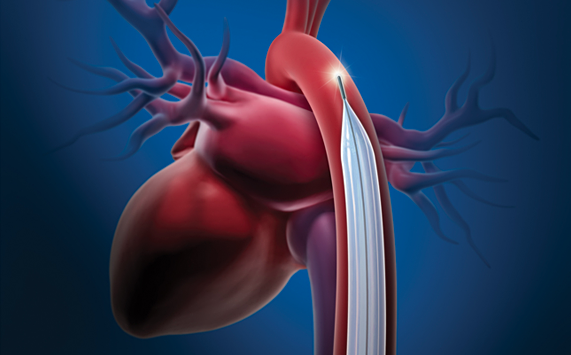
Cardiologists who have experience with COVID-19 patients in New York City say a low threshold should be used to assess patients for cardiogenic shock in the setting of acute systolic heart failure related to COVID-19. If inotropic support fails in these patients, researchers suggest use of an IABP (intra-aortic balloon pump) as the first line mechanical circulatory support device, because it requires the least maintenance from medical support staff.
April 8, 2020 — Research to help increase awareness of the cardiovascular manifestations of COVID-19 disease and the adverse impact of cardiovascular involvement on prognosis was published in Circulation April 3, the journal of the American Heart Association (AHA).
In the article "The Variety of Cardiovascular Presentations of COVID-19," the team of 18 New York City physicians note novel coronavirus (COVID-19, SARS-CoV-2) can involve the cardiovascular system in a variety of ways.[1] The researchers said there are evolving considerations for treatment across the spectrum of patients with pre-existing cardiovascular diseases. The researchers also detail four case studies of patients to illustrate the multiple cardiovascular presentations of COVID-19 infection.
"We tried to put together some of the observations we noted in our early experiences in these patients at out center with manifestations of COVID-19," explained Justin Fried, M.D., Attending cardiologist at Columbia University Irving Medical Center, New York City, and assistant professor at at Columbia University and lead author on the report. "We are seeing significant cardiac involvement, but it is important to note that many of our patients with underlying cardiovascular disease, notably heart failure and coronary disease, are developing significant effects form COVID-19 that is destabilizing conditions, and that presents unique challenge. I worry most about our patients who have underlying cardiovascular disease, which can be exacerbated by COVID-19."
The first patient presented predominately with cardiac symptoms with secondary respiratory symptoms and what appeared to be a case of classic myocarditis. Coronary angiography showed no blockages in the coronary arteries. The patient was treated with supportive care just for the COVID-19 and improved, along with increased left ventricular function, Fried said.
The second patient primarily had respiratory symptoms with acute respiratory distress syndrome (ARDS) requiring veno-venous extracorporeal membrane oxygenation (VV-ECMO). Cardiology was brought in after the patient experienced hemodynamic instability depressed left ventricular function. The patient was put on veno-arterial-venous (VAV)-ECMO.
"This case was more related to the profound cytokine storm that we are seeing in many of the COVID-19 patients, which shows some the challenges we are facing in these patients," Fried said.
The third case came in with some cardiac disease and developed polymorphic ventricular tachycardia while receiving medication to treat COVID-19, including azithromycin, which is known to cause QT prolongation. "It is very pertinent because the medications that are being advocated to treat the virus do have specific cardiac considerations we need to keep in mind," Fried explained.
The fourth patient in the study was a heart transplant patient who contracted COVID-19.
Key Observations in Cardiovascular Presentations of COVID-19 in New York City
The authors’ take-home messages are from the study were:
• In patients presenting with what appears to be a typical cardiac syndrome, COVID-19 infection should be in the differential during the current pandemic, even in the absence of fever or cough.
• One should have a low threshold to assess for cardiogenic shock in the setting of acute systolic heart failure related to COVID-19. If inotropic support fails in these patients, we consider IABP (intra-aortic balloon pump) as the first line mechanical circulatory support device because it requires the least maintenance from medical support staff.
• When patients on veno-venous extracorporeal membrane oxygenation (VV ECMO) for respiratory support develop superimposed cardiogenic shock, the addition of an arterial conduit at relatively low blood flow rates may provide the necessary circulatory support without inducing LV distension. Our experience confirms that rescue of patients even with profound cardiogenic or mixed shock may be possible with temporary hemodynamic support at centers with availability of such devices.
• COVID-19 infection can cause decompensation of underlying heart failure, and may lead to mixed shock. Invasive hemodynamic monitoring, if feasible, may be helpful to manage the cardiac component of shock in such cases.
• Medications that prolong the QT interval are being considered for COVID-19 patients and may require closer monitoring in patients with underlying structural heart disease.
• Our heart transplant recipient exhibited similar symptoms of COVID-19 infection as compared to the general population. For those transplant patients requiring hospitalization, how to alter the anti-metabolite and immunosuppression regimens remains uncertain.
• Furthermore, the COVID-19 pandemic creates a challenge for the management of heart failure patients on the heart transplant waitlist, forcing physicians to balance the risks of delaying transplant with the risks of donor infection and uncertainty regarding the impact of post-transplant immunosuppression protocols.
There have been reports of COVID-19 patients going into cardiogenic shock after they begin to recover from pulmonary distress, but Fried said this is not a common occurrence in the patients they have treated at Columbia.
"We have seen cardiogenic shock in some of these patients, but it is quite rare to have just isolated cardiogenic shock. Many of these patients do present with mixed shock," Fried said. "There is also a question if we are under diagnosing cardiogenic shock."
He said most of the shock seen in these patients is vasodilatory. In some cases, they used PA hemodynamic monitoring catheters to get a better picture.
Hear more from the interview with Fried in the VIDEO: Multiple Cardiovascular Presentations of COVID-19 in New York.
Co-authors include Justin A. Fried, M.D.; Kumudha Ramasubbu, M.D.; Reema Bhatt, M.D.; Veli K. Topkara, M.D., M.Sc.; Kevin J. Clerkin, M.D., M.Sc.; Evelyn Horn, M.D.; LeRoy Rabbani, M.D.; Daniel Brodie, M.D.; Sneha S. Jain, M.D., M.B.A.; Ajay Kirtane, M.D., S.M.; Amirali Masoumi, M.D.; Koji Takeda, M.D., Ph.D.; Deepa Kumaraiah, M.D., M.B.A.; Daniel Burkhoff, M.D., Ph.D.; Martin Leon, M.D.; Allan Schwartz, M.D.; Nir Uriel, M.D.; M.Sc.; and Gabriel Sayer, M.D.
Related Cardiology Related COVID-19 Content:
VIDEO: Cancelling Non-essential Cardiac Procedures During the COVID-19 Outbreak — Interview with Ehtisham Mahmud, M.D.
ACC COVID-19 recommendations for the cardiovascular care team
VIDEO: What Cardiologists Need to Know about COVID-19 — Interview with Thomas Maddox, M.D.
COVID-19 Hydroxychloroquine Treatment Brings Prolonged QT Arrhythmia Issues
FDA Approves ECMO to Treat COVID-19 Patients
The Cardiac Implications of Novel Coronavirus
ESC Council on Hypertension Says ACE-I and ARBs Do Not Increase COVID-19 Mortality
VIDEO: Imaging COVID-19 With Point-of-Care Ultrasound (POCUS)
CT Provides Best Diagnosis for Novel Coronavirus (COVID-19)
Radiology Lessons for Coronavirus From the SARS and MERS Epidemics
Deployment of Health IT in China’s Fight Against the COVID-19 Epidemic
Radiologists Describe Coronavirus CT Imaging Features
Coronavirus Update from the FDA
CT Imaging of the 2019 Novel Coronavirus (2019-nCoV) Pneumonia


 March 04, 2026
March 04, 2026 









