September 25, 2018 – New data demonstrate the correlation between the presence of non-flow-limiting, non-intervened-upon, lipid-rich plaques and the development of a major adverse cardiac event (MACE) from a de novo culprit lesion. The correlation was detected at both the patient level (vulnerable patients) and segment level (vulnerable plaques) with near infrared spectroscopy-intravascular ultrasound (NIRS-IVUS) within 24 months post-intravascular imaging.
Findings were reported at the 30th annual Transcatheter Cardiovascular Therapeutics (TCT) scientific symposium, Sept. 21-25 in San Diego.
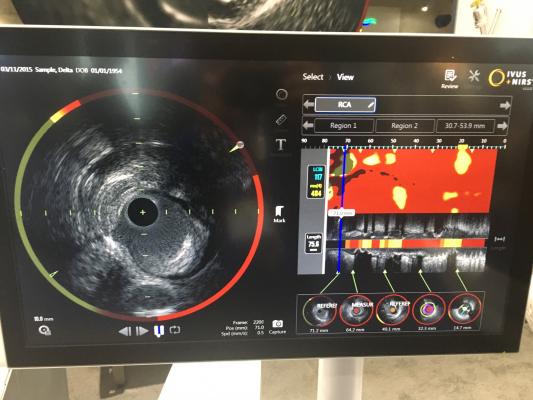
Coronary lipid-rich plaques may be associated with subsequent cardiovascular events, and it has been hypothesized that the outcome post-percutaneous coronary intervention (PCI) could be improved by the detection and subsequent treatment of vulnerable patients and lipid-rich vulnerable coronary plaques. Intravascular near-infrared spectroscopy (NIRS) is available as a dual modality catheter with simultaneous, co-registered intravascular ultrasound (IVUS).
“Multi-vessel NIRS can be easily and safely performed to assess and identify vulnerable patients and vulnerable plaques,” said Ron Waksman, M.D., associate director of the Division of Cardiology at MedStar Heart Institute in Washington, D.C. “Intravascular NIRS imaging in mildly or non-obstructive coronary arteries can be used as a tool to identify both patients and nonculprit arteries at high risk for future events and should be considered for use in patients undergoing cardiac catheterization with possible PCI.”
Watch a VIDEO interview with Waksman at TCT 2018 on the results of the trial.
From February 2014 to March 2016, a total of 1,563 patients with suspected coronary artery disease who underwent cardiac catheterization with PCI for an index event were enrolled at 44 sites in the United States and Europe. Imaging by NIRS-IVUS was performed in two or more arteries, and patient level and plaque level events were detected for two years. All patients with at least one maxLCBI4mm segment greater than or equal to 250, and a randomly selected 50 percent of patients with all maxLCBI4mm segments less than 250, were followed.
In the vulnerable patient-level analysis, the risk of experiencing non-culprit MACE event within 24 months was 18 percent higher with each 100 unit increase in maxLCBI4mm. Patients with maxLCBI4mm ≥400 had a MACE rate of 12.6 percent compared with 6.3 percent for patients with maxLCBI4mm˂400. In the vulnerable plaque-level analysis, the risk of experiencing an event in a coronary segment within 24 months was 45 percent higher with each 100 unit increase in maxLCBI4mm. Plaque with maxLCBI4mm ≥400 had a MACE rate of 3.7 percent compared to 0.8 percent for plaque with maxLCBI4mm˂400.
The LRP study was funded by Infraredx Nipro Company. Waksman disclosed that he is on advisory boards for Abbott Vascular, Amgen, Boston Scientific, Medtronic, Philips Volcano, PiCardia LTD and Cardioset; a consultant for Abbott Vascular, Amgen, Biosensors, Biotronik, Boston Scientific, Medtronic and Philips Volcano; and received grant support from Abbott Vascular, AstraZeneca, Biosensors, Biotronik, Boston Scientific and Chiesi. In addition, he is part of the AstraZeneca and Chiesi speaker’s bureaus; and is an equity holder in MedAlliance, DOMed, Pi-Cardia LTD and Cardioset.
For more information: www.crf.org


 May 06, 2026
May 06, 2026 









