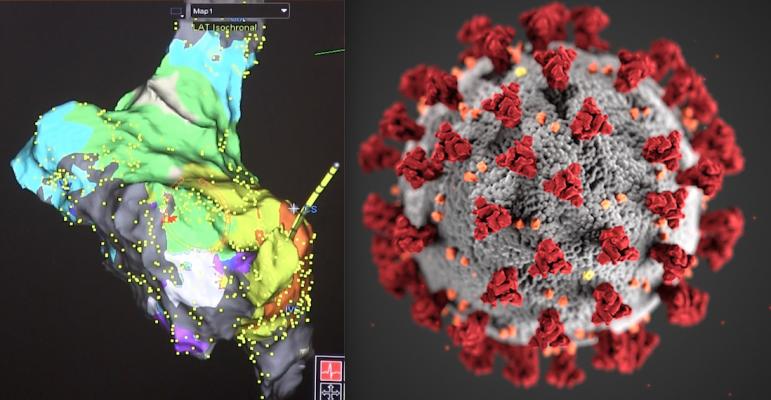
Patients with atrial fibrillation are at far greater risk of a catastrophic COVID outcomes, so steps should be taken to reduce AFib risks in addition to precautions against COVID like making, hand washing and social distancing. Images include an electromap from an AF ablation procedure and a COVID-19 from the CDC.
In our most challenging and distressing days, it is nice to think about a post-COVID-19 world.
But while this pandemic will end at some point, it is quite unlikely that we will completely eradicate the novel coronavirus that causes COVID-19 (SARS-CoV-2) — the way we did, for instance, with the virus that causes smallpox.
Rather, many virologists and public health experts have come to believe, a reasonably effective vaccine will help us reach some degree of herd immunity, and treatments and therapies will continue to reduce suffering, but the virus will likely continue to circulate. And for those who are vulnerable, it will likely continue to be a grave danger.
So, while it can be soothing to think of a world without COVID, we have to prepare and act now as though it will never go away. And this is especially important for those with or at-risk of atrial fibrillation (AFib).
That is a huge group, by the way. For example, the ongoing seven-decade long Framingham Heart Study has shown that the lifetime risk of atrial fibrillation in the United States is as high as one in four.[1] And while there is still much about COVID that we do not know, one thing is already very clear: These individuals are at far greater risk of a catastrophic COVID outcome.
For COVID patients, AFib makes a very bad situation much worse. But it is usually far too late — once patients are on a ventilator, in the ICU, fighting for their lives — to deal with an unchecked arrhythmia, which often isn’t treatable until the underlying issue of COVID is under control. This is why it’s important for care-givers at all levels to “think ahead, protect hearts, and reduce mortality.”
That was the advice one of us offered, alongside colleagues from around the world, based on data coming out of China in the early months of this global pandemic, which clearly showed that newly diagnosed and worsening cardiovascular disease are common complications in COVID-19 patients.[2] Since then, the evidence of a tremendously problematic association has only mounted. In one study led by researchers at the University of Pennsylvania,[3] for instance, ICU-admitted patients with COVID were 10 times more likely to have a significant heart arrhythmias. Now, more than ever, it is vital to take action early, because by the time a patient gets COVID, it may be too late.
Preventing is the Best Medicine in AFib
While there is certainly nothing new about the fact that prevention is always preferable to reactive care, the advent of COVID makes this approach to health and wellness all the more important. And the time to start on the road to preventative wellness is now, for even if you are an optimist about the potential that a vaccine will be approved soon, it may be mid-2021 — or longer — before a vaccine will be widely available.
As we wait, every day a person can avoid infection is another day in which doctors and researchers are learning how to treat COVID, and even how to treat it for individuals with AFib. Thus, the first step is to simply do what public health officials have been advising for a long time, now: Wash your hands frequently. Wear a mask in public. Even when you are wearing a mask, maintain plenty of space from other people. And avoid gatherings.
People who do these things are less likely to get COVID. And the result is more time to work on the things that can be done to lower the risk of a grim outcome if and when an infection does occur.
This begins by addressing the underlying conditions that resulted in AFib in the first place, many of which can be improved in a matter of weeks and months — enough, perhaps, to pull a person away from the “tipping point” in which AFib and COVID combine for drastic outcomes.
Controlling Blood Pressure and Diabetes Key to Helping Control AFib
It may be wise to start with blood pressure. Hypertension not just a cause of AFib for many people — it is also linked to increased risk of mortality in patients with COVID, and may be the most prevalent comorbidity in patients hospitalized for the disease, according to research presented at the American Heart Association Hypertension Scientific Sessions.[4] Thus, it makes sense that getting blood pressure under control as soon as possible is a key preventative strategy.
The second-most prevalent COVID comorbidity, is diabetes, which is found in 24% of people hospitalized with COVID and in 32% of those that ultimately required treatment in an ICU. Diabetes is one of the most common concomitant diseases in patients with AFib.[5] Thus, a more in-sync metabolism is of vital importance as well. The American Diabetes Association notes that, while people with diabetes face a higher chance of serious COVID complications, “your risk of getting very sick from COVID-19 is likely to be lower if your diabetes is well-managed.”
 One common concern of both COVID and AFib is that each increases your risk of clot formation leading to heart attack and stroke. In both disorders, this risk goes up with the more underlying medical problems you have such as obesity, hypertension, heart failure, diabetes and vascular disease. Unfortunately, when COVID and Afib are combined, there is likely a synergistic effect of risk making your risk of stroke even higher.
One common concern of both COVID and AFib is that each increases your risk of clot formation leading to heart attack and stroke. In both disorders, this risk goes up with the more underlying medical problems you have such as obesity, hypertension, heart failure, diabetes and vascular disease. Unfortunately, when COVID and Afib are combined, there is likely a synergistic effect of risk making your risk of stroke even higher.
Even if a person with AFib does not have hypertension or diabetes, however, the ways to address these concomitant issues is the road toward a better outcome if and when a COVID infection occurs. These are the steps that are covered in our soon-to-be-released book, "The AFib Cure: Get Off Your Medications, Take Control of Your Health, and Add Years to Your Life."
8 Tips to Reduce Atrial Fibrillation Risk
While some of the steps described in the book may take years to achieve, much of the advice can be applied right away — and the effects can be realized right away, thus reducing the risk. This includes:
● Lose weight: The scientific data connecting weight and AFib are so compelling that many electrophysiologists specializing in heart rhythm disorders feel that carrying extra weight is a primary cause of AFib. In fact, our research has shown that even a few extra pounds can make a big difference in a person’s AFib risk and how they respond to treatments—not to mention their much lower risk of a catastrophic COVID complication should they ultimately get infected.
● Get better sleep: The impact of poor sleep on AFib has been well documented. Even small interruptions of sleep quality and duration can increase the risk of atrial fibrillation, and it’s even worse for people with sleep disorders such as sleep apnea, who have up to a 400 percent increased risk of AFib. And good sleep, of course, plays a big role in decreasing hypertension and your susceptibility to a viral infection.
● Optimize stress levels: In a 2014 study published in the Journal of the American College of Cardiology, Dr. Rachel Lampert from Yale University noted that feelings of stress and anxiety, as well as sadness, anger, and impatience, all may increase the risk of an AFib attack up to 500 percent in the same day these negative emotions are experienced. This is especially important given that stress has been well documented to be an important factor in one’s susceptibility to viral illnesses.
● Get more exercise: While endurance sports may be a risk factor for AFib, regular exercise is exceptionally protective. People who live sedentary lifestyles are at significant risk of AFib, not to mention all of the other health consequences of not getting enough exercise which could also put them at increased risk from COVID.
● Avoid alcohol and energy drinks: These are common triggers for AFib. An occasional wine or beer, or sip or two of an energy drink may not be problematic for most people, but a little goes a long way and if the goal is zero AFib then abstinence is the best strategy.
● Avoid sugar and processed carbohydrates: Blood-sugar fluctuations can cause cardiac scarring and may trigger AFib. A reduction in foods loaded with these ingredients can pay big — and fast dividends.
● Keep electrolytes in balance: One study from researchers in The Netherlands showed that low levels of potassium could quadruple the chances of AFib in some individuals. Those experiencing magnesium deficiency are also at considerable risk. Reasonable increases in foods rich in potassium, calcium and magnesium — from spinach to strawberries, from broccoli to bananas, and from tofu to tomatoes — are a good bet right now. So-called “sports drinks” are not.
● Get more vitamin D: Most people know about vitamin D’s role in bone health, but in recent years its other roles have come into better focus—and that includes its association with atrial fibrillation. At a time in which social distancing often means staying inside, it’s all the more important to ensure adequate (but not overabundant) D consumption.
These are all unquestionably good steps to take for anyone who has, or is at risk for, AFib, and who wants to improve their quality of life. But at this particularly tumultuous time in our history, reducing the factors that cause and aggravate AFib is not just about improving a person’s life, and it might very well be a matter of saving it.
About the Authors: Cardiologists John D. Day, M.D., and T. Jared Bunch, M.D., are the authors, with Matthew D. LaPlante, of The AFib Cure: Get Off Your Medications, Take Control of Your Health, and Add Years to Your Life (BenBella Books, February 2021).
Day is director of the Intermountain Heart Institute Heart Rhythm Specialists and is past president of the Heart Rhythm Society (HRS), 2015 – 2016.
Bunch is a professor of medicine at the University of Utah School of Medicine. Prior to that, he served as the medical director of heart rhythm services for Intermountain Healthcare.
References:


 April 14, 2026
April 14, 2026