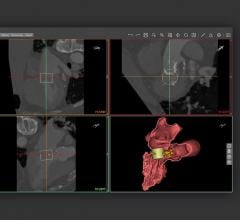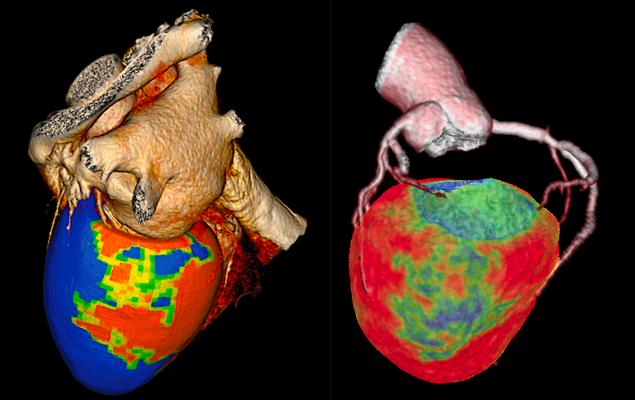
Two examples of CT myocardial perfusion (CTP) imaging assessment software. Canon is on the left and GE Healthcare is on the right. Both of these technologies have been around for a few years, but there has been an increasing amount of clinical data from studies showing the accuracy of the technology compared to nuclear imaging, the current standard of care for myocardial perfusion imaging, and cardiac MRI.
Here is an overview of a few of the biggest technology advances in cardiovascular computed tomography (CT). These are helping push CT angiography (CTA) to become a primary imaging modality with the ability to push beyond anatomical imaging to allow physiological imaging similar to the information offered by nuclear imaging and MRI.
Other advances include the ability to greatly lower dose and improve image quality using artificial intelligence (AI) image reconstruction and being able to show photo-realistic anatomical imaging that is helpful in explaining conditions to patients or surgeons.
CT Myocardial Perfusion Imaging
In March 2020, the Society of Cardiovascular Computed Tomography (SCCT) released a new expert consensus document on CT myocardial perfusion (CTP) imaging. The recommendations outline the use of both coronary anatomy and myocardial perfusion to help identify those patients who might most benefit from further invasive procedures to treat their coronary artery disease.
“CT perfusion has been developed and significantly validated over the last decade; however, its adoption into clinical practice has been limited by the lack of standardization and other factors. This international expert consensus group was comprised of a diverse group of individuals with significant experience in CT perfusion imaging and were tasked to identify some of the key principles that unify the various approaches to CTP,” said writing group co-chair Amit Patel, M.D., FSCCT of University of Chicago.
CT perfusion has been available for several years, but clinical study evidence was needed to show correlation between the analysis software, real-world disease and the gold-standard technologies of MRI and nuclear perfusion imaging. SCCT said the growing body of evidence has established the diagnostic accuracy and incremental value of myocardial CTP over coronary CTA.
In single center studies, myocardial CTP imaging has demonstrated high accuracy when compared with single photon emission computed tomography (SPECT), cardiovascular magnetic resonance (CMR), invasive coronary angiography (ICA), positron emission tomography (PET) and invasive fractional flow reserve (FFR). Multicenter studies have also established the accuracy of combining myocardial CTP with coronary CTA. These studies suggest that CTP is particularly accurate when interpreted in the context of coronary CTA findings.
The new consensus statement provides expert consensus regarding the performance and interpretation of CTP, including patient selection, image acquisition, post-processing and interpretation of CTP results.
“The combination of coronary CTA and CTP can be used to detect both coronary atherosclerosis as well as its physiological consequences. While further studies will continue to refine the capabilities of CTP, the current expert consensus statement will be useful for clinicians and researchers who are interested in adopting this technique,” says writing group co-chair Ron Blankstein, M.D., MSCCT, of Brigham and Women's Hospital and SCCT president.
Noninvasive CT-based FFR and Planning Interventional Procedures
A key diagnostic tool to determine if a stent is needed in a coronary lesion in the cath lab is pressure wire based FFR. However, the technology requires the use of pharmacological stress agent adenosine and a wire pull back in the vessel, taking additional procedure time and adding cost to the procedure limiting adoption. Expanded use of FFR would likely take place if the technology was less expensive and easier to use. CT-based FFR (FFR-CT) is now being use by many larger hospitals to assess patients presenting with chest pain faster than traditional troponin testing, keeping patients overnight for morning nuclear scans or sending them to the Cath lab for invasive angiograms. FFR-CT is also starting to be used at some centers to help plan procedures.
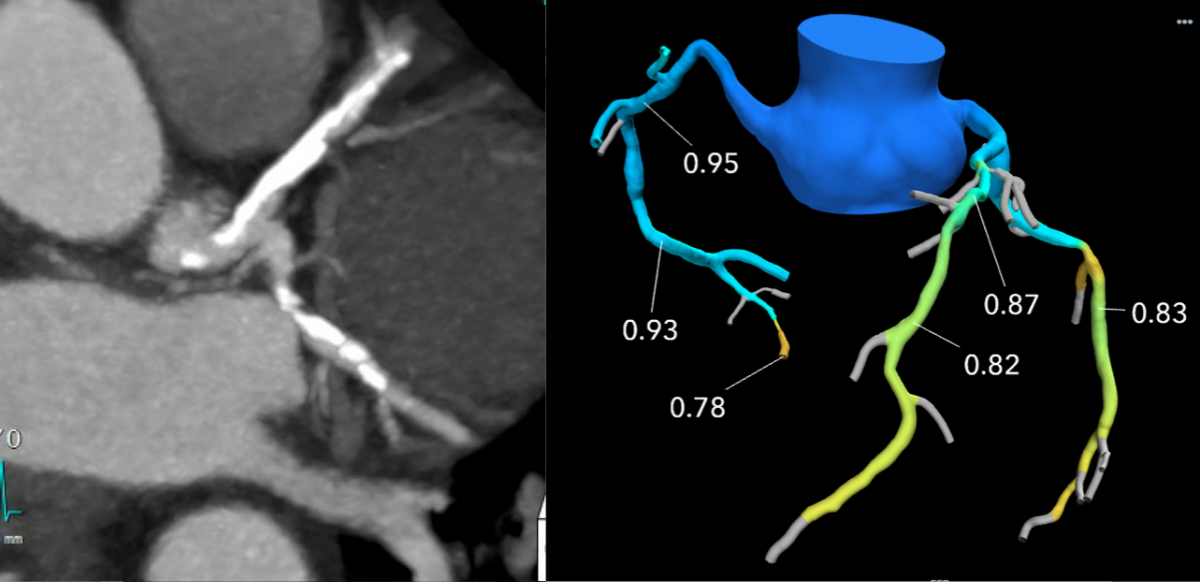
A HeartFlow FFR-CT example showing comparison with a CT scan of heavily calcified coronary arteries. The lesion looks severe anatomically on CT, but it not significant enough to qualify for stenting according to the FFR-CT.
The CT imaging is sent to an outside vendor so it can be run through a computational fluid dynamics algorithm using a supercomputer to create a 3-D coronary tree with FFR ratios for all the vessel segments. It can take up to a couple hours to process the results, but it is fast enough to clear most patients to go home if there are no clear blockages anatomically or physiologically.
“CT has advanced amazingly over the past 20 years,” James Udelson, M.D., chief of the division of cardiology, Tufts Medical Center. “There is a 99 percent predictive value that if you see severe disease that you will find severe disease in the cath lab. The problem has been with moderate lesions, such as a 60 percent stenosis in the mid-LAD — is that physiologically significant? Patients who get CT are often cathed at a high rate, likely because a physician sees the moderate stenosis and are worried about it and they do a cath. Now, with FFR-CT, you can interrogate using just a resting CT dataset to see if that 60 percent stenosis is or is not physiologically significant.”
Using this technology, Tufts has been able to reduce the number of diagnostic catheterizations for moderate stenosis patients, now only sending patients to the cath lab who are confirmed through the CT-FFR that they need revascularization.
Predicting Outcomes of Stent Procedures Using FFR-CT Modeling
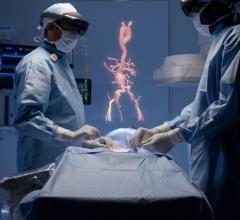
The most recent iteration of the Heartflow FFR-CT technology that gained U.S. Food and Drug Administration (FDA) approval in September 2019 allows the user to virtually stent a vessel segment to determine the FFR value if the vessel was opened to its native lumen size. This serves as a planning tool to assess patients prior to entering the cath lab and predicting what their coronary flow might be under optimal revascularization conditions.
HeartFlow Planner is a non-invasive, real-time virtual modeling tool for coronary artery disease (CAD) intervention. It enables interventional cardiologists to virtually model clinical scenarios vessel-by-vessel, explore treatment strategies before a procedure.
“The information provided by the HeartFlow technology is powerful and will not only help us efficiently diagnose coronary artery disease, but help us better understand different treatment options,” said Victor Marinescu, M.D., cardiologist, Advocate Health Midwest Heart Specialists and member of the medical staff, Edward-Elmhurst Health. “The visual nature of the HeartFlow Planner also makes it a great tool to explain to patients what will happen during their procedure.”
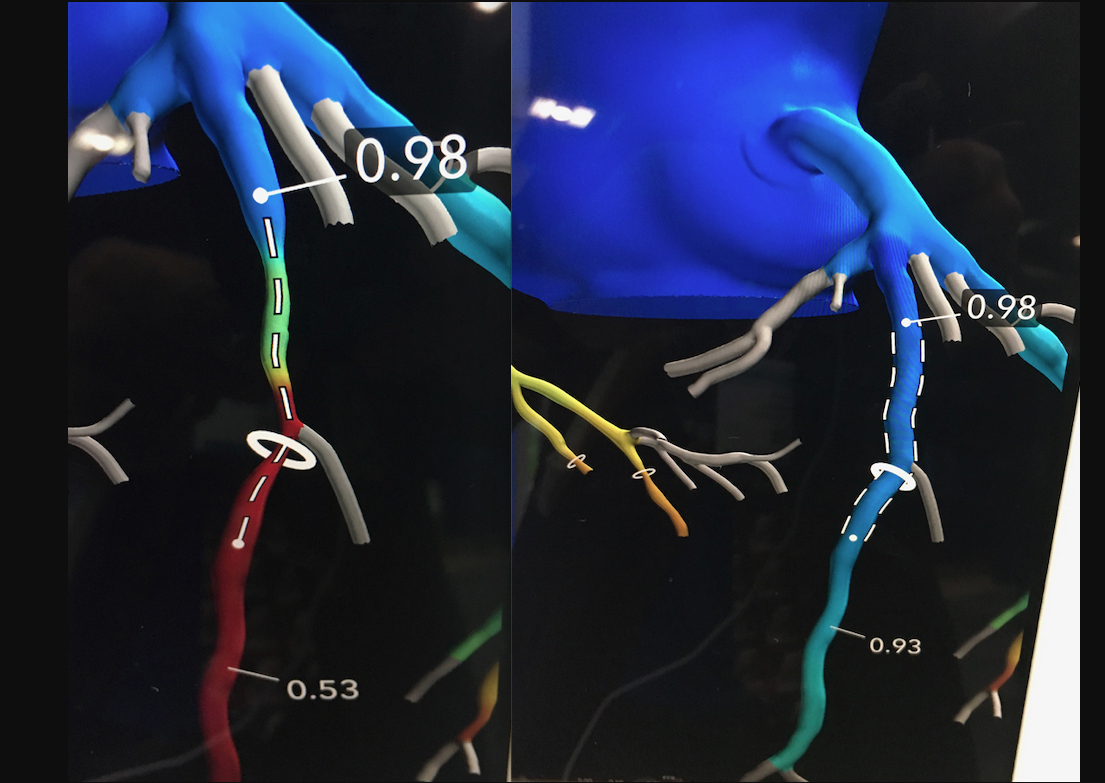
HeartFlow Planner is a non-invasive, real-time virtual modeling tool for coronary artery disease (CAD) intervention. The HeartFlow Planner will enable interventional cardiologists to virtually model clinical scenarios vessel-by-vessel, explore treatment strategies for patients with CAD before each procedure, review cases with colleagues and ensure everyone has a clear picture of the initial treatment plan.
Artificial Intelligence Enters CT Image Reconstructions
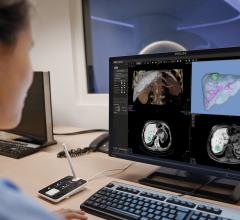
CT vendors are developing new AI algorithms to reconstruct CT images better than conventional iterative or model-based reconstruction methods. Both Canon Medical Systems and GE Healthcare now have deep-learning CT image reconstruction software, both of which gained FDA clearance in the spring of 2019.
In deep learning, you feed the system the answers (in the case of CT, what ideal clinical images and resolution should look like) and the machine figures out what needs to be done with input image data to make it look like the ideal reference image, explained Jeannie Yu, M.D., FACC, FSCCT, director of cardiovascular imaging, Long Beach VA Health System. In this way, she said deep learning can be used to help in image resolution recovery that has better noise reduction and resolution than iterative reconstruction images.
Her center is using Canon Medical Systems’ AiCE deep learning reconstruction (DLR) software for the Precision CT system. The technology uses 10 convolutional neuro network (CNN) algorithms with different kernel sizes to reconstruct the images. Yu illustrated that this AI-driven software takes a lot of computing power, with the system operating using 71.2 teraflops. A teraflop is a unit of computing speed equal to one million floating-point operations per second. For comparison, Yu said IBM Watson AI software operates at 80 teraflops, a Playstation 4 game console at 1.8, Xbox One X gaming console at 6 and the iPhone X runs at 5 teraflops.
GE Healthcare developed its Deep Learning Image Reconstruction (DLIR) software for the Revolution Apex CT system. This next-generation image reconstruction option uses a dedicated deep neural network (DNN) to generate what GE calls TrueFidelity CT Images. Compared to current iterative reconstruction technology, TrueFidelity CT images can elevate every image to offer better image quality, image sharpness and noise texture, according to GE.
Photo-realistic and Surgical View Imaging
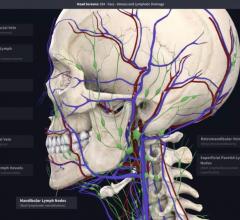
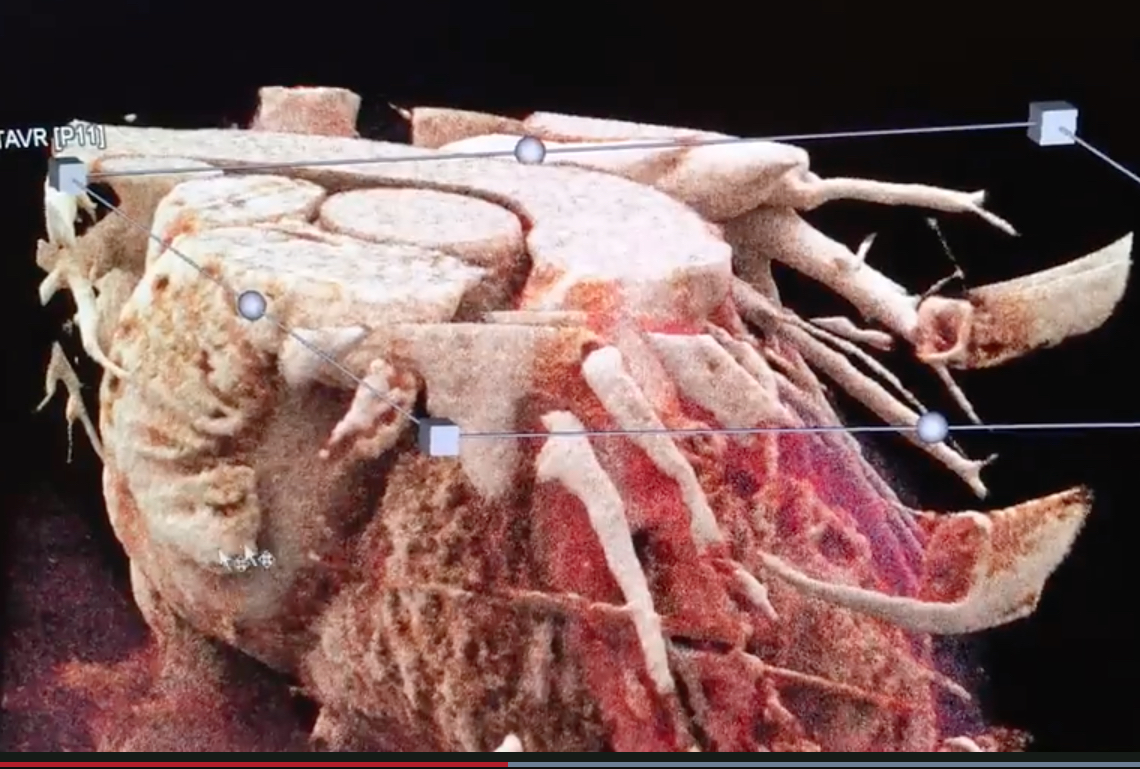 A few CT vendors now offer advanced visualization software offering realistic, photo-quality, surgical view image renderings. Canon Medical offers its Global Illumination photo-realistic rendering and Siemens Healthineers offers its cinematic image reconstruction. Vendors who offer this technology say it is not used for diagnostics, but can be helpful when explaining things to the patient and their family, educating physicians and staff, and for surgeons. It offers a realistic view of the anatomy that is easier for most people to understand who are not familiar with cardiac anatomy as it appears in traditional CT multiplanar reconstruction (MPR) images.
A few CT vendors now offer advanced visualization software offering realistic, photo-quality, surgical view image renderings. Canon Medical offers its Global Illumination photo-realistic rendering and Siemens Healthineers offers its cinematic image reconstruction. Vendors who offer this technology say it is not used for diagnostics, but can be helpful when explaining things to the patient and their family, educating physicians and staff, and for surgeons. It offers a realistic view of the anatomy that is easier for most people to understand who are not familiar with cardiac anatomy as it appears in traditional CT multiplanar reconstruction (MPR) images.
Here are two examples of the technology:
ESC Guidelines Give Coronary CTA a Class 1 Recommendation
In September 2019, the European Society of Cardiology (ESC) published new guidelines on the diagnosis and management of chronic coronary syndromes (CCS), which classifies (CTA) as a Class 1 recommendation for diagnosing CAD in symptomatic patients. The document, which is a continuation of the 2013 stable coronary artery disease (CAD) guidelines, updates the term to CCS to emphasize the dynamic nature of the disease.
Per the guideline, unless obstructive CAD can be excluded based on clinical evaluation alone, either non-invasive functional imaging or anatomical imaging using coronary CTA should be used as the initial test to rule out or establish the diagnosis of CCS.
The new guideline suggests that "Coronary CTA is the preferred test in patients with a lower range of clinical likelihood of CAD, no previous diagnosis of CAD and characteristics associated with a high likelihood of good image quality."
“Depending on patient characteristics, local expertise and availability, as well as patient-specific considerations, physicians should decide between coronary CTA and ischemia testing,” said ESC President-elect Stephan Achenbach, M.D., FSCCT. “This is a recognition of the numerous trials that have been performed to establish the usefulness and reliability of CT angiography as a first-line examination."
“The guideline recommendations are based on data that shows that the use of coronary CTA leads to accurate identification of coronary artery disease, which if treated appropriately, can lead to improved patient outcomes.” added Blankstein. “The guidelines recognize that there are multiple factors that should be used in test selection, but that for many, a coronary CTA-first approach is beneficial.”
Related Cardiac CT Technology Advances Content:
7 Hot Topics in Cardiac CT Imaging
Image Gallery From the Society of Cardiovascular Computed Tomography 2019 Meeting
VIDEO: Use of FFR-CT to Non-invasively Evaluate Coronary Lesion Severity — Interview with James Udelson, M.D.
SCCT Issues Expert Consensus on CT Myocardial Perfusion Imaging
8 Cardiovascular Technologies to Watch in 2020
New ESC Guideline Provides Class 1 Recommendation for Coronary CTA
HeartFlow Announces FDA Clearance for HeartFlow Planner
VIDEO: Example of an Automated CT Cardiac Calcium Scoring Exam
VIDEO: Example of In-Stent restenosis Visualized Using Spectral CT
VIDEO: Will CT-FFR Replace Diagnostic Angiograms? — Interview with Patrick Serruys, M.D.
VIDEO: Walk Around of a Siemens Go.Top Dedicated Cardiac Scanner
VIDEO: Walk Around of a GE Cardiographe Dedicated Cardiac CT Scanner
VIDEO: Using FFR-CT in Everyday Practice — Interview with Kavitha Chinnaiyan, M.D.

 May 12, 2020
May 12, 2020