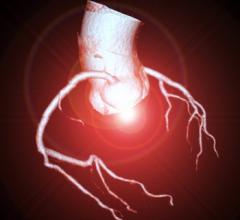
Left, a 3-D rendering of a heart from a cardiac CT exam. Right, a lung-CT exam showing the heart and ground glass lesions in the lungs of a COVID-19 patient. CT has become a front-line imaging modality in the COVID era because it offers both cardiac and lung information to help determine a patients disposition with chest pain, COVID-19 and COVID-caused myocarditis and pulmonary embolism.
July 28, 2020 — The use of cardiovascular computed tomography angiography (CCTA) is one of the areas that has seen a sudden increase in use and value since the start of the ongoing COVID-19 pandemic. While SARS-CoV-2 has had significantly impacted cardiovascular care delivery, with a large reduction in elective diagnostic testing and face-to-face patient care, it also resulted a necessary re-examination of how cardiac care is delivered. Alternative approaches, beyond traditional, entrenched clinical practice for cardiac imaging are discussed in a recent paper published in Radiology: Cardiothoracic Imaging.[1]
"In many ways, the COVID crisis has been like a crucible," the authors of the paper wrote. "Anything that is extraneous or unnecessary, anything that has gone on 'just because' gets melted away, leaving only that which is inherently of value and worth keeping."
The authors said telemedicine is showing cardiologists that not every patient needs to present in-person in order to have meaningful interactions for care. They said the same is true for an expanded clinical role of CCTA in ambulatory and acute care settings has been equally beneficial. However, they argue neither approach will be sustainable in the future unless the regulatory and reimbursement systems for care delivery can adapt to these innovative approaches.
"All of us at all of our institutions that have developed over time that have either been reinforced by culture or payment mechanisms, but what the pandemic has allowed is a sort of rethinking of all of this and stripping things down to what really is effective and works," said one of the study authors Geoffrey Rose, M.D., president of Sanger Heart and Vascular Institute with Atrium Health, in Charlotte, N.C. He explained this includes the use of cardiac CT, point-of-care ultrasound (POCUS) and telemedicine.
Use of CT in the COVID-19 Era
COVID-19 has disrupted traditional cardiovascular care pathways leading to significant challenges. The authors said among these are choosing appropriate tests and best align with infection protection protocols.
Historically, CCTA has been used for triple rule out (TRO) of acute chest pain for the assessment of acute pulmonary embolism, acute coronary syndrome, and acute thoracic aortic dissection. However, during the COVID-19 crisis, the authors said they have added two more critical diagnoses, which include COVID lung infection and acute viral peri-myocarditis.
"We really found CT to emerge as as a front line test for the evaluation of chest pain for patients at intermediate risk, and now even more so in the COVID era with the issues of logistics in testing," Rose explained. "We find the ability to get patients in for a CT and out the door faster, with less contact is particularly well-suited to a COVID environment."
The study authors used a protocol that includes a gated non-contrast scan of the chest for the evaluation of COVID-19 lung disease and a coronary artery calcium score, followed by an ECG synchronized CTA of the heart, heart and aorta, or heart, pulmonary arteries, and aorta.
The clinical role of TRO remains modest, but has been used in patients that have positive d-dimer or high clinical suspicion of having acute pulmonary embolism, the authors wrote. There have been some reports suggesting that a delayed enhancement CT protocol may be helpful in aiding in the diagnosis of COVID myocarditis as has been described previously for other causes of myocarditis. Although cardiac MRI (CMR) is the preferred noninvasive technique for the detection of acute myocarditis and scarring, the clinical access to CMR during the crisis has been very limited, and the lack of direct visualization of the coronary arteries limits the utility.
Instead of using transesophageal echo (TEE), CCTA has also become the noninvasive imaging of choice for the evaluation of the left atrial appendage (LAA) thrombus during COVID-19, the authors wrote. Even in the American Society of Echocardiography (ASE) imaging guidelines under COVID-19, CT is suggested as an alternative, because of the amount of increased viral shed exposure from aerosolization.[2]
Clinical Findings From CCTA in COVID Patients
The authors said they found two positive acute peri-myocarditis cases using their CCTA protocol in 10 known COVID-positive patients. They also used a standard CT protocol that includes wide reconstructed field of view for the evaluation of the pulmonary parenchyma for the evaluation COVID lung disease in patients with cardiac symptoms and elucidating the etiology of atypical chest pain and dysrhythmia. The pulmonary findings have been interpreted in a standardized fashion, as laid out in recent guidance documents.[3]
The challenges were noted with performing CCTA on critically ill COVID-19 patients with fever, shortness of breath and coughing include tachycardia, unable to breath hold and risk of exposing frontline workers to the the virus. For these reasons, some modifications of the routine patient preparation and scanning procedures are often required, the authors wrote.
Prior to COVID-19, many centers have been providing oral heart rate control and beta blockade in triage or holding areas, but with a desire to keep time in the department to a minimum, the authors said their centers expanded use of outpatient pre-beta blockade. Owing to a desire to optimize social distancing, every effort is made to lower the heart rate using a combination of oral beta-blockers a day or two prior to the testing, and intravenous beta blocker on the CT couch to achieve the best images with the least amount radiation exposure possible, in accordance with the Society of Cardiovascular Computed Tomography (SCCT) acquisition guidance.[4,5].
However, high heart rate as a result of fever and systemic infection may render heart rate control with either beta blocker or calcium blocker difficult, the paper stresses. Due to the urgency of the scan, use of wide acquisition windows covering the entirety of the cardiac cycle may be needed to help increase the likelihood of an interpretable scan. During the COVID-19 crisis, the authors also said they received approval from their hospital administration to send CCTA cases from both the emergency departments and inpatient cases off-site to HeartFlow for fractional flow reserve CT (FFR-CT) analysis if needed to improve positive predictive value of the scans and determine if revascularization was really needed to cut unneeded exposure to the cath lab staff.
In the setting of known or highly probable COVID-19, CT may have a role for pre-catheterization evaluation of patients presenting with ST-segment elevation MI (STEMI). The experience in Northern Italy has raised awareness of fulminant COVID-associated myocarditis presenting as STEMI, the authors wrote.
"In all, it is estimated that in the setting of widespread community COVID infection that as many as 60 percent of STEMI presentations may be related to COVID rather than an acute plaque rupture amenable to PCI," the study authors wrote.
Many hospitals are now using point-of-care ultrasound (POCUS) examinations to help determine which patients more likely to have myocarditis because they lack a regional wall motion abnormality. While some have proposed the use of CCTA in advance of invasive catheterization angiograms, for those with suspected COVID infection who present with STEMI, it is important that logistical issues should not delay appropriate care in the patients with true epicardial obstruction, the authors said.
Of particular note, the authors explained that in patients with atypical presentations, CCTA may be particularly helpful where the findings of ST-elevation and transthoracic echocardiography are divergent. The European Society of Cardiology (ESC) has provided guidance regard testing in the COVID environment, where using CT angiography (CTA) is the preferred test to noninvasive functional testing during the pandemic. The guidelines also state that in case CCTA is not possible or available, noninvasive testing should be postponed owing to the close contact between patients and personnel during stress echo exams.[6].
The authors of the paper include Michael Poon and Michael Kim from Lennox Hill Hospital, Northwell Health; Jonathon Leipsic, Center for Heart Lung Innovation, University of British Columbia and St. Paul’s Hospital, Vancouver, Canada; Frederick Welt, University of Utah Health, Salt Lake City; and Geoffrey Rose, Sanger Heart and Vascular Institute, Atrium Health, Charlotte N.C.
Watch a related interview with author Geoffrey Rose, M.D. — VIDEO: CT and POCUS Emerge As Frontline Cardiac Imaging Modalities in COVID-19 Era
Related COVID-19 Cardiology Content:
The Cardiovascular Impact of COVID-19
How Cardiology Dealt With the COVID-19 Surge in New York City
Kawasaki-like Inflammatory Disease Affects Children With COVID-19
New Research Highlights Blood Clot Dangers of COVID-19
VIDEO: Impact of COVID-19 on the Interventional Cardiology Program at Henry Ford Hospital — Interview with William O'Neill, M.D.
ACC COVID-19 Clinical Guidance For the Cardiovascular Care Team
The Cardiac Implications of Novel Coronavirus
Cardiology Stands Up to the COVID-19 Challenge
COVID-19 STEMI Registry Created to Study Acute Cardiovascular Effects of the Virus
How to Manage AMI Patients During the COVID-19 Pandemic
References:
2. James N. Kirkpatrick, Carol Mitchell, Cynthia Taub, et al. ASE Statement on Protection of Patients and Echocardiography Service Providers During the 2019 Novel Coronavirus Outbreak: Endorsed by the American College of Cardiology. American Society of Echocardiography (ASE). https://doi.org/10.1016/j.echo.2020.04.001. Accessed July 26, 2020.
3. Simpson S, Kay F, Abbara S et al. Radiological Society of North America Expert Consensus Statement on Reporting Chest CT Findings Related to COVID-19. Endorsed by the Society of Thoracic Radiology, the American College of Radiology, and RSNA. Radiol Cardiothorac Imaging 2020;2(2):e200152. doi: 10.1148/ryct.2020200152.

 February 06, 2026
February 06, 2026