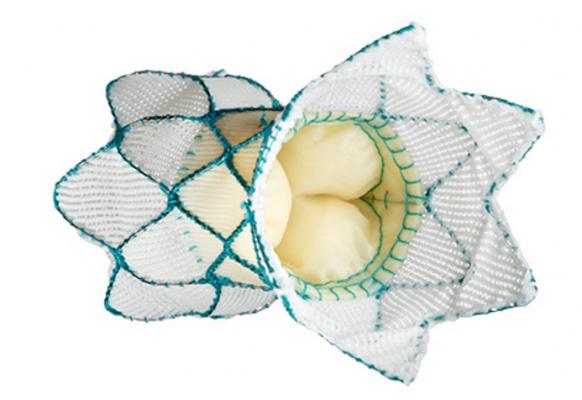
The Medtronic Harmony Transcatheter Pulmonary Valve (TPV) System is is designed for patients without a conduit with RVOT malformations who require a correction to their structural malformation early in life and need a minimally invasive option to restore pulmonary valve function.
March 26, 2021 — Today, the U.S. Food and Drug Administration (FDA) cleared the Medtronic Harmony Transcatheter Pulmonary Valve (TPV) System. It is first in the world non-surgical heart valve to treat pediatric and adult patients with a native or surgically-repaired right ventricular outflow tract (RVOT) to stop severe pulmonary valve regurgitation caused by Congenital heart disease.
The Harmony valve is intended to improve blood flow to the lungs in patients with severe pulmonary valve regurgitation (PR) without open-heart surgery, which is the current standard of care. The use of the Harmony valve may delay the time before a patient needs additional open-heart surgery. It can also potentially reduce the total number of open-heart surgeries required over an individual’s lifetime.
“Until recently, the only option for a patient that had severe PR after previous open heart surgery was to return to the operating room for another open heart surgical procedure, either a bioprosthetic Pulmonary Valve replacement or an RV-PA conduit,” said John P. Cheatham, M.D., lead principal investigator and professor emeritus, Department of Pediatrics, Cardiology at Nationwide Children's Hospital in Columbus, Ohio. He also serves as the lead principal investigator of the Harmony Trials. “The Harmony TPV therapy finally offered a non-surgical option to treat severe PR and restore pulmonary valve competence.”
The Harmony TPV device was granted FDA Breakthrough Device Designation for the treatment of pediatric and adult patients with severe pulmonary valve regurgitation. Breakthrough Device Designation is a process designed to expedite the development and review of devices that may provide for more effective treatment or diagnosis of life-threatening or irreversibly debilitating diseases or conditions.
“The Harmony TPV provides a new treatment option for adult and pediatric patients with certain types of congenital heart disease. It offers a less-invasive treatment alternative to open-heart surgery to patients with a leaky native or surgically-repaired RVOT and may help patients improve their quality of life and return to their normal activities more quickly, thus fulfilling an unmet clinical need of many patients with congenital heart disease,” said Bram Zuckerman, M.D., director of the Office of Cardiovascular Devices in the FDA’s Center for Devices and Radiological Health.
Congenital heart defects (CHDs) are conditions that are present at birth and can affect the structure of a baby’s heart and the way it works. They are the most common type of birth defect, affecting about 40,000 babies born each year. It is estimated that over two million infants, children, adolescents and adults are living with CHDs in the U.S. Patients with CHDs often require heart procedures early in life to help improve blood flow to the lungs. After having one of these procedures, the patient may or may not have a working pulmonary valve, which could lead to pulmonary regurgitation. Severe pulmonary valve regurgitation may be corrected through open-heart surgery to place a right ventricle-pulmonary artery conduit or an artificial valve.
During the implantation procedure of a Harmony valve is inserted through a vein in the groin or in the neck and into the right side of the heart, and then into the RVOT where it is placed into position. The self-expanding valve is then released from the catheter and anchors to the RVOT. Once the new valve is in place, it functions like the native valve to prevent the back flow of blood and ensure the flow in the correct direction.
Harmony Transcatheter Pulmonary Valve Clinical Trial Data
The FDA assessed the safety and effectiveness of the Harmony TPV device through the prospective, non-randomized, multi-center clinical study — The Medtronic Harmony Transcatheter Pulmonary Valve Clinical Study. During the study, physicians implanted the device in a total of 70 patients. All patients were scheduled for follow-up examinations at the start of the study, at implant procedure, discharge, and post implant at one month, six months, and annually through five years. The follow-up has been extended to 10 years as part of the post-approval study.
The primary safety endpoint was no procedure- or device-related death within 30 days following the implant, which 100% of patients attained. The primary effectiveness endpoint was percentage of patients with no additional surgical or interventional procedures related to the device and acceptable heart blood flow function at six months. Among patients with evaluable echocardiography data, 89.2% of them achieved the primary effectiveness endpoint.
Adverse events observed during the clinical study included irregular or abnormal heart rhythms (23.9%, including 14.1% ventricular tachycardia), leakage around the valve (8.5%, including 1.4% major leakage), minor bleeding (7.0%), narrowing of the pulmonary valve (4.2%), and movement of the implant (4.2%).
The Harmony TPV device is contraindicated for patients with an infection in the heart or elsewhere; patients who cannot tolerate blood thinning medicines; or patients who have sensitivity to Nitinol (titanium or nickel).
The Harmony TPV device was approved using the Premarket Approval (PMA) pathway. Premarket approval is the most stringent type of device marketing application required by the FDA and is based on a determination by the FDA that the PMA application contains sufficient valid scientific evidence to provide reasonable assurance that the device is safe and effective for its intended use(s).
The device was also part of the U.S.-Japan Medical Device Harmonization by Doing Collaboration, which seeks to promote timely access to innovative devices in both the U.S. and Japan through greater collaboration and communication among regulatory, academic and industry stakeholders across all stages of product development, and by developing practical solutions to shared real-world challenges.
Harmony Transcatheter Valve Will Join Melody Valve to Treat Pulmonary Valve Regurgitation
Typically in congenital heart patients with pulmonary valve issues, a subset of these patients will require open-heart surgery early in life to correct these malformations and some will receive a prosthetic conduit that increases blood flow from the heart to the lungs. Once the conduit is no longer functional, the Medtronic Melody transcatheter pulmonary valve can be implanted to restore pulmonary valve function and delay additional surgical intervention.
The Harmony TPV is designed for patients without a conduit with RVOT malformations who require a correction to their structural malformation early in life and need a minimally invasive option to restore pulmonary valve function.
The Melody was the first transcatheter valve implanted in a human anywhere in the world and the first transcatheter valve to be approved by the FDA under a humanitarian device exemption in 2010, predating the Sapien and CoreValve TAVR valves. Melody is the longest studied TPV with the largest body of evidence, with more than a decade of study data on long-term durability, safety and effectiveness.
For more information: www.medtronic.com/us-en/patients/treatments-therapies/transcatheter-pulmonary-valve-therapy
Related Transcatheter Valve Content:
FDA Clears Sapien for Pulmonary Valve
Medtronic Congenital Heart Transcatheter Valve Studies Show Strong Results in SCAI Late-breakers
Medtronic Shares Two-Year Harmony Transcatheter Pulmonary Valve Results
FDA Expands Indication for Melody Transcatheter Valve for Failed Surgical Valves
TAVR Expected to See Rapid Growth in Next 5 years
VIDEO: The Expansion of TAVR Following the FDA Clearing its Use in All Patients — Interview with Torsten Vahl, M.D.


 May 13, 2026
May 13, 2026 









