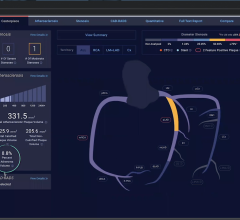
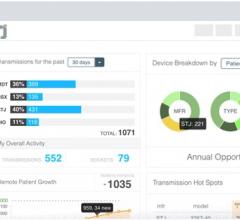
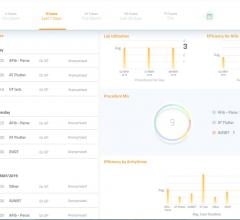
An example of flexible electronics made by MC10. These types of wearable devices may soon be used to remotely monitor patients.
Several futuristic technologies and their potential impact on healthcare were discussed during the Future of Cardiovascular Medicine track sessions at the American College of Cardiology (ACC) 2015 annual meeting. Among the topics were use of big data, the integration of smartphones and wearable devices into patient care, robots in the cath lab, 3-D printing and how technology will help lower the cost of clinical trials for drugs and devices and speed their introduction to market.
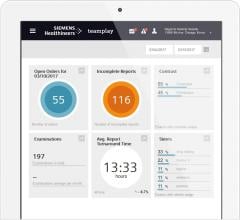
Smartphone Apps, Wearables to Montor Cardiac Conditions
There has been an explosion of healthcare-related apps for smartphones, which number more than 250,000, said Peter Fitzgerald, M.D., Ph.D., director of the Center for Cardiovascular Technology and Innovation, and director of the Core Cardiovascular Analysis Laboratory, Stanford University, California. Consumer-grade wearable devices now interface with these apps to record exercise data, heart rate, blood pressure, ECG and other vitals. Fitzgerald said wearables now account for a quarter of sales growth in personal health monitoring devices. While on the surface this looks like a consumer trend, he said these apps and devices will have a major impact on the future of healthcare.
“There are more cell phones in the world than there are toothbrushes,” he explained. “We are living in a planet of cell phones.”
He said the number of smartphones and the rapid expansion of wearable sensors could be leveraged to bring personalized healthcare to billions of people. This might have a major impact on management of heart failure (HF), where apps can remotely monitor hundreds of thousands of patients for signs that their symptoms are worsening, and can notify patients to increase medications or contact their doctor. Fitzgerald explained this type of big data technology already exists to detect and flag credit card fraud long before a customer realizes their card or personal information was stolen.
“It is like a credit card fraud problem, where software can monitor heart failure remotely,” Fitzgerald said. This would help reduce the current number of HF readmissions for patients with imporperly managed chronic HF. “Hospitals should be for emergencies, not urgencies,” he explained.
Use of Health Kiosks in Hospitals, Clinics and Pharmacies
While apps and personal monitoring devices offer new mechanisms to provide real-time lifestyle management, another innovation to aid patients in a timely manner is the use of healthcare kiosks. These are already coming into use at university health centers for after-hours care, and will soon be available at major pharmacy chains such as the Walgreens and Walmarts of the world. These not only measure blood pressure and take basic vitals, but also can perform simple blood tests, allow two-way video telemedicine conferencing with a healthcare provider and dispense prescriptions.
The 'Uberization' of Healthcare
In the information technology world, a recent innovation has been the software as a service (SaaS) model, where software access can be leased and operated and updated over the Internet, eliminating the need to load the software and regular updates on a hospital’s own computer network or each computer. Fitzgerald said this will be used as a business template for greater electronic access to healthcare. Integrating use of smartphones, patients will soon be able to access physicians, or locate the closest healthcare kiosk, clinic or hospital using mobile apps. He said this will lead to an “Uberization” of healthcare, similar to customers who use the Uber app to quickly locate and electronically hail the closest available cabs.
“Today’s consumers are much less patient because they expect instantaneous responses, and this will drive healthcare with 30-somethings and younger,” Fitzgerald said.
He acknowledged a lot of older healthcare providers may have an issue with the generational gap in smartphone technology and the expectation for immediate responses on things like appointments, imaging and test results. However, Fitzgerald said providers need to adapt to stay competitive in today’s market where consumerism and competition for these patients is now driving healthcare. These new technologies also offer pathways for much improved efficiency, which many providers might overlook.
David Holmes, M.D., Mayo Clinic, Rochester, Minnesota, and former ACC president, asked Fitzgerald what older cardiologists such as himself who might be unfamiliar with mobile technology can do to catch up to this technology boom and move away from how they have always done business.
“Currently you swallow the inefficiencies — you just accept it, but with these new technologies there is a vast improvement in efficiency, you just need a 16-year-old to show you how to use it,” Fitzgerald explained.
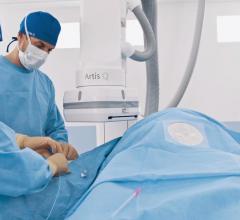
Robotics in the Cath Lab and EP Lab
Robotic systems are now U.S. Food and Drug Administration (FDA)-cleared for use for interventional cardiology procedures (Corindus Corpath) and for catheter ablations in the electrophysiology lab (Hanson), which enables more precise, controlled catheter manipulation than is possible with manual manipulation. However, one of the overarching benefits of these systems is that it removes the operator from the radiation field and allows them to work sitting down behind a console, without the need to wear lead aprons, Fitzgerald said. He noted the high statistics of interventional cardiologists who have orthopedic issues from wearing lead for their entire career, and the high rates of left side brain cancers and glaucoma due to radiation exposure. He said robotics can help eliminate these issues and make the cath lab a more comfortable and safer place for physicians to work.
“You can still do your best work in cases, but without the radiation dose,” Fitzgerald said.
Nanobots to Non-invasively Treat Diseases
Biocompatible machines on or near nano-scale are being developed that might have application for targeted medical therapies in the future, said Anthony DeMaria, M.D., the Judith and Jack White Chair in cardiology and founding director of the Sulpizio Cardiovascular Center at the University of San Diego School of Medicine. A basic example of this is the development of devices that can use nano-bubbles to propel a nanobot through stroke or pulmonary embolism thrombus to create channels that allow faster penetration of tPA to dissolve the clot.
Flexible Sensor Technology to Monitor Patients
The current explosion of consumer health sensor devices that interface their smartphone is just the beginning of a new era of miniaturized sensor technology, DeMaria said. He explained the next generation of sensor integration will be flexible, microcircuitry devices that can be printed from thin, pliable film for direct contact adhesion on the patient’s skin. These devices, applied like a temporary tattoo or stickers, will be able to directly monitor patient vitals more accurately than most current, larger wearable devices.
Cell Therapies to Treat Cardiac Conditions
DeMaria said new cell therapies in development include the concept of “disease in a dish,” where a patient’s own cells can be cultured and made resistant to a particular disease. These cells can then be reintroduced into the patient to make their whole body resistant.
He said another exciting concept is research looking at the use of virus vectors to create targeted pacemaker therapies.
3-D Printed Replacement Heart Valves and Blood Vessels
The use of 3-D printed anatomy from computed tomography (CT) datasets is already being used as a teaching aid at medical schools, and to help plan complex cardiovascular surgical procedures. DeMaria said research is being conducted to replace the polymers currently used to build up the 3-D printed structures with live cells or biocompatible polymers to create replacement organs, heart valves and vessels. The 3-D technology would allow creation of exact fit replacement parts customized for each patient.
Read the article, "The Future of 3-D Printing in Medicine."
Personalized Medicine in Cardiology
The cost of genetic testing has fallen dramatically over the past decade to a point where it is feasible to screen patients for their predisposition for specific diseases for about $1,000 or less. DeMaria said this type of screening would go a long way to identifying at-risk patients years before they show any signs of disease. It might also aid in the development of personalized pharmacogenomic agents and improved patient monitoring and prevention efforts for many types of diseases, detecting them before an onset of acute care episodes.
Genetic testing will be one part of the future of cardiology where emphasis will shift to preventive, personalized treatment where the patient is included and actively participates in their care. “Patient participation will be encouraged and increased because of poor participation now,” DeMaria said. “Around 50 percent of patients do not adhere to medication compliance for cardiovascular drugs they are prescribed.”
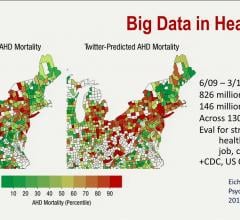
Use of Big Data to Offer New Insights in Cardiology
Healthcare has been very focused on using data for administrative purposes and has not been proactive in using it to engage patients or improve patient outcomes, said James Tcheng, M.D., FACC, FSCAI, professor of medicine, Duke University School of Medicine, North Carolina.
“We are falling short of achieving meaningful use of health information technology,” he said. “We are focused on administrative click-off boxes. But, data is now being used to help identify which patients we need to engage, and this is a paradigm shift. I think big data will be a big driver in the future for research and how we provide care.”
With the conversion to electronic medical records (EMR), he said a typical tertiary care hospital generates about 100 terabytes (TB) of data per year. By comparison, he said the Library of Congress is estimated to contain only about 10 TB of text data.
This volume of data offers new sources of healthcare insights that previously were very difficult and time-consuming to tabulate. Take for example the ability to find heart failure (HF) population trends based on region, state, county or individual hospital. These factors might include pulling unrelated vital signs trends from yearly exams or family history in EMRs to predict which patients should be screened for HF years before they present with HF symptoms. Analytics showing low income areas with a high incidence rate of HF acute care episodes in emergency departments might help target preventive outreach programs or help earmark federal funds. Combing through large amounts of data on a population of patients might also help identify new ways to curb readmission rates or better engage patients so they can manage their condition.
Read the article, "Understanding How Big Data Will Change Healthcare."
Digital Clinical Trials in Cardiology Using Computer Modeling
Computer modeling is a well-established research method in industries outside of healthcare but it will see growing application in medicine, said Paul David Morris, MBChB, MRCP, BMedSci, University of Sheffield, Sheffield, United Kingdom. Computing power today is sophisticated enough to create virtual humans that might be used in the future to perform virtual clinical trials.
He said the technology has already gained acceptance with the FDA with the approval last November of HeartFlow’s virtual computed tomography-fractional flow reserve (CT-FFR) software. It uses supercomputing fluid dynamics software to reconstruct a 3-D simulation of a patient’s heart from CT scans. It assesses the FFR blood flow for all coronary vessel segments and has very close correlation to invasive catheter-based FFR measurements in the cath lab. Another company is Austria-based Vascops, which developed similar software called A4clinics for detailed fluid dynamic analysis for aortic aneurysms, Morris said.
He explained this technology can be translated into virtual clinical trials for new implantable cardiovascular devices. Morris predicts the use of “in-silico” trials in the next few years to help cut clinical trial costs and speed testing to bring devices to market faster.
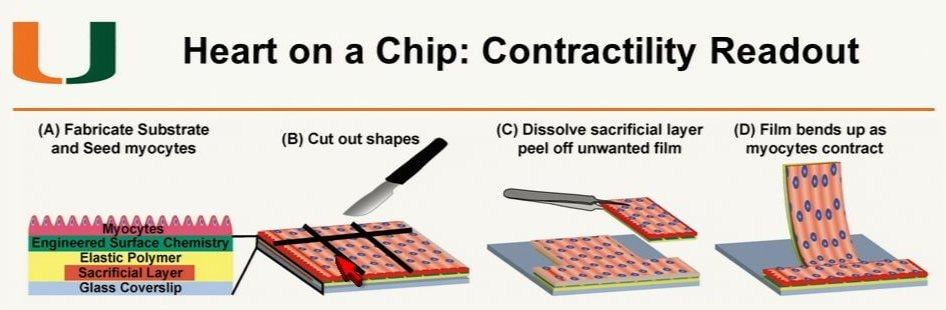
Heart on a Chip Technology May Greatly Speed Preclinical Research
Ashutosh Agarwal, Ph.D. assistant professor, Department of Biomedical Engineering, University of Miami, Florida, has been working on developing human organ mimic platforms. Often called “organs on a chip,” he explained a nano-printed silica microchip-like device can be configured in different formats to act as a scaffold for different types of human organ cell cultures. In the case of the heart, strips can be created on the chip to create a scaffold so a culture of human myocytes can grow along them to create a similar cellular alignment as found in the myocardium. This “heart on a chip” created on a thin film, can be cut into strips that will flex as the myocytes contract. Various drug candidates can be used on these chips and the contractibility tested to verify if an agent has any influence on human heart tissue. These systems offer data within minutes or days, instead of weeks or months.
Related Future Technologies in Cardiology and Healthcare Content:
The Future of 3-D Printing in Medicine
VIDEO: Editor's Choice of Future Healthcare Technologies at HIMSS 2015



 May 07, 2026
May 07, 2026