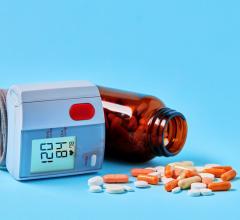
Hand-held bar-coding devices, such as the Symbol 8846, which works with McKesson's Medication Safety Advantage solution, also scan syringes and IVs before they are administered.
Between 44,000 and 98,000 Americans die each year from preventable medical errors, according to the Institute of Medicine’s (IOM) 1999 report. That single fact, along with all the complications associated with it — patient lawsuits, regulatory pressures and media scrutiny — has compelled hospitals to implement new systems to reduce preventable errors, including decreasing errors associated with the administration of medications. According to an American Society of Health-Systems Pharmacists survey, the No. 1 fear of patients entering the hospital is that they will receive wrong medications, further confirming drug safety is a big issue for hospitals.
For many hospitals, bar coding at the bedside is one solution gaining traction since the release of the IOM report, according to hospital officials and industry insiders. Bar coding has replaced what many clinicians describe as inefficient, error-prone manual processes of medication administration, where human errors could occur at several points between a doctor ordering a medication for a patient and a nurse administering that medication.
Bar Coding Medications
Before bar coding can be effective at the bedside point of care, all medications from hospital pharmacies must contain scannable bar codes. Estimates vary, but many medications utilized by hospitals don’t come with bar codes. Mary Beth Navarra-Sirio, a vice-president and patient safety officer with McKesson, estimates only 40 percent of mediations are manufactured with bar codes. Doyle Boykin, vice-president of nursing with Presbyterian Healthcare Services in New Mexico, says since the FDA doesn’t currently mandate standardized bar coding on medications, Presbyterian re-bar codes nearly all its medications to match its bar-coding system.
In order for a hospital pharmacy to be properly equipped for automated medication safety systems, including bar coding, the pharmacy system must have a “clean database,” according to Kris Cervin, F.D., a staff pharmacist at Rice Memorial Hospital in Willmar, MN, who earlier this year helped implement the Omnicell’s SinglePointe, an automated medication dispensing system designed to store all medications. That means making sure all types of medications are found both in the pharmacy database and in the database nurses use to store and administer medications.
One area of medication administration that leaves many systems vulnerable to errors are patient-specific, nonstandard medications, according to Richard Caldwell, MS, RPh, senior product manager, medication systems for Omnicell, and a former associate director of pharmacy services at Stanford Hospital and Clinics in Palo Alto, CA. Roughly 20 percent of medications administered to patients, including home medications, multi-use medications (such as an inhaler) and transfer medications, are a major culprit in potential medication administration errors because of storage issues, according to Caldwell. Many of those medications are not bar coded either.
Once all medications are properly bar coded by the hospital pharmacy and the pharmacy’s system is integrated with the bar-coding system in the nursing units, bedside point-of-care bar coding for medication administration becomes possible.
Bedside Safety
When the IOM report was released, point-of-care bar coding was in its infancy in the U.S. market. After the report was released, several hospitals, including the Beloit Memorial Hospital in Beloit, WI, moved to institute bar coding for medication administration.
Doris Mulder, a vice-president with Beloit Memorial Hospital, says the hospital changed its reporting of medication errors to an anonymous reporting system prior to switching to bar coding in order to get a more accurate picture of the number of medication errors that were occurring. The number of medication errors reported increased “over 100 percent,” Mulder said. Starting in 2003, Beloit moved to institute a bar-coding system manufactured by CareFusion. (Cardinal Health acquired the CareFusion line in 2006.) The reduction of medication administration errors was readily apparent, according to Mulder. She says errors after the first year of bar coding decreased approximately 86 percent.
“We were a little surprised, but very gratified and very happy that the numbers did decrease so dramatically,” Mulder said.
CareFusion’s current bedside point-of-care wireless personal digital assistant (PDA) device, called the CareFusion Medication Administration, is designed to allow nurses and other clinicians scan a patient’s wristband to verify the right patient is given the right drug, in the right dose, at the right time, by the right route of administration. The device is hooked into the CareFusion server and the pharmacy server via a WiFi connection. As a nurse logs into their PDA device using their ID badge, Medication Administration receives data in real time from the pharmacy’s system and provides the nurse an “executive dashboard” for that care area, telling the nurse what medications or tasks are due for each patient.
The nurse collects the appropriate medicines, then makes rounds to each patient to administer them. Before any medicines are given to a patient, the nurse scans the patient’s wristband.
“If it’s not the correct order for that particular patient, there is logic in the software when the provider scans the patient wristband to do the identification,” said Joe Condurso, who oversees the CareFusion unit for Cardinal Health. “The task would be halted or stopped and allow the provider to make an assessment that either it was the wrong order or that the wrong task was going to be executed.”
Boykin reported similar results after implementing several automated McKesson patient-safety systems, including a bedside bar-coding system, at Presbyterian starting in 1999. Before implementing bar coding, Presbyterian conducted an observational study of medication errors. After implementing the bar-coding system, Presbyterian conducted another observational study, which yielded about an 80 percent error reduction rate in medication administration.
“We knew that we had errors just like all organizations who administer medication,” Boykin said. “The results of (the observational study) were pretty eye-opening. It was pretty illuminating for us to realize that this was going on and that we were able to fix it.”
In both cases, successful implementation didn’t come without challenges. Hospital officials admit some staff resisted the changes, even if they were replacing a manual process with an automated one. Having the staff see the viability of the new system quickly helped the Beloit staff to accept the changes.
“It doesn’t take very long in a hospital my size for news to spread quickly, and the first time a nurse was saved from doing a medication error because of the hand-held, that spoke loudly not just to that nurse, but to all the nurses on that unit,” Mulder said.
A technical problem both Beloit and Presbyterian experienced was the screen size of the hand-held PDAs. With the average age of nurses increasing, several nurses had problems reading the small screens.
Scanning patient wristbands proved to be difficult at times. Since wristbands are curved and not flat, scanners don’t always register the band. Presbyterian moved to different type of wristband that is more like a tag to alleviate the problem, said Boykin. Another issue is that patients get water on the bands, which hinders the band’s ability to be scanned.
Implementing Bar Coding
Cervin recommends organizations make it a priority to involve nurses and pharmacists early in the training process. All healthcare workers and manufacturers who spoke with Acuity Care Technology echoed those sentiments.
“We didn’t just have nurses and pharmacists and IS people on our planning team,” Mulder said. “We had people from radiology, people from the lab, the CNAs, the housekeepers all involved. We weren’t sure who all it was going to touch, but we wanted everyone to be involved.”



 January 28, 2026
January 28, 2026