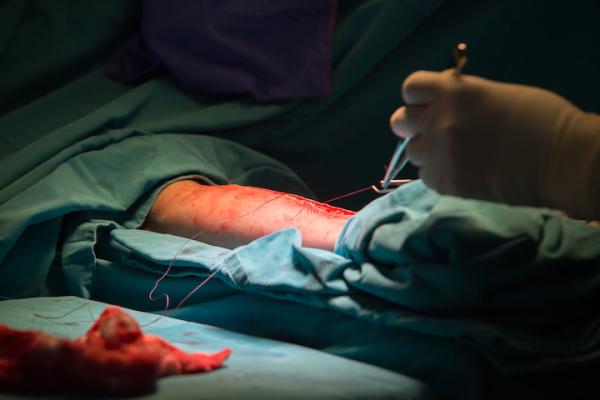
Closing access to the radial artery after harvesting a section of the artery for a coronary artery bypass graft (CABG). Photo by Getty Images.
March 30, 2020 — Patients undergoing coronary bypass graft (CAGB) surgery lived longer and had better outcomes when surgeons used a segment of the radial artery from their arm, instead a saphenous vein from their leg, according to research presented at the American College of Cardiology (ACC) 2020 Scientific Session.
After 10 years of follow-up, data showed that using the radial artery rather than the saphenous vein was associated with a statistically significant decrease in the combined rate of deaths, heart attacks and repeat revascularization procedures, said Mario Gaudino, M.D., professor of cardiothoracic surgery at Weill Cornell Medicine in New York and principal investigator for the study. There was also a significantly lower incidence of the combined endpoint of deaths and heart attacks.
“The choice of an artery or a vein to create the second bypass is one of the most important unresolved questions in contemporary bypass surgery,” Gaudino said. “This study offers the first evidence from randomized trials to show that patients live longer and have better outcomes when surgeons use the radial artery instead of the saphenous vein to create the second bypass.”
Bypass surgery, also known as coronary artery bypass graft surgery or CABG, is the most frequently performed heart operation in adults, accounting for about 60% of all heart surgeries performed annually in adults in the U.S. A section of an artery in the chest is used to create a “detour” for blood to flow around a blocked coronary artery (one that carries blood to the heart).
When multiple bypasses are needed, most heart surgeons use the saphenous vein from the leg to create most of them, Gaudino said. Yet consensus guidelines in both the U.S. and Europe recommend using arteries instead of the saphenous vein. Findings from observational studies have suggested that patients do better and that bypasses created using the radial artery last longer than those that use the saphenous vein.
Most heart surgeons, however, have resisted switching to the radial or other arteries because doing so would add some time and complexity to the heart bypass operation, Gaudino said. Until now, no clinical trials have definitively shown that patient outcomes are better when the radial artery is used, he added.
For the RADIAL study, Gaudino and his team combined the results from five trials in which patients receiving bypass surgery were randomly assigned to get a second bypass from either the radial artery or the saphenous vein. The trials enrolled a total of 1,036 patients whose average age at the time of their surgery was 67 years, and 70% were men. The trials were performed in five countries: Australia, Korea, Italy, Serbia and the United Kingdom. The primary endpoint was the combined rate of death, heart attack or need for a second procedure to treat the same artery. The co-primary endpoint was the combined rate of death or a heart attack.
In results reported in the New England Journal of Medicine in 2018, Gaudino and his team found that after an average of five years of follow-up, patients who received radial artery vs. saphenous vein bypasses had significantly fewer heart attacks and repeat procedures to open a blocked artery, but the death rate was similar in the two groups.
The current study includes an additional five years of follow-up from patients enrolled in the original trials. After a median of 10 years, patients who received radial artery vs. saphenous vein bypasses had about a 23% reduced risk of experiencing the primary or secondary endpoint event. Use of the radial artery was associated with about a 27% reduction in deaths, a 26% reduction in heart attacks and a 38% reduction in repeat procedures. Women appear to benefit the most from the use of the radial artery.
The study is limited in that the results are from a pooled analysis of several small trials rather than one large trial, and the number of patients was relatively small, Gaudino said.
“Our overall sample size of just over 1,000 patients is fairly small, especially considering that bypass surgery is such a widely performed operation,” he said. “These results are important, but they do not give us a final answer. We need a large randomized trial to confirm these findings.”
Gaudino said he hopes that this confirmation will come from the ongoing ROMA trial, of which he is the lead investigator. This international trial aims to enroll 4,300 patients undergoing bypass surgery in centers all around the world. It will test whether outcomes are better for patients who receive two or more arterial bypasses compared with patients who receive just one. Initial results are expected in about five years.
Read an overview of the STS meeting by Mario Gaudino, M.D. — 5 Key Presentations at the Society of Thoracic Surgeons Annual 2019 Meeting
ACC 2020 Late-breaking Studies
Find more news and video from ACC 2020


 April 02, 2026
April 02, 2026 









