Feb. 1, 2007 - New data shows that a year after undergoing carotid angioplasty and stenting, a minimally invasive treatment to prevent stroke, nearly half of patients (43 percent) showed statistically significant improvement in brain function, such as memory, judgement and reasoning. Those are the findings of a study being presented at the International Symposium on Endovascular Therapy (ISET).
"Many patients have returned to a level of function they thought they had lost. That can mean being able to do things for themselves again, including driving to the store to buy milk and living at home independently," said Rodney Raabe, M.D., chief of radiology at Sacred Heart Medical Center, Spokane, WA. "As they get older, most people worry about stroke, but they also worry about becoming forgetful and losing their ability to think clearly."
In the right patient, this treatment appears to be able to improve brain functions of memory and the ability to reason, both of which are important for independent living. In the study, researchers performed a two-hour battery of 11 standard neurocognitive tests commonly used to assess patients believed to have a dementing process, such as Alzheimer's disease. Tests included functions such as having patients remember a list of words, think abstractly, repeat digits in sequential and reverse sequential order, generate lists based on cues, and complete puzzles of alternating sequences.
In the study, 16 (43 percent) of 37 patients showed significantly improved neurocognitive function one year after the carotid angioplasty and stenting procedure. Improvement was seen at three months and continued through the six and twelve month assessment points. Of the remaining patients, neurocognitive function remained stable in 20 (54 percent) and declined in one (3 percent) at one year.
"One of the biggest debates in carotid artery disease is whether to treat so-called 'asymptomatic' patients: those who have clogged carotid arteries but don't have early warnings of stroke, such as transient ischemic attacks (TIAs), or mini-strokes," said Dr. Raabe. "Our research suggests we need to rethink the term 'asymptomatic.' Even when people aren't at immediate high risk for stroke, if their carotid arteries are clogged, they have reduced blood flow to the brain and that appears to reduce brain function, which is a serious concern."
Half of the patients in the study were considered symptomatic before treatment, meaning they had suffered TIAs and had 70 percent blockage in at least one carotid artery. The remaining 15 patients were asymptomatic, meaning they had not suffered TIA, but their carotid arteries were at least 80 percent blocked.
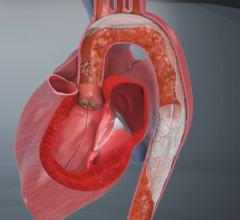
Every year, about 700,000 Americans have a stroke. About a third of those people die, making stroke the third-leading cause of death in the United States. Approximately 30 percent of all strokes are the result of clogged carotid arteries. Carotid arteries, located on each side of the neck, are the main source of blood to the brain. Like arteries in the heart and other parts of the body, the carotid arteries can become clogged with plaque, potentially causing a stroke by cutting off blood flow to part of the brain.
For many years, people with severely blocked carotid arteries had only two options to attempt to prevent stroke: medication and surgery, called endarterectomy, to open blocked arteries and clean them out. Surgery involves a neck incision of up to seven inches.
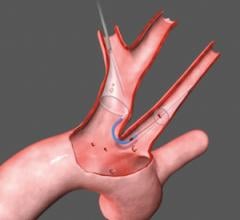
In recent years, the combination of minimally invasive carotid angioplasty and stenting is increasingly offered as an alternative to surgery. The procedure involves making a small incision in the groin and advancing a thin tube, or catheter, through the blood vessels to the site of the blockage, inflating a balloon to open up the narrowed artery and leaving behind a stent, a tiny metal mesh device that acts as scaffolding to keep the artery propped open.
Studies show that both surgery and angioplasty with stenting can reduce the risk of stroke in asymptomatic patients by half.
Early on, carotid angioplasty with stenting was considered risky because in placing the stent, blood clots were often knocked loose and could travel to the brain, potentially causing a stroke. Filter-like devices were developed to catch the clots and prevent them from going to the brain, but tiny clots can still escape and have been thought to contribute to cognitive decline following treatment.
Dr. Raabe's study originally set out to determine if the filter devices helped patients maintain cognitive function. The research team was pleased to find that not only did brain function not get worse, it improved. The study suggests that by opening up the artery, angioplasty and stenting increases blood flow. Increased blood flow allows the brain more effective access to neurocognitive reserves, outweighing negative effects of tiny clots that pass through the filter. Several studies have looked at brain function after surgery, with mixed results. While studies have shown that blood flow to the brain improves after surgery, the invasiveness of surgery, coupled with the required general anesthesia, may lead to decreases in neurological function. "It's sort of a wash," said Dr. Raabe.
Considered to be the premier meeting on endovascular therapy, the International Symposium on Endovascular Therapy (ISET) is attended by more than 1,200 physicians, scientists and industry professionals from around the world. The meeting pioneered the use of live cases to promote the multidisciplinary treatment of vascular disease. ISET is presented by the Baptist Cardiac & Vascular Institute, Miami.


 April 25, 2023
April 25, 2023