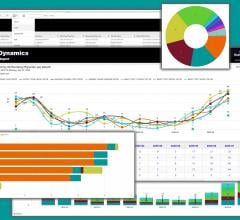
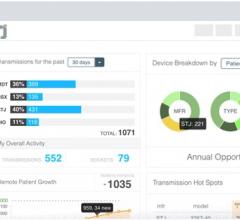
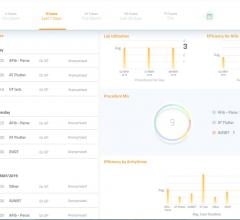
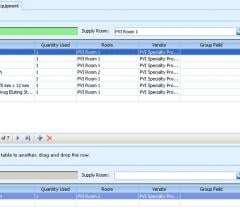
There are numerous factors that impact the larger picture in cardiology, especially from a business perspective. Here are several overarching trends effecting cardiology in 2019 and beyond.
Cardiology Cost Drivers
Reimbursements from the Centers for Medicare and Medicaid Services (CMS) and insurance providers drive trends for the adoption of new technologies. However, new technologies that can show empirical evidence for being able to improve outcomes at lower costs are being moved up for better payments. CMS and other insurers are also using a carrot and stick approach with
increased use of CMS bundled payments. These give a flat fee for diagnosing and treating a heart attack or heart failure, rather than hospitals being paid for all the tests and procedures they did. This approach makes the hospitals want to find new ways to be more cost-effective and to increase their bottom lines to capture more of the bundled payment as revenue.
Heart failure makes up about a third or more of the costs to Medicare. This has caused CMS to look closely at what is driving costs, and really high readmission rates are mainly to blame. There are penalties or no reimbursements for patients who come back for repeat treatments because they were not managed properly the first time. so, new technologies to address heart failure readmissions are of major interest to
hospitals. Many of these include
information technology (IT) solutions, rather than treatment device technologies.
Other conditions like
atrial fibrillation (AF) also drive up costs, so vendors are attempting to find better ways to diagnose and treat this condition. Current treatments are only effective in the first attempt on about 60 percent of patients.
Consolidation of Hospitals and Outside Physicians
This is a continuing trend where single hospitals or smaller hospital systems are being bought up by bigger fish to create economy of scale with larger healthcare systems. These often cover specific geographic areas and often cast a wide net to include some luminary hospitals, smaller community hospitals, immediate care centers and minute clinics inside drug partner pharmacies. Duplicate staff and services are sometimes eliminated after mergers and consolidation. Outside physicians, including cardiologists and radiologists, are also being brought into the fold as employees of the health systems, rather than the old model as outside contractors who have access to the hospital's amenities.
Trends in Cardiovascular Technologies
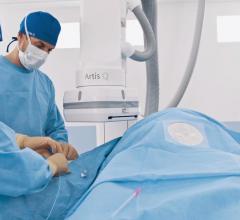
Any techniques and technologies that can improve outcomes, cut costs, reduce hospital length of stay or prevent readmissions can capture hospital and cardiologist attention in today's healthcare environment. There has been a massive movement over the past two decades away from traditional open heart or vascular surgical procedures to catheter-based interventional procedures. This includes improvements in the durability and complexity of percutaneous coronary intervention (PCI), reopening
chronic total occlusions (CTOs),
endovascular aortic repair (EVAR), expanded interest in treating
peripheral artery disease (PAD), and
structural heart cases that used to be the realm of the cardiac surgeon.
There is a major revolution and rapid uptake in
transcatheter valve technologies to replace open heart surgery. Structural heart procedures to repair or replace failing heart valves have had positive clinical trial after positive trial over the last several years. Several key cardiac surgeons in the field say catheter-based interventions will likely be the way of the future and surgical case volumes will see steady declines over the next decade.
The Role of Information Technology and AI in Cardiology
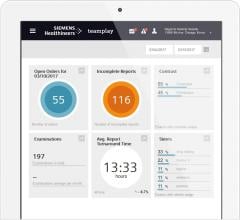
IT solutions are now increasingly being leveraged in more sophisticated ways since most hospitals have converted to integrated electronic medical records (EMRs) over the past decade. These allow all patient and departmental data to be accessible in one location. Analytics software is now being used to mine this data to identify workflow inefficiencies and areas to cut costs or improve charge capture.
Clinical decision support (CDS) software to help hospitals and doctors better meet guideline-based care in all specialties is being introduced to help clinicians make better care decisions. This includes choosing appropriate tests and procedures in an effort to reduce costs or avoid tests that will not be reimbursed.
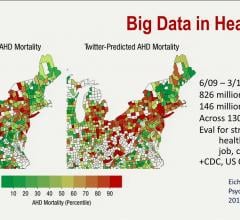
Artificial intelligence (AI) will be taking over many of the manual tasks for monitoring data and to answer questions more quickly. AI will also be used to alert administrators or doctors when it autonomously identifies a problem. Applications to watch also include AI to monitor
population health in the background. This can identify patients at risk for various cardiovascular diseases before they present with any symptoms. The software also can identify patients who need extra care and counseling because of the high likelihood they will not be compliant with discharge orders and be readmitted. AI also will offer a second set of eyes on cardiac imaging to help identify anomalies or greatly reduce time by performing all the measurements automatically without human intervention.
This use of IT also includes patient portals to engage with patients and allow better access to their records and care. This is already starting to filter down to apps on smartphones to improve care, compliance with doctors' orders and to aid diagnosis of conditions before they become problematic, such as heart failure and AF.
Cardiac Imaging Trends
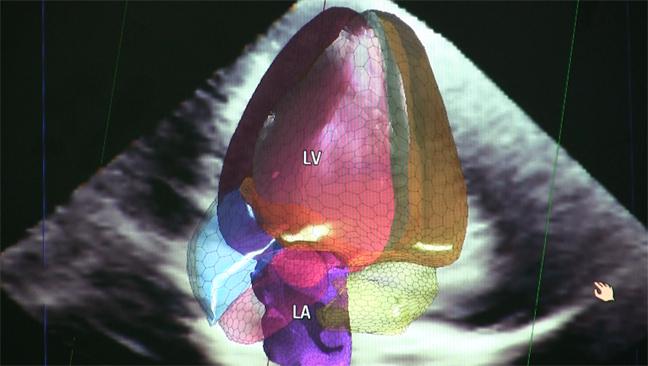
Cardiac ultrasound (echo) remains the No.1 imaging modality in cardiology because of its broad availability, low cost and no radiation. However,
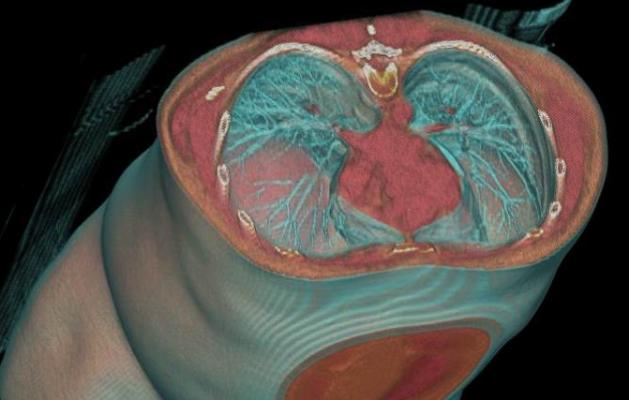
computed tomography (CT) is poised to become the front-line imaging test for acute chest pain patients in the emergency department. It is also the gold standard for structural heart procedure planning, and the number of these cases is rapidly rising.
CT fractional flow reserve (CT-FFR) technology is widely expected to become the main test for chest pain in the next decade, since it has the potential to save both time and money. CT-FFR also will become the primary gate-keeper to the cath lab to significantly lower, or possibly eliminate, the need for diagnostic catheter angiograms.
Cardiac MRI has seen numerous advances in recent years that cut imaging times by 50 percent and automate quantification, cutting the time to read and process these exams. MRI is expected to see and increase for cardiac exams in the coming years. MRI and CT-FFR may greatly reduce the number of nuclear exams, which are currently the gold standard for cardiac perfusion imaging.



 February 15, 2022
February 15, 2022