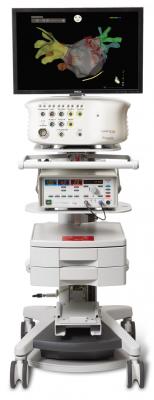
Nationwide data show that although only about 12 percent of X-ray exams are for interventional cardiology or electrophysiology (EP) procedures, nearly 50 percent of a patient’s lifetime radiation exposure comes from the cardiovascular labs. In an effort to reduce this level of patient radiation exposure, Scripps Prebys Cardiovascular Institute, part of Scripps Memorial Hospital and Scripps Green Hospital, evaluated Biosense Webster’s CartoUnivu module for the Carto 3 System (Figure 1) before it was made commercially available earlier this year. Researchers looked for its potential benefits in reducing radiation exposure to patients and clinical staff.
Methods
The CartoUnivu module provides for fixed fluoroscopic images or cines to be transferred to the 3-D electro-anatomic mapping system. The module allows for real-time visualization of intracardiac catheters against a background of a stored fluoroscopic image (Figure 2). Typically, multiple fluoroscopic images (three to eight) are acquired at different angulations and stored. Once transferred, the fluoro image is integrated into the 3-D map view, allowing the user to create an electo-anatomical map on top of the captured fluoroscopic image or looping cine. Not only does this proved fluoroscopic images for reference, our electrophysiologists consistently commented that it diminished the interest in confirming catheter location with additional fluoroscopy.
Researchers performed a retrospective evaluation of the impact of this new technology on radiation usage. We reviewed our first 31 CartoUnivu cases from two EP laboratories and compared the procedure and fluoroscopy times to 96 procedures for six months using traditional mapping and fluoroscopy methods, matched by operator (total of eight). The 137 patients included in the study were referred for either pulmonary vein isolation (PVI) procedures for atrial fibrillation (18 study, 51 controls), cavotricuspid isthmus block for atrial flutter (8 study, 33 controls), supraventricular tachycardia ablation, either atrioventricular nodal reentrant tachycardia (AVNRT) or Wolff–Parkinson–White syndrome (WPW) (six study, 23 controls) or ventricular tachycardia (VT) (three study, six controls). The study was approved by the Scripps Institutional Review Board; all data was de-identified for confidentiality.
Results
Cumulative for all procedures, researchers found that the average procedure duration for the CartoUnivu module assisted studies was 254±31 minutes versus 267±85 for the retrospective control group (p=NS). However, the average fluoroscopy times for the CartoUnivu studies were 22±19 minutes versus 60±27 minutes for the comparison group (p<.0001). The fluoroscopy dosage was 1,453 cGy/cm² for the CartoUnivu module versus 3,593 cGy/cm² in controls (p<.0001). The average reduction in fluoroscopy time was 64 percent and dosage 60 percent with the CartoUnivu approach.
The retrospective comparison has limitations as the new focus on reduced radiation usage impacted physician behavior with the new CartoUnivu module. Nevertheless, once mastered, the learning curve inherent with the new system would suggest an opportunity to further diminish radiation usage. Researchers evaluated the findings by operator and procedure. Every operator (n=8) has lower radiation usage with the CartoUnivu module. The radiation reduction was observed in all ablation procedures, though it was more pronounced in the complex cases (PVI and VT).
Conclusion
In a non-randomized retrospective review, researchers found a statistically significant 64 percent reduction in fluoroscopy times and 60 percent in dosages (p<.0001) for EP ablation procedures utilizing the CartoUnivu module fluoroscopic integration system as compared to traditional fluoroscopy supplemented with similar 3-D mapping. The availability of a fluoroscopic image to be stored and superimposed into the 3-D electro-anatomic mapping system resulted in less need for fluoroscopic confirmation of landmarks and catheter positions. They predict that this CartoUnivu module will reduce physician dependence on fluoroscopic imaging and thus diminish radiation exposure for patients, physicians and staff. If these data are confirmed, patient safety will be positively impacted by this new technology.
Editor’s note: Steven L. Higgins, M.D., FHRS, chairman, department of cardiology, director of electrophysiology, Scripps Memorial Hospital, La Jolla, Calif. He is a paid consultant to Biosense Webster. The Scripps Prebys Cardiovascular Institute combines the expertise of Scripps Memorial Hospital and Scripps Green Hospital, with a skilled team of nearly 100 cardiologists. Scripps was recently designated as No. 20 in the U.S. News Top-Ranked Hospitals for cardiology and heart surgery.