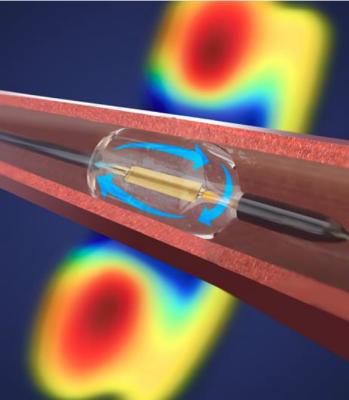
An illustration of the Recor renal denervation ablation balloon at work in the renal artery.
November 9, 2021 — Six-month outcomes from the randomized RADIANCE-HTN TRIO Trial comparing endovascular ultrasound renal denervation (RDN) to a sham procedure for treatment-resistant hypertension (HTN) found that the addition of a pharmacologic intervention led to further blood pressure reductions after RDN with a smaller increase in additional medications prescribed and less use of diuretics.
Findings were reported at the 2021 Transcatheter Cardiovascular Therapeutics (TCT) annual scientific symposium of the Cardiovascular Research Foundation (CRF).
“Blood pressure reductions after RDN were achieved with a smaller increase in additional medications prescribed and less use of aldosterone antagonists compared with a sham procedure,” said Ajay J Kirtane, M.D., S.M., professor of medicine at the Columbia University Vagelos College of Physicians and Surgeons, chief academic officer at Columbia University Interventional Cardiovascular Care and director at NewYork-Presbyterian/Columbia University Irving Medical Center’s Cardiac Catheterization Laboratories. “These results demonstrate the additional effects of pharmacologic intervention with maintenance of a BP-lowering effect of endovascular ultrasound RDN at six months.”
Patients with HTN require a multi-faceted approach for blood pressure control. In RADIANCE-HTN TRIO, patients with daytime ambulatory systolic blood pressure (dASBP) 135/85 mg Hg despite a fixed dose combination pill consisting of a calcium channel blocker, angiotensin receptor blocker, and thiazide diuretic, were randomized to RDN (n=69) or sham procedure (n=67). Presented at ACC 2021 and published in The Lancet, two-month results found that, in conjunction with the three-drug fixed-dose combination pill, RDN reduced dASBP by an additional 8 mm Hg, a 4.5 mm Hg greater reduction compared with a sham procedure (–8.0 mm Hg versus –3.0 mm Hg; median between-group difference –4.5 mm Hg; adjusted p=0.022).
During months two through five, the addition of a standardized stepped-care antihypertensive treatment (SSAHT) was recommended sequentially with the addition of spironolactone 25 mg/d, bisoprolol 10 mg/d, full dose of a centrally acting α2 receptor agonist, and an α1 receptor blocker if monthly measured home blood pressure was ≥135/85 mm Hg, with the goal of achieving blood pressure control in both groups. Adherence to prescribed medications was similar in both groups (71% for RDN versus 78% for sham, p=0.41).
The increase in the number of anti-hypertensive medications at six months following the addition of the SSAHT was 0.7 ± 1.0 for RDN and 1.1 ± 1.1 for sham (p=0.045). The use of aldosterone antagonists at two months was 3% for RDN and 11% for sham (p=0.16). At six months, the number increased in both groups but to a lesser extent in the RDN group (40% for RDN compared to 60.9% for sham, p=0.017).
The addition of the stepped care antihypertensive regimen to the initially randomized therapy further decreased blood pressures in both arms; the overall change from baseline in dASBP was -11.8±14.2 mm Hg in the RDN group versus -12.3±14.2 mm Hg for sham (p=0.65). Home blood pressure was lower in patients initially randomized to RDN when adjusted for baseline BP and number of medications (-4.28 mmHg, p=0.027). Safety outcomes were similar for both groups.
The study was funded by ReCor Medical. Kirtane reported institutional funding to Columbia University and/or Cardiovascular Research Foundation from Medtronic, Boston Scientific, Abbott Vascular, Abiomed, CSI, CathWorks, Siemens, Philips, ReCor Medical and Neurotronic. In addition to research grants, institutional funding includes fees paid to Columbia University and/or Cardiovascular Research Foundation for consulting/speaking. Personal disclosures include travel expenses/meals from Medtronic, Boston Scientific, Abbott Vascular, Abiomed, CSI, CathWorks, Siemens, Philips, ReCor Medical, Chiesi, OpSens, Zoll, and Regeneron.
Links to All the TCT 2021 Late-Breaking Clinical Trials
Related Renal Denervation Therapy Content:
Renal Denervation Lowers Blood Pressure in Medication-Resistant Hypertension
PCR Says Renal Denervation Offers Hope for Noncompliant Hypertension Patients


 October 31, 2025
October 31, 2025 









