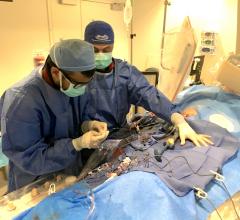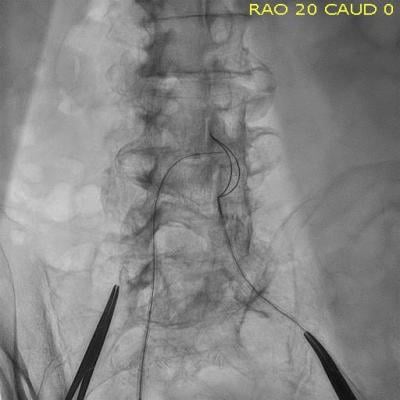
A transcaval access TAVR procedure, showing a guide wire in the vena cava and a snare located in the aorta to pull the guide wire through.
Patient selection for who is best suited for a transcatheter aortic valve replacement (TAVR) procedure is partly based on vascular access routes that can accommodate the large diameter TAVR devices. The femoral access route is considered the best option because it is the most minimally invasive, but some patients will not qualify because of heavy calcification or large lesions in the femoral artery, or popcorn-type calcifications in the aorta. A new, innovative approach to bypass the issues in suboptimal access vessels uses the transcaval access method. This involves using femoral vein access and then a small puncture is made into the aorta above the problematic regions to continue on to the heart.
One of the key pioneers of this technique is Adam Greenbaum, M.D., co-director of the Henry Ford Center for Structural Heart Disease, Detroit. His hospital has now conducted more than 100 transcaval procedures, making Henry Ford the center with the most extensive experience with the technique to date.
Worldwide, he said there have been more than 350 transcaval TAVR cases performed at about 40 centers.
"It continues to grow. There is interest expressed by other sites on a daily basis because there is this whole push in transcatheter valve technology for less invasive ways to do these procedures. If you don't have femoral access, we are asking what is the least invasive way of still delivering the transcatheter valve," Greenbaum said. "There is this push away from transapical access to extra-thoracic access to stay out of the chest, and these options include subclavian, carotid or transcaval. Interestingly, with transcaval we are routinely sending patients home on day one after their procedure."
What is Trancaval Access?
"Transcaval access starts with access in the venous system, traveling up to the inferior vena cava (IVC) up to a point at the aorta where it is large enough to handle the delivery sheath for the transcatheter valve," Greenbaum said. "You cross over in the retroperitoneal space between the vena cava and the aorta. You then continue on up the aorta for a standard retrograde TAVR."
He said the concept originated around 2010 at the National Institutes of Health (NIH) as a proposed method to solve delivery issues using larger devices. After testing the concept and refining techniques in animal testing, the first-in-human procedures occurred in 2013.
Safety of Transcaval Procedures
When the first cases were presented there was surprise from some interventional cardiologists who questioned the safety of puncturing the aorta in the center of the patient's abdomen. "The procedure seems to work pretty well, but it is amazing how polarizing that concept still is years later, because people think if you put a hole in the side of the aorta, that is going to be a very quick demise for that patient," Greenbaum said. "But in actuality, with a simultaneous hole in the IVC, because the pressure in the retroperitoneal space is higher than the IVC, the blood actually moves from the hole in the aorta to the hole in the IVC and stays intravascular. That is the concept that makes this procedure take place."
No conduit is used to bridge the two openings, "there is just empty space there," Greenbaum explained. He said the delivery sheath for the TAVR system helps form a hemostatic seal between the openings in the IVC and the aorta.
After the TAVR procedure when the sheath is removed, a steerable introducer sheath is used to guide the placement of an Amplatzer duct occluder to seal the wall of the aorta. "Interestingly, we don't close the hole on the venous side. All of these fistula tracks close over time, from hours, to days or weeks," he said.
"People think that this would be a high-anxiety-provoking part of the procedure, but it really isn't. Their blood pressure stays fine and it can be done in a very controlled situation," Greenbaum confirmed.
How to Gain Transcaval Access
Greenbaum described the steps for the transcaval procedure as follows:
1. Computed tomography (CT) is used to plan the procedure to find where there is a good location cross between the vessels. Greenbaum chooses a location below the level of the renal arteries where there is no calcium. "We use a contrast CT of the aorta before the procedure to assess suitability and choose the level at which to cross into the infrarenal aorta. We make sure no structures like bowel loop or major side branches are at the level of crossing by examining the CT before the case. Typically, the access is at the level of the L3-L4 disc space, which we use for geographic landmarks," he explained.
2. Angiography alone is used to guide access and closure. A standard goose neck single loop snare is positioned in the aorta to identify a landmark landing zone on fluoro imaging and help a guide wire from the IVC across into the aorta.
3. Standard 6 French diagnostic guiding catheters are then used (usually renal-shaped work best) in the IVC to point an 0.014-inch coronary guide wire toward the snare in the aorta.
4. A transcatheter electrosurgery ablation system is used to create the hole in the walls of the vessels. Greenbaum said the electrode is energized only for about a second to cross between the vessels.
5. Escalating wire sizes are then used across the opening from the IVC to gradually enlarge the opening. Greenbaum starts with an 0.014 wire, then moves to an 0.035 stiff wire that will enable the delivery of the TAVR sheath.
6. Vessel closure is performed using a deflectable catheter, usually an Abbott Agilis catheter, to help orient an Amplatzer ductal occluder to plug against the wall of the aorta. Greenbaum said only the aortic hole is sealed, so a double-sided occluder is not needed. He said a single-sided, first generation duct occluder is used. Henry Ford has standardized on only using the 10 mm size Amplatzer, which matches the size of the hole left by the TAVR sheath.
7. Monitoring of these patients after discharge includes a followup CT scan at 30 days just to confirm everything is normal at the access sites. Greenbaum said Henry Ford early on used serial CT scans to monitor these patients, but found the 30-day scan was sufficient.
Transcaval TAVR Patient Selection
TAVR patients are generally older and usually have significant peripheral artery disease (PAD), which can often exclude the use of the femoral access route. This is why CT scans are performed prior to TAVR procedures to determine the best access routes to deliver the transcatheter device to the aortic valve
"There is no doubt that these are sicker people to start," Greenbaum explained. "People with peripheral vascular disease have calcified aortas, they have calcified subclavians, they have disease in their carotids. Obviously, knowing how to do all of these alternative access methods, I think, is helpful for a referral center so they can actually help a patient benefit from a transcatheter heart valve by being able to give it to them."
For these patients, Greenbaum said transcaval is the least invasive way to get them through the procedure, which may translate to better outcomes. "We do see the 30-day outcomes in these patients are equally as good to any of the other access methods," he said.
Related Transcaval TAVR Content:
VIDEO: Transcaval Access in TAVR Procedures — Interview with Adam Greenbaum, M.D.
VIDEO: Walk Through of the Henry Ford Hospital Structural Heart Cath Lab
Study Deems Transcaval Valve Replacement Pioneered at Henry Ford Hospital Successful
First Transcaval Aortic Valve Replacement Performed in Europe
Additional articles and videos on Henry Ford Hospital
Find more structural heart technology content
References:





 April 27, 2023
April 27, 2023