the effect of CTO PCI symptoms when compared to the placebo-controlled procedure.
This study is published online by JACC: Cardiovascular Interventions.[3]
Complete listing of SCAI 2018 late-breaking trials with links to articles.
Read more on CTO Therapies:
VIDEO: New Technology to Treat Chronic Total Occlusions (CTOs) — interview with Farouc Jaffer, M.D., Ph.D., director of coronary interventions at Massachusetts General Hospital
VIDEO: Treating Chronic Total Occlusions — interview with Bill Lombardi, M.D., director of complex coronary artery interventions at the University of Washington
References:


 May 06, 2026
May 06, 2026 









