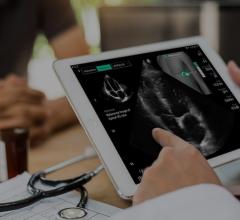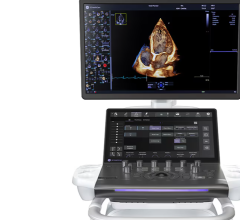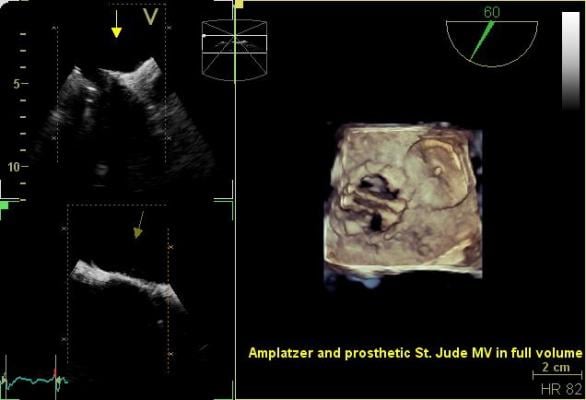
Philips introduced CX50 xMatrix architecture designed to support advanced fluoro integration with the EchoNavigator system. It aligns TEE views with live fluoroscopy to enhance navigation in complex structural heart procedures.
The development of 3-D transesophageal echo (TEE) just a few years ago has enabled a new generation of interventional procedures to be performed, which otherwise would have been extremely difficult or impossible. With live 3-D TEE, physicians can see cardiac structures and function, as well as real-time displays of the beating heart, from new perspectives.
TEE provides visualization of pathology and function that is immediately accessible and easier to interpret over 2-D images. TEE also offers more perspectives of the heart, the surgeon’s view and the view inside the left ventricle. This has made possible much more complex transcatheter structural heart procedures, which may replace open-heart surgical procedures in the years ahead.
Unlike traditional transthoracic echocardiography (TTE), 3-D TEE has a definite imaging advantage during complex interventions because it offers simultaneous bi-plane (also called X-plane) imaging, allowing visualization from two different angles. These views, displayed on the main screen in a cath lab or hybrid operating room (OR), better visualize the location of catheters and devices inside the heart more clearly than 2-D angiography.
“Over the past few years the use of 3-D and 4-D TEE has really exploded,” said Al Lojewski, vice president and general manager of GE Healthcare’s cardiovascular ultrasound unit. “It is used with all the new transcatheter structural heart procedures with mitral valve repair, LAA occlusion and TAVR. There are more and more devices and procedures now being introduced that use TEE for visualization.”
Guiding Transcatheter Structural Heart Procedures With TEE
3-D TEE has enabled more complex transcatheter procedures, such as closure of atrial septal defects (ASDs), ventricular septal defects (VSDs) and the left atrial appendage (LAA). TEE also is used to more accurately assess the placement and function of transcatheter aortic valve repairs (TAVR) and makes possible transcatheter mitral valve repair procedures, such as the MitraClip.
“It’s mandatory — these procedures require TEE. You can use 2-D TEE, but most of the recommendations are changing to advise use of 3-D TEE,” said Bijoy Khandheria, M.D., FACP, FESC, FASE, FACC, director of echocardiography services, Aurora Healthcare, advanced cardiovascular services, Aurora/St. Luke Medical Center, Aurora/Sinai Medical Center, Milwaukee. He is also past president of the American Society of Echocardiography (ASE). “I would imagine over the next year it will become mandatory to do these procedures using 3-D TEE.”
He said this is especially true of the MitraClip devices now before the U.S. Food and Drug Administration (FDA) for final review. The clip mimics an open-heart surgical suture repair, but requires the operators to use echo to grasp both leaflets of the valve at the same time. Positioning of the clip on the center of the valve and its orientation to leaflets is crucial.
“With the MitraClip, you can’t clasp the clip without TEE visualization,” Khandheria said. “If you do it with 2-D Tee, it can be done, but you need four different angles to see the clip for alignment before you can close the clip.”
He explained that even experienced TEE operators have issues getting all four views on 2-D TEE. “Usually you can only get two or three of the four positions, so you have to hope and pray you are on target,” he said. “In 3-D, you don’t have to reconstruct the image in your mind. It is also much easier to visualize the grasping of the valve leaflets.”
Beyond making procedures easier to visualize, Khandheria said 3-D TEE saves a lot of time. His experience has shown that 3-D can save between 60–70 percent of the time spent imaging with 2-D TEE. “It has to be a 3-D/4-D system, otherwise in six months you will realize how much longer it takes to do these procedures, and time is money,” he explained.
In TAVR, TEE helps accurately place the angiographic pigtail catheter in the noncoronary cusp of the aortic root. It also offers Doppler flow imaging to evaluate the hemodynamics of the valves and to check for paravalvular leaks. Khandheria said the FDA also requires use of 3-D TEE for proper sizing of the annulus in TAVR procedures.
With LAA occlusions, Khandheria explained it is just easier to view the anatomy and the device in 3-D than on four separate 2-D planes. In addition, he said the 3-D TEE is much easier to use when trying to see if the occluder is seating properly. For example, with the Lariat LAA occlusion system from SentraHeart, a balloon is used to help place the device, which lassos and remotely sutures the LAA closed. Khandheria said the trial for the device used 2-D TEE, which did not visualize pericardial effusions caused by the balloon pressure tearing the cardiac tissue. He felt the issue was under-reported in the trial for the device. But with newer 3-D TEE, he said physicians now check for effusions at Aurora and have caught two so far.
Intra-cardiac echo (ICE) is often used to help guide transseptal punctures, but Khandheria said TEE can be used instead. ICE also has been used to guide septal defect closures, but causes navigation issues because it cannot visualize the other side of the heart once the metallic implant is placed. For these reasons Aurora uses 3-D TEE to guide both of these procedures.
New Subspecialty of Interventional Echocardiography
The new uses of TEE, especially 3-D/4-D TEE, are raising the question in hospitals as to who should be operating these systems during procedures. Traditionally, the anesthesiologist performed 2-D TEE, but with use of 3-D/4-D TEE, Lojewski said it really requires an experienced echocardiographer who is familiar with the anatomy and can quickly obtain the view required by the interventionalist. However, Lojewski said you can not just tie up a physician in a hybrid OR for a procedure that takes up most of the day. The American Society of Echocardiography recognized this issue at its 2012 annual meeting. Several ASE presenters said the new specialty of interventional echocardiography will likely develop out of the increasing need for TEE during complex transcatheter procedures.
Khandheria moved from Mayo Clinic to help Aurora build its echocardiography program in 2008. Since then, and with the creation of an interventional structural heart program, Aurora saw a boost in TEE use from
29 percent of procedures in 2009, to 45 percent in 2011.
Aurora uses TEE with a dedicated echocardiographer as the operator integrated into its hybrid OR cardiac care teams. The healthcare system uses TEE to guide TAVR and MitraClip procedures, paravalvular leak repairs, septal defects and LAA occlusions, and to guide transeptal punctured at the start of EP ablation procedures. When delivering TAVR valves transapically, Khandheria said 3-D TEE is used to navigate the valve into position to ensure it goes through the left ventricle without damaging chordae tendineae or the mitral valve.
The rapid increase in these types of procedures nationally has given rise to a new subspecialty of interventional echocardiographers. “You need a different breed of people with a significantly different mindset to work in the cath lab or hybrid OR on structural heart cases,” Khandheria said. “Echocardiologists usually sit in a dark room all day reading echos. But, you can’t rewind a live echo and say ‘let me look at that again.’ You need to make instantaneous decisions in real-time. They need to be able to work closely with the interventional cardiologists as a part of the heart team and learn their lingo.”
Live 3-D TEE Advances
Philips took an early lead with 3-D TEE, being the first vendor to introduce the technology in 2008, and now has more than 2,500 of these systems installed in North America. In 2012, both GE and Siemens introduced 3-D TEE systems.
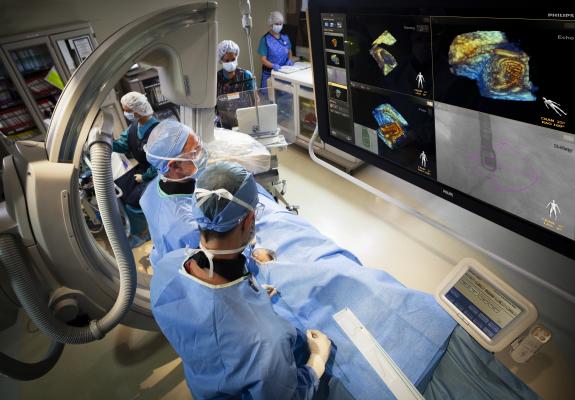
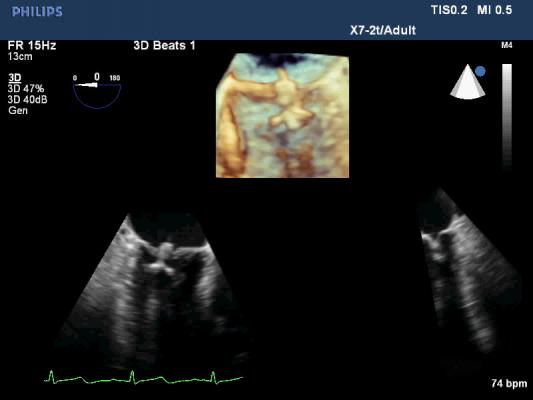
Philips recently announced its CX50 xMatrix portable ultrasound system that interfaces with its live 3-D TEE, which was previously only available with the larger iE33 xMatrix system. The smaller footprint of the CX50 xMatrix is expected to make it more competitive in the cath lab and hybrid OR environments, where space is often in short supply. The CX50 xMatrix architecture is designed to support advanced fluoro integration. Philips’ new EchoNavigator system (approved by the FDA last fall) aligns TEE views with live fluoroscopy to enhance navigation in complex structural heart procedures. The user can mark locations on a live TEE image, and then those marks precisely line up to show the location and image orientation on live fluoroscopy.
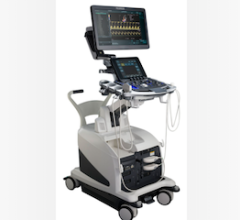
GE Healthcare’s new Vivid E9 Breakthrough 2012 (BT12) cardiac ultrasound system includes a 3-D/4-D TEE probe. It offers tools to improve workflow efficiency through simplified image acquisition. It is designed for intuitive navigation and advanced, yet easy-to-use, quantification. The new TEE probe allows 4-D dataset acquisitions to quickly visualize cardiac structures. It also helps quantify left ventricular pump function, myocardial deformation and mitral valve morphology. The probe includes triplane imaging, 4-D views and high frame rates.
With this new system, GE said it has focused on simplifying workflow and increasing ease-of-use. The system enables one-button acquisition of mitral valve images, rather than using the track ball and a combination of buttons to slice the image into different views. In bi-plane mode, it has the ability to tilt and rotate at the same time. A QuickRotate button provides consistency and accuracy by allowing users to rotate an image in 30-degree increments with a single click. The system also offers laser lines, a new tool to help understand the relationship between 2-D slices and 4-D views, helping visualize the linkage between 2-D and 4-D and improve depth perception.
Siemens released its fourSight TEE View, which enables 3-D acquisition, reconstruction and display at the point-of-care. Both 2-D and 3-D assessment can be combined with the use of a V5Ms transducer. Reconstruction can be done immediately or at a later date, either on the Acuson Sequoia ultrasound platform or offline with the syngo Ultrasound Workplace.
The system also features 3-D “en face” display, and 2-D and color Doppler display with measurement capabilities. It calculates 3-D hemodynamic volumes, area calculations and basic distance measurements.
Hemodynamic Management Via TEE
Gearing its TEE system for the critical care market, ImaCor Inc. calls its Zura system a hemodynamic transesophageal echocardiography (hTEE) management device. Hemodynamic management of critically ill patients is a challenge due to ineffective data, said the vendor, explaining cardiac filling pressures and flow data have limitations in the ICU, and the use of pulmonary artery catheters has declined due to ineffectiveness and increased patient safety risks.
ImaCor said direct visualization with hTEE is continuously available to optimize cardiac performance by reassessing volume, pressors, inotropes, ventilator settings and pulmonary vasodilators.
Patient selection for hTEE is risk-based relative to hemodynamic status. The objective is optimization of cardiac performance to maintain tissue perfusion and prevent organ dysfunction. Successful weaning of pharmacologic and mechanical circulatory support often requires the direct visualization of cardiac performance provided by hTEE. Assessment of LV filling and function, right ventricular function and fluid responsiveness is accomplished by obtaining three primary views: the mid-esophageal 4 chamber, the transgastric short axis and the superior vena cava. These views are the recognized gold standard for assessing hemodynamic status.
The ImaCor ClariTEE probe is purpose-built for critical care. Its miniaturized probe enables long-term patient management for up to
72 hours. It uses a disposable, detachable hTEE probe.
Related TEE Content:
360 View of the TEE Echo Workstation During a MitraClip Procedure
VIDEO: Developing New Cath Lab Technologies With Real-time Collaboration Between Industry, Doctors
Interventional Imagers: The Conductors of the Heart Team Orchestra
ASE Releases Guidelines for Transesophageal Echo in Congenital Heart Disease
VIDEO: The Role of Advanced Imaging in Structural Heart Interventions
VIDEO: Incorporation of 3-D Echo Into Peri-operative Practice
Recent Advances in Echocardiography Technology


 April 30, 2026
April 30, 2026