The fingerprints of value-added medicine were all over products and works-in-progress on the exhibit floor of the annual meeting of the American College of Cardiology (ACC). From computed tomography (CT) to information technology (IT), positron emission tomography (PET) to deep learning algorithms, vendors sought to demonstrate how cardiology could be more efficient, more effective and convenient or comfortable for the patient. This dualistic, yin-and-yang approach — yin for administrators and providers; yang for patients — could be seen all over the ACC exhibit floor.
Cardiac CT Advances
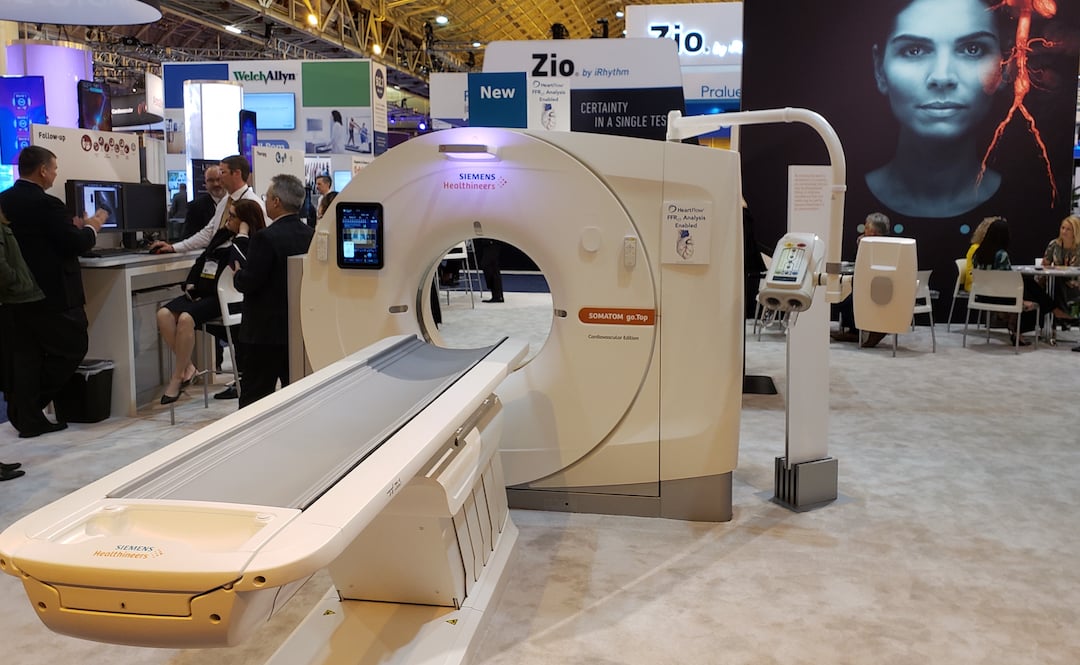
From the exhibit floor, Siemens launched a version of the
go.Top CT scanner dedicated for cardiology, its compact footprint and pricing (south of $800,000) is designed to fit the physical spaces of outpatient centers and their budgets. The underlying Go platform suits patients as well with a gantry-hung PC tablet that can take the place of control room and, thereby, allows the technologist to spend more time directly with patients. (A radiological version of the 128-slice Siemens go.Top was released at the Radiological Society of North America (RSNA) 2017 meeting.) In line with its patient centricity is the CARE kV feature, which optimizes radiation dose and image contrast and its Check&GO algorithm, which helps identify problems with anatomical coverage and the distribution of media contrast.
Although optimized for outpatient cardiology offices, the cardiovascular (CV) version of the CT might also be installed in hospitals, according to Matthew Dedman, Siemens’ director of CT product marketing. Siemens has developed a technical solution that optimizes data transmission from the scanner to the company HeartFlow, where CT-based fractional flow reserve (FFR) analyses may be conducted. This solution can then be leveraged for the transmission of results back to the physician.
Similarly, GE Healthcare directed booth goers to its
Cardiographe, a CT scanner launched some two years earlier. Philippe Karam, GE’s global sales and marketing director, noted the CardioGraphe’s dedication to cardiology and cost-effectiveness, stating that the system had been built specifically for the cardiology market. It can be used to plan procedures including transcatheter aortic valve replacement (TAVR), according to Kira Behrens, GE’s director of premium CT for the U.S. and Canada. Dose efficiency is achieved using a cardiovascular version of GE’s ASiR (adaptive statistical iterative reconstruction) software.
Priced under $800,000, the CardioGraphe — which installs in as little as 15 square meters — can typically fit in outpatient clinics, emergency departments, a large interventional lab, or even physician offices, according to the company. In a single heartbeat, the dedicated CV scanner can create a 3-D image of the coronaries, valves, chambers and myocardium, as well as an angiogram of the aorta. Rotation speed is 0.24 seconds; single-beat heart coverage 140 mm, and resolution 0.28 mm, according to the company.
Also on the ACC show floor, Circle Cardiovascular Imaging was talking up smart algorithms to extend the use of cardiac MRI and CT. The goal, according to Circle’s Tom Gardner, is to make life easier for cardiologists and radiologists, mostly in cardiac MRI space but also in cardiac CT. “We have offered and introduced deep learning into our application so that we can speed up and actually improve the processing for some of the studies that you want to look at,” said Gardner, sales director for North America.
In the algorithms, the company leverages deep learning — a type of artificial intelligence (AI) — to calculate ejection fraction and stroke volumes, for example, from cardiac MRI. These algorithms take over such tedious manual processes as drawing contours, a process that is not only tedious but time-consuming, “so you can spend your time really understanding patients’ needs,” he said.
New Innovation May Expand Cardiac PET
PET has evolved mostly as an oncologic imaging modality with potential in cardiology. At ACC.19, Jubilant DraxImage was working to realize at least some of that potential, promoting its Ruby-Fill (Rubidium Rb82 Generator) product for cardiac PET.
“We believe that a product that is safe and efficient and has dosing flexibility is going to probably make (PET) more convenient to use (in cardiology),” said Lisa Shearin, cardiovascular marketing director for Jubilant Draximage. “We see people who have been using PET typically in oncology trying to carve out spaces — maybe a day or half-day — to image cardiac patients.”
The flexible dosing possible with Ruby Fill, which has a 60-day shelf life, could overcome time limitations that might keep PET on the cardiac sideline. “You can have confidence that on day 57, for example, you’re going to get the same type of images as you did on day one or two,” she said.
Ruby Fill is installed in about 20 sites in North America, according to Shearin, a number she said could double by the end of the year. Shearin said she hopes that a 2016 position statement from the American Society of Nuclear Cardiology (ASNC) that describes myocardial perfusion PET as a “first-line preferred test” for certain patients will accelerate cardiac adoption.
Precision Medicine Shines On ACC Exhibit Floor
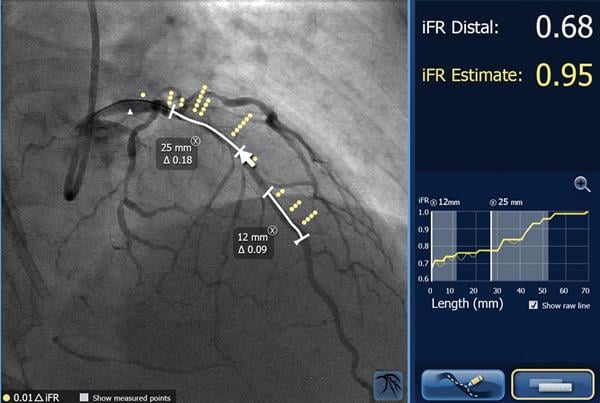
Philips framed need — and value — of a product in its portfolio with results from an international study presented during the ACC meeting. The study concluded blood flow restrictions remained in coronary vessels in as many as 25 percent of patients who underwent coronary interventions. Importantly, the lesions that caused these restrictions could be localized using a technology called iFR (instantaneous wave-free ratio, also referred to as instant wave-free ratio or instant flow reserve, an easier to use version of FFR).
When localized, the lesions might be resolved, according to Justin Davies, Ph.D., a consultant cardiologist in the Division of Cardiology Cardiothoracic and Thoracic Surgery at Imperial College Healthcare NHS Trust in London, who invented the technology. Davies explained that pressure sensors located at different points along the iFR wire may show differences in pressure. These differences may be apparent when the iFR wire is pulled back from the initial treatment site.
“With IFR, you know not only that you need to treat this patient but also where to treat,” said Bert van Meurs, Philips’ chief business leader for image-guided therapy.
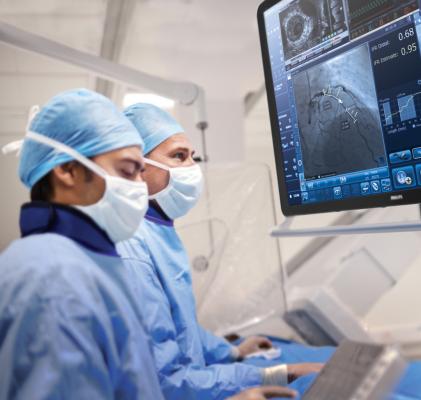
If the pressure drops, the interventionalist knows that residual stenosis occurs somewhere between the two pressure sensors. Philips SyncVision iFR Co-registration product maps the pressure readings onto angiograms, allowing interventionalists to see where in the artery the lesion is likely located.
The iFR technology is already used in cath labs around the world to determine the severity of these coronary restrictions. Philips, which sponsored the study that demonstrated the extended value of iFR, has licensed this technology from the Imperial College. Philips looks at “the total procedure and how we can help to develop more integral solutions to address that specific patient in a more effective way,” said van Meurs, who noted that the company focuses on the combination of imaging and intervention.
The study, which was conducted at major U.S. and European medical centers, showed that the positive effects of coronary interventions in patients suffering from coronary artery disease may be limited by residual lesions. The study suggests that patient outcomes might be improved if the locations of these residual stenoses could be determined.
Most vascular interventions begin with access through the femoral artery. At ACC 2019, Terumo Interventional Systems promoted radial access through the wrist as a safe and cost-effective alternative. Access through the radial artery has been constrained, however, by the relatively few interventional devices compatible with it.
3D Systems laid about a dozen different simulators on tables at its ACC booth. Simulations, said company rep Michelle Halsne, are critically important to achieving good outcomes. “The first time you see an aortic dissection, you hope it is not on your patient,” said Halsne, regional sales manager for medical simulation at 3D Systems, which she estimated has sold about 3,000 simulators worldwide, many of them to educational facilities. “You build confidence and competence and skills for patient one to patient 10,000.”
The simulators used wires and catheters to provide the tactile feeling of a real intervention. Although virtual reality (VR) simulations were not apparent at the company’s ACC booth, VR is integrated in some simulators to provide a visual sense, she said. “(Interventionalists) are seeing it as though they are working on a patient,” said Halsne, who noted that tactile feedback is an important part of VR. The VR simulation, she said, “feels just like they are pushing the wire through. If they are doing a chronic total occlusion case, (the occlusion) is going to fight back, just like it would in a real case.”
Linking Multiple Modalities By Integrating Data
Philips’ angiographic platform, called Azurion, is more focused on the interventional procedure than the imaging modality, according to van Meurs. Azurion combines angiography with other technologies, such as iFR, in ways that optimize workflow. “The focus is on innovating the procedure and not just innovating one imaging modality,” Van Meurs said.
Combining data from multiple modalities may include co-registering recently acquired CT and real-time echo images. GE Healthcare showed how its Vivid E95 cardiovascular ultrasound could fuse echo and CT data. CT data has proven useful when planning interventional procedures, “but we had lost that data when we were in the (interventional) lab,” said Jake Dewees, clinical commercial marketing manager for GE ultrasound. GE’s fusion feature on the E95 CV ultrasound system, a feature that was commercially released in January 2019, fixes that.
And the CT data does not have to come from a GE scanner. “You can take anybody’s 3-D CT data set and download that into the (E95) and have that available to you during the case,” said Al Lojewski, vice president and general manager of the GE cardiovasular ultrasound.
Similarly, Philips showcased the integration of CT on its Epiq-CVx ultrasound system, which allows the user to navigate through the fused CT-echo image. Data from a third modality, digital angiography, can also be co-registered onboard this newly updated version of Philips’ high-end echo system, which the company showed at the ACC along with a new 3-D transesophageal echo probe.
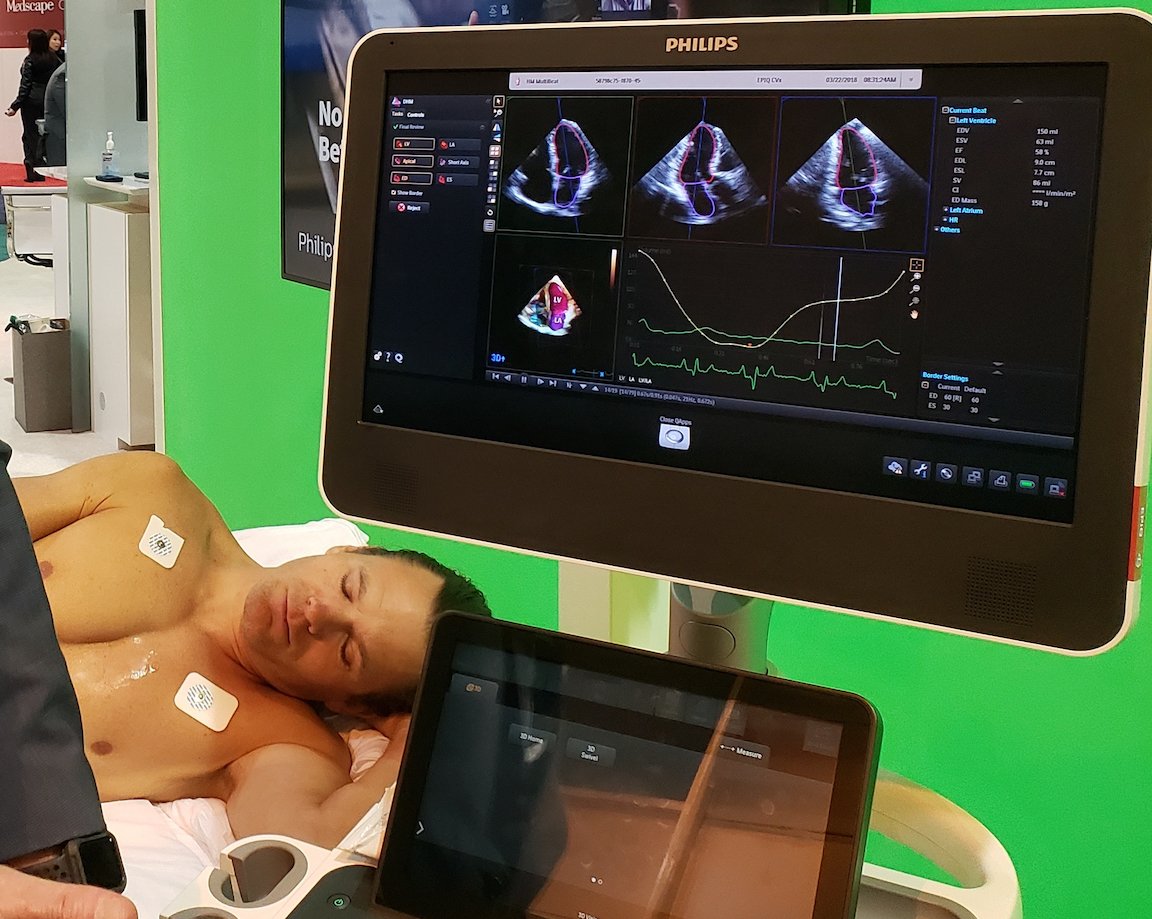
Particularly intriguing on the Epiq-CVx is the “dynamic heart model” feature, which automatically calculates 3-D ejection fraction and chamber volumes. “You want to let the machine do everything,” said Steven Blankenship, a Philips applications specialist. Blankenship noted that the automatic calculations add consistency and reproducibility. “The artificial intelligence of the machine is doing all the work,” he said.
AI-based algorithms can pick the most relevant echo views to assess on GE’s Vivid 95E, according to Lojewski. Using the algorithms, which were developed using GE’s Edison platform, he said, “reduces the amount of time that (physicians and sonographers) are spending and it improves the consistency (from scan to scan). You want to make it as simple as you can. That is what we are doing. (The machine) picks the views for you and you can spend more time with the patient reviewing their chart.”
The automation achieved through artificial intelligence is not being done for the sake of AI but rather to reach a higher goal. This is nothing new. The industry has long sought increased efficiency and effectiveness through automation.
Such efforts are evident not just in recently developed smart algorithms but in the development of technology that promotes the fuller use of modalities, from the use of PET imaging in cardiac applications to the building of dedicated cardiac CTs using parts of other premium scanners.
Enterprise Imaging Stands Out
Certain other products could be stratified into separate classes. Among them is enterprise imaging. Change Healthcare described efforts to develop a cloud-enabled vendor neural archive, which the company plans to take live for initial customers this summer.
The goal is to make the cloud-enabled VNA an informatics backbone compatible with the company’s own offerings and those of third-party vendors, mostly using standards-based interfaces, “where standards exist,” said Ori Garini, director of product management for cardiology. “Where they don’t, we have a very good mechanism for creating propriety interfaces.”
Aaron Green, general manager of the Change Healthcare cardiology division, expects to initially take about a half dozen sites to the cloud. This will spread, eventually, to most or all Change customers. The company has a substantial installed base, about 20 percent of the total market in North America; the whole country of Ireland; 90 percent of the cardiology trusts in the United Kingdom; and “large cardiology footprints” in Australia and Germany, Green said, “I would say you are going to see a massive shift within the market over the next five years to cloud-based solutions.”
At ACC 2019, Philips showcased the latest version of its Intellispace Cardiovascular, an image and information management system designed specifically for cardiology. Key features include the integration of images and data from multiple modalities amid streamlined workflow to help improve operational performance from the cath lab to nuclear medicine, electrophysiology to stress echo.
A standout is the system’s timeline, which serves up a graphical and chronological overview of patients — and provides “launch points” from which patient records can be obtained. Images and data about patients, as well as a worklist of cases, can be viewed in the Intellispace Cardiovascular Workspace.
Standards-based interconnectivity is the lever of choice, as Philips works with customers and third-party vendors to create a seamless informatics environment, according to Jon Kamerman, Phillips senior market manager.
Editor's Note: Greg Freiherr is a contributing editor to Imaging Technology News (ITN) and Diagnostic and Interventional Cardiology (DAIC). Over the past three decades, Freiherr has served as business and technology editor for publications in medical imaging, as well as consulted for vendors, professional organizations, academia and financial institutions.
Related ACC 2019 Content:
VIDEO: Use of an Antibacterial Envelope to Reduce Infections for Pacemakers, ICDs — Interview with Khaldoun Tarakji, M.D.
PODCAST: Fitting Artificial Intelligence Into Cardiology — Interview with Anthony Chang, M.D.
Sunday ACC 2019: Mixed Reality Offers Advantages of Virtual and Augmented Realities
VIDEO: Key Trends in Electrophysiology — Apple Watch to Detect AF and the CABANA Trial — Interview with Christine Albert, M.D.
Video Game Format Used to Train Cardiologists
PODCAST: How Technology Is Changing Cardiology — Interview with Partho P. Sengupta, M.D.,
VIDEO: Why Are There So Many Foreign Doctors? — Interview with William Pinsky, M.D., and Mandeep Mehra, M.D.,
PODCAST: Shortcomings of CTA in Cardiology — Interview with Todd C. Villines, M.D.
VIDEO: Use of Wearables to Track Electrophysiology Patients — Interview with Khaldoun Tarakji, M.D.
Saturday ACC 2019: How Machine Learning Empowers Echo Users Today
ACC.19 Future Hub Hosts “Shark Tank” of Emerging Technologies In Cardiology
VIDEO: Characterization of Cardiac Structural Changes and Function Following Radiation Therapy — Interview with Magid Awadalla, MBBS
PODCAST: Choosing CTA Over Functional Requires Judgment Call — Interview with Rami Doukky, M.D.
VIDEO: Utilization of PET For Evaluation of Cardiac Sarcoidosis — Interview with Raza Alvi, M.D.
 From the exhibit floor, Siemens launched a version of the go.Top CT scanner dedicated for cardiology, its compact footprint and pricing (south of $800,000) is designed to fit the physical spaces of outpatient centers and their budgets. The underlying Go platform suits patients as well with a gantry-hung PC tablet that can take the place of control room and, thereby, allows the technologist to spend more time directly with patients. (A radiological version of the 128-slice Siemens go.Top was released at the Radiological Society of North America (RSNA) 2017 meeting.) In line with its patient centricity is the CARE kV feature, which optimizes radiation dose and image contrast and its Check&GO algorithm, which helps identify problems with anatomical coverage and the distribution of media contrast.
From the exhibit floor, Siemens launched a version of the go.Top CT scanner dedicated for cardiology, its compact footprint and pricing (south of $800,000) is designed to fit the physical spaces of outpatient centers and their budgets. The underlying Go platform suits patients as well with a gantry-hung PC tablet that can take the place of control room and, thereby, allows the technologist to spend more time directly with patients. (A radiological version of the 128-slice Siemens go.Top was released at the Radiological Society of North America (RSNA) 2017 meeting.) In line with its patient centricity is the CARE kV feature, which optimizes radiation dose and image contrast and its Check&GO algorithm, which helps identify problems with anatomical coverage and the distribution of media contrast. Philips framed need — and value — of a product in its portfolio with results from an international study presented during the ACC meeting. The study concluded blood flow restrictions remained in coronary vessels in as many as 25 percent of patients who underwent coronary interventions. Importantly, the lesions that caused these restrictions could be localized using a technology called iFR (instantaneous wave-free ratio, also referred to as instant wave-free ratio or instant flow reserve, an easier to use version of FFR).
Philips framed need — and value — of a product in its portfolio with results from an international study presented during the ACC meeting. The study concluded blood flow restrictions remained in coronary vessels in as many as 25 percent of patients who underwent coronary interventions. Importantly, the lesions that caused these restrictions could be localized using a technology called iFR (instantaneous wave-free ratio, also referred to as instant wave-free ratio or instant flow reserve, an easier to use version of FFR). Particularly intriguing on the Epiq-CVx is the “dynamic heart model” feature, which automatically calculates 3-D ejection fraction and chamber volumes. “You want to let the machine do everything,” said Steven Blankenship, a Philips applications specialist. Blankenship noted that the automatic calculations add consistency and reproducibility. “The artificial intelligence of the machine is doing all the work,” he said.
Particularly intriguing on the Epiq-CVx is the “dynamic heart model” feature, which automatically calculates 3-D ejection fraction and chamber volumes. “You want to let the machine do everything,” said Steven Blankenship, a Philips applications specialist. Blankenship noted that the automatic calculations add consistency and reproducibility. “The artificial intelligence of the machine is doing all the work,” he said.

 April 02, 2026
April 02, 2026 









