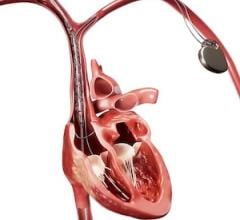
Cardiac computed tomography (CT), magnetic resonance imaging (MRI), echocardiography and nuclear myocardial perfusion imaging each offer advantages and disadvantages, and frequently at least two of these tests are required to get the full picture of a patient’s cardiac health. However, in this age of cutting healthcare costs, declining reimbursements and improving efficiency, it would be advantageous to have a single gold standard exam. Technology advances are now making that possibility.
MRI is ideal because it uses zero radiation, offers higher contrast and clarity than CT, can image without contrast and performs perfusion exams. But, its limitation remains its expense, ferrous metal and implantable device safety issues and the complexity of its operation.
Nuclear imaging is limited because it fails to provide detailed anatomical information and uses ionizing radiation. It also is expensive, and short half-life radiotracers limit its hours of operations and on-demand use.
Software advances have improved 3-D echo image quality to the point where it appears like a CT reconstruction. It uses no radiation and offers immediate images of anatomy inside the body. But, echo has a limited ability to image the function of the heart. It also requires highly trained operators to ensure precise positioning of the transducer and interpretation can be subjective. (To read about recent echo advances from the September-October 2012 issue, go to www.dicardiology.com/article/ultrasound-sees-increasing-use-interventional-procedures)
CT has the major disadvantage of high radiation doses compared to other modalities, but technical advances make CT the most likely dominant cardiac imaging technology in the next decade. The rapid expansion and decreasing cost of computing power has enabled fast iterative reconstruction software for lower dose scans. New detector technology is reducing the amount of electronic noise in lower-dose scans and new ECG gating technology has helped cut dose. Combined, these advances have reduced CT dose by more than 50 percent compared to doses a few years ago.
CT analysis software now allows visualization and quantification of perfusion in the myocardium with images similar to nuclear studies, but with a highly accurate anatomic image base.
Taking perfusion imaging a step further, CT software now cleared in Europe and in trials in the United States can quantify the fractional flow reserve (FFR) for all vessel segments in the coronary tree, allowing cardiologists to pinpoint the exact lesion causing ischemia. In the future, this technology may eliminate the need for diagnostic catheter angiography and provide a detailed navigation and treatment plan for interventional cardiologists to cut procedure time and improve patient outcomes. (To read more about these CT advances in the September-Octover 2012 issue, go to www.dicardiology.com/article/latest-advances-coronary-ct-angiography-software.)
Lastly, CT is already a primary tool in emergency rooms and radiology departments across the country. Its widespread availability, ease of use and elimination of user-dependent variability makes CT a primary candidate.



 May 12, 2026
May 12, 2026