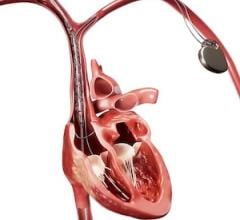
The percentage of women entering the cardiology workforce is low, despite the fact that half of all medical students are women. Despite the low numbers, many women have become luminaries in the field of cardiology, including Dee Dee Wang, M.D., director of advanced cardiovascular imaging at Henry Ford Hospital, pictured here.
Now, more than ever, the field of cardiology needs women.
But as the national need for more cardiologists overall increases, fewer medical students are choosing to pursue a career in cardiology. Shockingly, the percentage of women entering the cardiology workforce has remained low for well over 10 years. While half of all medical students are women, fewer than one in five cardiologists is female.
I wish I better understood the reasons why. I fell in love with cardiology on the first day of medical school, almost literally. I thought the heart was an amazing organ, and because it was so intuitive, I could easily determine what would happen if certain parts stopped working or what it meant if an image showed an abnormality. I can whole-heartedly say there has not been a single day when I’ve regretted making that decision, but many women hesitate to do so.
Some believe they cannot have an adequate work-life balance if they choose such a “demanding” field, but I have found that women truly can have it all, just perhaps not at the same time.
A series of papers in the May 30, 2018 issue of JAMA Cardiology discussed a range of potential reasons for underrepresentation of women in cardiology. In a survey of internal medicine trainees in 198 residency programs, female respondents and all respondents who chose not to go into cardiology placed a greater value on factors related to work-life balance than on finding stimulating work.
They have been conditioned to believe that the field of cardiology in particular has extensive irregular hours and significant on-call demands in interventional cardiology and other cardiovascular fields. Many also believe that there are very limited opportunities for female cardiologists — to only be able to lead a women’s heart program, for example. While women’s heart programs are critically needed, they are not be our sole career option.
While the field admittedly is intense, cardiology has many career options. There are a number of subspecialties that allow for a better balance of work-life — from preventative care and the management of lipids and high blood pressure, to doing catheter-based interventions in heart attack patients or those with rhythm disorders. There are also more choices in how we practice: solo practitioners versus members of group practices, or office versus hospital-based.
In a Viewpoint from the same JAMA issue, the author writes that more than half of women in cardiology have been asked during interviews about their intention to have children. For medical students, the decision to have children is large — it often means an interruption in intensive training that can be very difficult to make up.
When I was in training, it was practically unheard of for anyone to have children, and there were absolutely no resources for childcare or maternity leave. I chose to wait until after my training to have my children — a now 32-year-old son and 31-year-old daughter. I chose a job in imaging that allowed me a “normal” schedule, and the time I needed to be both a mother and “Dr. Gillam.”
But because of the groundswell of support from the professional community for more female cardiologists, more hospitals and training programs are implementing maternity or family leave policies that make it possible for women to complete their training.
At Atlantic Health System, for example, we work with women who want to have a family to create training schedules on an individual basis and are committed to figuring it out together. At present, four out of nine cardiology fellows are women.
While many programs still require expectant mothers to take sick or paid leave time before these policies take effect, this is an example of the way the profession is changing to encourage more women to enter the field.
We are becoming increasingly supported by medical professional societies dedicated to encouraging more women to go into medicine. This is true in the U.S., Canada, Europe and elsewhere in the world. The American College of Cardiology (ACC) has a Women in Cardiology Section, and I have been active in the Women in Cardiology Committee of the American Heart Association (AHA). Other groups, such as the Society for Catheterization and Angiography (SCAI), and a new international organization called Women as One have also taken on this issue.
Together, we are committed to not only changing the perception of what having a career in cardiology and a family life means for women, but providing strong female mentors who can share their own journeys, lend support and mentor the next generation of young female cardiologists.
Some of the steps we are taking include formal leadership training, mentorship programs, and conducting studies to better understand decision-making about how women choose specialties and subspecialties. We are reaching out to physicians to create a databank of women who are available to speak and serve on advisory boards. We are asking professional societies to actively look at ways to establish gender equity (as well as ethnic and racial equity) as they assign speaking roles, podium opportunities and editorial opportunities in their professional society journals and meetings.
As women are taking more leadership roles in industry, support across the pharmaceutical, biopharmaceutical and medical technology industries has also been increasing. I credit much of this discussion and spirit of empowerment to the #MeToo movement, and the importance of banding together to encourage and support each other.
Today, I have a strong support network of colleagues and mentors (many of them men!) that I go to for guidance, support or clinical decision making. I also speak to them about their journeys.
I did sacrifice. In the 19 years my children were growing up until the point they left for college, I didn’t change jobs and I traveled little. I did stay in close contact with my professional colleagues, but in ways that did not require me to travel.
When my youngest left for college, I made up for lost time. I took a job at Columbia in a mainstream academic program, went back to school and earned my MPH in health policy and management, and got very involved in professional organizations. I also took advantage of speaking opportunities, editorial opportunities — all of the things I had to say no to in earlier parts of my career. I am friendly with a number of now-prominent female cardiologists who have the same types of stories.
What I tell my mentees, and those who speak with me about my career, is that you can’t have everything at the same time, but if you think things through, you can have most things, just at different stages of your career.
There is an exceptional amount of room for women in cardiology, and a strong support network of people who are willing to work with young women to “have it all” in this male-dominated field.
I look forward to the day when I will read the headline, “More Women Choosing Cardiology,” and supporting them when they do.
About the author: Linda D. Gillam, M.D., MPH, FACC is the Dorothy and Lloyd Huck Chair of Cardiovascular Medicine at Morristown Medical Center/Atlantic Health System and professor of medicine at the Sidney Kimmel Medical College at Thomas Jefferson University. She recently completed a term as chair of the Women in Cardiology Committee of the American Heart Association and serves on the leadership committee of the AHA Council on Clinical Cardiology. Under Gillam’s leadership, Atlantic Health System and Morristown Medical Center have become nationally recognized as leaders in cardiovascular medicine and surgery, attracting best-in-class talent, state-of-the-art technology and clinical trials.
Related Women in Cardiology Content:
Women Breaking the Glass Ceiling in Structural Heart



 May 12, 2026
May 12, 2026