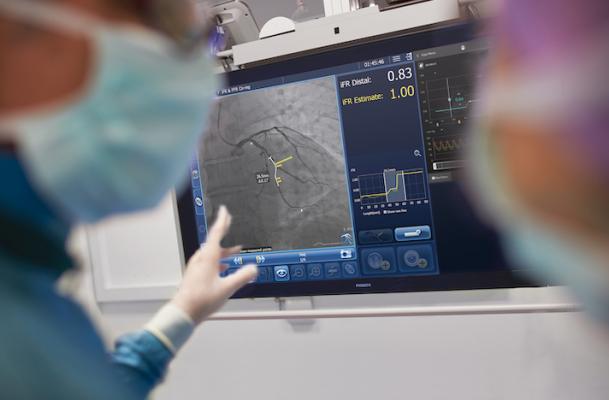
Angiography with a co-registered view of pressure drops according iFR readings in a coronary vessel. The DEFINE PCI study showed patients had improved outcomes and less recurrent chest pain at one year using iFR physiologic measurements combined with landmarks shown on angiographic imaging to better guide therapy. Image by Philips Healthcare
Fractional flow reserve (FFR) is considered the gold standard measure whether a coronary lesions needs a percutaneous coronary intervention (PCI) or if the patient can be treated with medical therapy and avoid a permanent metallic stent implant. There were several FFR late-breaking clinical trials presented at the 2020 Transcatheter Cardiovascular Therapeutics (TCT) meeting in October.
FFR is widely used to guide the revascularization strategy in the catheterization lab. The FAME I and FAME II trials have shown that stable ischemic heart disease lesions with FFR more than 0.80 can be safely treated medically, while PCI of lesions with FFR less than 0.80 may benefit from revascularization. The trials detailed below looked at how to improve this strategy, better optimize PCI and if computed tomography (CT) derived FFR can help reduce overall healthcare costs.
TARGET FFR Failed to Help Reduce Residual Blockages Following PCI
The late-breaking TARGET FFR trial at TCT showed a physiology-guided optimization PCI strategy did not achieve a significant increase in the proportion of patients with final FFR ≥0.90, and it failed to reduced the proportion of patients with a residual FFR ≤0.80 following PCI. This was a surprise to many, who expected the data to show improved outcomes.
“When assessing the proposed optimal post-PCI FFR cutoff value of ≥0.90, we found that the majority of patients with angiographically acceptable PCI results actually have a physiologically suboptimal outcome,” said Damien Collison, M.D., interventional cardiologist at the Golden Jubilee National Hospital, Glasgow, Scotland. “Up to 30% of patients may even have a final FFR result that remains below the guideline-directed threshold for performing revascularization in the first place. In our randomized controlled trial, application of an FFR-guided optimization strategy after stenting led to improvements in both FFR and CFR and significantly reduced the proportion of patients with a final post-PCI FFR ≤0.80.”
The study enrolled 260 patients that were randomized between March 2018 and November 2019 at a single site. Following angiographically successful PCI procedures, patients were randomized (1:1) to receive either a physiology-guided incremental optimization strategy (PIOS intervention group, n=131) or blinded post-PCI coronary physiology measurements (control group, n=129). Patients undergoing successful, standard-of-care PCI for either stable angina or medically stabilized non-ST-segment-elevation myocardial infarction (NSTEMI) were eligible for randomization.
Read more in the article FFR-guided PCI Optimization Strategy May Lead to Improved Outcomes.
iFR Co-registered With Angiography Improved Post-PCI Outcomes
Another trial may offer a solution to better optimize PCI using a variant of FFR technology from Philips Healthcare called instant wave-free ratio (iFR). It co-registers the pressure drops with angiography so physician can identify precise locations causing ischemia, plan stent length and even place a virtual stent to predict physiologic improvement before the intervention.
The late-breaking DEFINE PCI study showed patients had improved outcomes and less recurrent chest pain at one year using iFR physiologic measurements. The one-year data showed an optimal post-PCI iFR of ≥0.95 was associated with improved event-free survival. Patients with a post-PCI iFR of ≥0.95 had 68% fewer clinical events than patients with less than optimal post-PCI iFR values (1.8% vs 5.7%, p=0.04).
Read more details in the article DEFINE PCI Study One-year Data Show Potential of Treating Residual Ischemia to Improve Outcomes for Coronary Stenting.
FFR-CT Not as Cost-effective as Envisioned
Invasive FFR has competition from image-derived FFR assessments. Key among these is computed tomography FFR (FFR-CT) that can evaluate the entire coronary tree FFR values to determine if a patient presenting with chest pain requires PCI and can skip the use of diagnostic catheter angiograms. The U.K. included FFR-CT in its routine clinical proactive under the National Institute for Health and Care Excellence (NICE) guidelines.
The late-breaking FORECAST randomized clinical trial looked to confirm that FFR-CT use would result in a lowering of costs to care for patients in the U.K. National Health System (NHS). However, it did not significantly reduce costs, but it did reduce the use of invasive coronary angiography.
"In patients presenting with new onset stable chest pain, a strategy of CT coronary angiography with FFR-CT, when compared with a strategy of routine care, it did not significantly reduce costs in the NHS system. But, it was associated with a significantly lower rate of invasive angiography," explained Nick Curzen, BM (Hons), Ph.D., chair of interventional cardiology and professor of interventional cardiology, University of Southampton, United Kingdom, who presented the study.
He said it was disappointing because the hope was to show there was a cost saving using a non-invasive method, which patients would prefer.
"The fact is, the invasive coronary angiography rate and the revascularization rate were not reduced enough to take account of the costs for the CCTA and FFR-CT up front. The trial question is if FFR-CT can save money. I think we can reach that point, but not by using it so freely," Curzen said. He said the wide use of the technology may be the issue and if were only used on select patients, the cost saving would likely be more evident.
"In order for a test to lower costs, it is going to have to provided fairly substantial resource offsets, and in this study it simply did not," explained David Cohen, M.D., chair in cardiovascular clinical research at Saint Luke’s Mid America Heart Institute. "The only way FFR-CT is going to lead to cost saving is if it can offset other tests, like avoiding the need for nuclear stress tests."
Read more in the article FFR-CT Did Not Significantly Reduce Costs But Reduced Rates of Invasive Coronary Angiography.
FFR Combined With OCT Improved Outcomes in Diabetics
Data from the COMBINE (OCT-FFR) study found that the use of FFR combined with OCT imaging can help improve the accuracy of high-risk lesion identification in patients with diabetes. The study also suggests that the presence of thin cap fibro-atheroma, even in the absence of an abnormal FFR, was predictive of future events.
While FFR has helped improve identification of ischemic culprit lesions in most patients this is not true in all subgroups. Recent evidence has shown that in some patient subgroups such as diabetes mellitus (DM) and/or acute coronary syndrome (ACS), lesions with FFR of more than 0.80 can have worse outcomes than in patients without DM or ACS, most likely due to plaque instability or rapid progression of atherosclerotic plaque.
Previous studies have shown that lipid-rich plaques with a thin cap fibro-atheroma (TCFA) have unfavorable clinical outcomes compared to non-TCFA lesions particularly in DM patients. Optical coherence tomography (OCT) can accurately identify lipid-rich and TCFA lesions. Whether OCT can identify lesions with future unfavorable clinical events despite lack of ischemia has not been studied previously.
The COMBINE trial was a prospective international, natural history study. Patients with DM and with stable or acute coronary syndromes who had one or more non-culprit target lesion(s), with a 40-80% diameter stenosis, underwent FFR assessment. FFR-negative patients underwent OCT assessment and were further medically treated. Depending on the presence or absence of TCFA, patients were divided in two groups: TCFA negative (group A) and TCFA positive (group B). Patients with target lesions with FFR<0.80 were revascularized (group C).
The primary endpoint was the incidence of target lesion related MACE defined as cardiac death, target vessel myocardial infarction (MI), clinically-driven target lesion revascularization (TLR), or hospitalization due to unstable or progressive angina at 18 months in the medically treated patients with FFR>0.80 and TCFA patients (Group B) compared with medically treated patients with FFR>0.80 and no-TCFA (Group A). The secondary endpoint was the incidence of MACE between patients with FFR>0.80 and TCFA (Group B) vs. revascularized lesions that had FFR<0.80 (Group C).
The primary endpoint occurred in 13.3% of Group B compared with 3.1% of Group A [HR 4.7 95%CI (2-10.9) P=0.0004], suggesting that the presence of TCFA even in the absence of an abnormal FFR was predictive of future events. This rate of adverse events was even higher than the rate of events among the revascularized lesions with abnormal FFR at baseline (Group C) [HR 1.25 95%CI (0.28-5.59) P=0.77].
“In patients with diabetes, COMBINE (OCT-FFR) showed that the presence of a high-risk plaque is a strong predictor of future MACE, despite lack of ischemia,” said Elvin Kedhi, M.D., Ph.D. Kedhi is a professor of cardiology, working in ULB (Liberal University Brussel) Hopital Erasme and Silesian Medical University, Katowice, Poland. “Additionally, patients with high-risk plaques (TCFAs) have a significant increase in target-lesion related MACE and MI compared to patients without TCFA at 18 months. These findings indicate that combining FFR and OCT can improve the accuracy of high-risk lesion and patient identification and should be adopted in practice.”
The Role of Coronary Flow Reserve in the Era of FFR
The DEFINE-FLOW observational late-breaking study of deferred lesions following combined FFR and coronary flow reserve (CFR) assessments found that untreated vessels with abnormal FFR, but intact CFR, do not have non-inferior outcomes compared to those with an FFR greater than 0.8 and a CFR greater than or equal to two when treated medically.
The role for invasive CFR assessment in the current era remains unclear since FFR has become a reference standard guiding decisions for revascularization. While observational data from invasive and noninvasive tools has indicated that lesions with intact CFR do well, few of these studies simultaneously assessed FFR. This study was designed to address the limitations of the current literature.
A total of 455 patients were enrolled from 12 sites in six countries. Of those enrolled, 430 patients (533 lesions) were protocol-treated and followed for two years. Stable coronary lesions underwent simultaneous FFR and CFR measurement in at least duplicate with central core lab review of the tracings. Treatment followed the local measurements according to a uniform protocol whereby only lesions with both FFR ≤0.8 and CFR <2 underwent percutaneous coronary intervention (PCI). All other combinations, including FFR ≤0.8 but intact CFR >2, received initial medical therapy.
“Because the study was observational, it is not clear what the outcomes among FFR+/CFR- lesions would have been had they undergone PCI instead of medical therapy,” said Nils Johnson, M.D., MS, Associate Professor of Medicine and Weatherhead Distinguished Chair of Heart Disease, Division of Cardiology, Department of Medicine and the Weatherhead PET Imaging Center at McGovern Medical School at UT Health (Houston) and Memorial Hermann Hospital – Texas Medical Center. “There were a number of limitations to this study such as few lesions with severe FFR/CFR as well as unblinded subjects and physicians. The limitations coupled with the results makes this a hypothesis-generating study that can help to further understand the role of invasive CFR and how to treat CFR/FFR discordance.”
Read more in the article Deferring PCI in FFR-Abnormal Lesions With Preserved Coronary Flow Reserve Not Associated With Similar Outcomes as Untreated Lesions with Normal FFR.
Related Trends and Late-breaking Studies at TCT 2020:
Top 10 Takeaways on Interventional Technologies at TCT 2020
Links to all TCT 2020 Late-breaking Study Presentations


 May 06, 2026
May 06, 2026 









