November 7, 2007 - The application of clinical practice modifications combined with advanced electronic technologies can improve the care of patients at risk for sudden cardiac arrest (SCA), according to poster data presented at Scientific Sessions 2007, the annual congress of the American Heart Association.
Recognition of at-risk patients improved from a baseline of 24 percent to 70 percent at regional clinics not using the process, and to 93 percent at the main clinic applying this process and technology.
The objectives of this prospective, single center study, sponsored by Medtronic Inc., were to compare the effect of specific clinical practice processes and tools on the ability of clinicians to recognize patients at risk for SCA, and apply the appropriate treatment guidelines for those patients.
Clinic staff was trained to use a new process to better identify at-risk patients, which included:
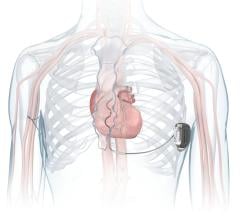
- A patent-pending clinical decision support tool for Electronic Medical Record (EMR) systems that automatically identified patients at risk and continued tracking of those patients who did not immediately qualify for implantable cardioverter-defibrillator (ICD) therapy;
- A standardized patient education process and education video;
- Broad operational and workflow changes.
The clinical practice process included optimal medical treatment prior to an implantable cardioverter-defibrillator (ICD), temporary and absolute exclusions for ICD therapy, and is based on current AHA/American College of cardiology (ACC) and the Centers for Medicare and Medicaid Services (CMS) guidelines with practice-specific requirements. An independent review of medical charts for all patients visiting the main clinic (the group utilizing the new process) and regional clinics (those that did not use the process) was conducted over a two-month period; patients were followed for six months.
“A recent report shows that it takes 10 to 15 years for new advances in medicine to be adopted into clinical practice,” said William Daniel, M.D., clinical director at Cardiovascular Consultants, P.C., and medical director of Quality and medical director of Inpatient Services at Mid America Heart Institute, Kansas City, Mo. “Recognizing this time lag, and the fact that there are thousands of pages of guidelines for caring for our cardiac patients, this study illustrated that the use of our electronic solution and process changes helped give physicians the right information at the right time, and allowed them to use their judgment and be extremely accurate in making appropriate treatment decisions. Further, every patient, regardless of age, gender or race, receives the same high quality of care, since the process reduces variability and physician reliance on memory.”
He continued, “Implementing true quality processes allows us to deliver evidence-based, guideline-driven care. Quality care should not be an option – we owe that much to our patients, ourselves and the profession of cardiology.”
Source: Medtronic
For more information: www.medtronic.com


 January 13, 2026
January 13, 2026