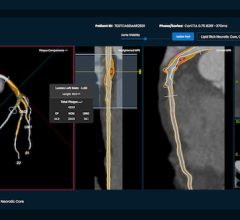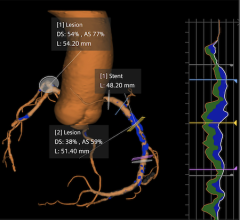
Obstructed LIMA graft as identified by 64-slice CVCT angiography
An asymptomatic 75-year-old woman with a history of coronary artery disease, angioplasty, coronary artery bypass grafting, hypertension and hyperlipidemia was referred for 64-slice cardiovascular computed tomography (CVCT) three months post bypass. A Persantine myocardial perfusion study had been conducted one week prior to CVCT to assess graft patency.
On April 22, 2005 the patient underwent diagnostic catheter angiography for suspicion of recurrent coronary artery disease. Diagnostic angiography revealed severe three-vessel coronary artery disease (90 percent left anterior descending, 90 percent right coronary artery and 100 percent circumflex). A surgical consult was obtained and coronary artery bypass grafting was performed two weeks later.
Three grafts were placed: saphenous vein graft to the posterior descending artery, saphenous vein graft to the obtuse marginal branch of the circumflex artery and a left internal mammary artery (LIMA) graft to the left anterior descending artery, with good result.
A myocardial perfusion study was ordered at three months post bypass surgery to assess graft patency. Due to orthopedic limitations, this patient was administered a Persantine myocardial perfusion study on Aug. 8.
The pharmacological stress test was performed by using 0.56 mg dipyridamole IV over four minutes. The resting heart rate was 66 bpm, and the resting blood pressure was 142/70. At the end of infusion, the heart rate was 76 bpm, and the blood pressure was 120/64. The patient was injected with 14.5 mCi of Techntium-99m Sestamibi (Cardiolite) for the rest images and 43.1 mCi of Technetium-99m Sestamibi for the stress images.
Results of the Persantine myocardial perfusion study included a normal sinus rhythm resting electrocardiogram with normal axis deviation and small insignificant inferior T waves noted. During peak stress, no significant ST-T segment shifts were noted.
The Persantine myocardial perfusion study was completed without electrocardiographic clinical ischemia. Preserved left ventricular systolic function was noted with an estimated gated ejection fraction of 69 percent. Scintigraphy demonstrated infero-lateral wall ischemia. Based on these results, failure of the saphenous vein graft to the obtuse marginal branch was suspected.
One week later, the patient was administered a CVCT angiographic study to confirm graft patency. After informed consent, nitroglycerine spray was given to optimize image quality; also, 100 cc of Isovue 300 were infused to obtain computed tomography of the cardiac structures with the Siemens Sensation 64-slice scanner.
A volume data set was acquired (64 x 0.6-mm collimation, gantry rotation time 330 ms, pitch .2 mm, tube voltage of 120 kV), covering the distance from the carina to the diaphragmal face of the heart. Cross-sectional images were reconstructed with a slice thickness of .75 mm overlapping in 0.4 mm intervals with the use of an electrocardiogram gated half-scan reconstruction algorithm to obtain an image acquisition window of 164 ms.
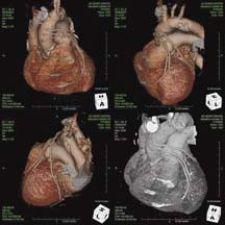
Results of the CVCT procedure demonstrated the presence of apical thinning, which may reflect a myocardial scar. Left ventricular size and wall thickness appeared normal. The left atrium was enlarged and left ventricular systolic function was decreased with ejection fraction estimated at 50 percent with anterior wall hypokinesis.
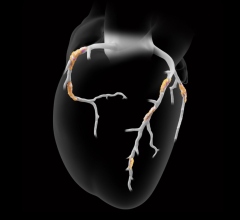
The LIMA graft was anastomosed to the left anterior descending artery and was thin and threadlike. There was no flow observed through the LIMA graft. The two recently placed saphenous vein grafts were occluded at their origin.
Thus, all bypass grafts appeared significantly compromised at three months post bypass surgery in this patient absent of typical symptoms.
Is a Change Needed?
This case suggests that a paradigm shift in post-bypass imaging protocols may be warranted. The relative lack of motion when imaging bypass grafts via CVCT angiography results in exceptionally high-quality images of diagnostic quality in virtually all patients.
Our experiences, along with recent contributions to the literature, have suggested that CVCT angiography is an efficacious, efficient and safe method of assessing coronary graft patency. 1-5
We suggest that early silent graft occlusions may be better identified via CVCT imaging than by traditional perfusion studies. The incidence points of silent graft occlusions have not been accurately established in the literature. Research utilizing 64-slice CVCT could clarify the uncertainty surrounding the timeframe to initiate assessment of graft patency as well as the imaging modality, which is most reliable in the identification of coronary graft occlusions.6
References
1. Frazier AA, Qureshi F, Read KM, Gilkeson RC, Poston RS, White CS. Coronary artery bypass grafts: Assessment with multidetector CT in the early and late postoperative settings. Radiographics. 2005;25:881-896.
2. Chiurlia E, Menozzi M, Ratti C, Romagnoli R, Modena MG. Follow up of coronary artery bypass graft patients by multislice computed tomography. Am J Cardiol. 2005;95:1094-1097.
3. Herzog C, Wimmer-Greinecker G, Schwarz W, Dogan S, Moritz A, Fichtlscherer S, Vogl TJ. Progress in CT imaging for the cardiac surgeon. Semin Thorac Cardiovasc Surg. 2004;16:242-248.
4. Vignaux O, Paul JF, Duboc D. Multislice CT and MRI of coronary artery disease: Current and future role. J Radiol. 2004;85:1786-1795.
5. Schlosser T, Kornorza T, Hunold P, Kuhl H, Schmermund A, Barkhausen J. Non invasive visualization of coronary artery bypass grafts using 16-detector row computed tomography. J Am Coll Cardiol. 2004;44:1224-1229.
6. Zellweger MJ, Lewin HC, Lai S, Dubois EA, Friedman JD, Germano G, Kang X, Sharir T, Berman DS. When to stress patients after coronary artery bypass surgery? Risk stratification early and late post CABG using stress myocardial perfusion SPECT: Implications of appropriate clinical strategies. J Am Coll Cardiol. 2001;37:144-152.


 April 15, 2026
April 15, 2026