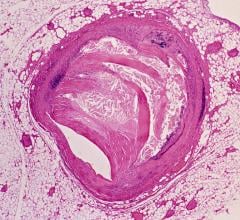
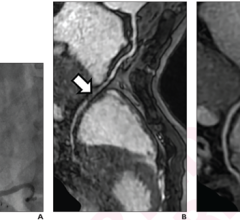
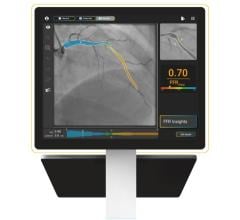
The Medis QFR technology allows non-invasive functional FFR assessment of coronary flow based on standard X-ray angiographic images in the cath lab without the use of a pressure wire.
Fractional flow reserve (FFR) pressure wires have been used now in interventional cardiology procedures for more than a decade to determine the physiological significance of a coronary lesion and decide if a stent is required. But in the past couple years, several new FFR assessment technologies have gained U.S. Food and Drug Administration (FDA) approval, including simplified hyperemia-free technologies and image based FFR assessments.
FFR offers a nonobjective modality to use empirical quantification, rather than the old method of “eyeballing” a lesion on an angiogram to guess at its level of restricting blood flow. Pressure wires inside the blood vessel can measure blood flow across a coronary lesion to determine it is flow limiting and requiring revasculatization, or due to the Venturi effect, if there is adequate flow so the lesion can be treated using medication. However, a big drawback of FFR is the need to use the stressor agent adenosine to induce hyperemia. This is uncomfortable to the patient and adds extra cost and time to procedures.
Philips/Volcano introduced an alternative modality called instantaneous wave ratio (iFR), which is a hyperemia-free physiologic index similar to FFR. Its validation in larger trials has increased its usage in the past couple years because it is easier to use and eliminates adenosine. Competitors in the FFR space have since launched similar hyperemia-free FFR technologies, including Abbott’s Resting Full-Cycle Ratio (RFR) and OpSens’ diastolic pressure algorithm (dPR).
Rather than a standalone console showing a wave form and the FRR ratio, vendors have tried to make the technology more useful and intuitive in the last five years by integrating FFR information with the angiographic imaging used to guide procedures. Philips’ is the most advanced in this area, offering co-registration of the FFR catheter readings with an angiogram to show the precise locations where there is a reduction in coronary pressure due to specific blockages. This makes it easier to see exactly where the culprit lesion is in patients with heavily diseased arteries, or which target lesions to stent so the entire messing is not encased in metal in attempts to stent all lesions. This can help reduce costs by reducing the number of stents and can improve outcomes by targeting which lesions really need to be revascularized.
Three image-based technologies now have FDA clearance to assess FFR without the use of a specialized pressure sensing catheter, again helping simplify procedures and reduce costs. They apply computational fluid dynamics and other algorithms to the image data to assess blood flow through vessels based on computed tomography (CT) or angiographic imaging in the cath lab, using different views, to create a 3-D vessel reconstruction showing color codes for the changes in virtual FFR pressures. CathWorks and Medis both have approval for FFR-angio for use in U.S. catheterization labs. Both systems take a few minutes to process the image data to render the 3-D image analysis.
HeartFlow’s FFR-CT technology has had FDA approval for a few years, but many hospitals wanted to see more validations that a CT scan assessment of a lesion match invasive pressure wire FFR. Numerous studies now show this correlation, and at some centers its use has reduced the number of diagnostic catheterizations. The main issue hospitals have with the technology is that it requires patient data to be transferred electronically to HeartFlow in California so a supercomputer algorithm can be applied. This process can take between 2-5 hours. However, some centers using the technology said it is good for outpatient assessments to determine if elective PCI is needed. In the emergency department, FFR-CT can be used for chest pain patients for faster discharge of non-heart attack patients. They say it can offer results faster than troponin series testing or holding a patient overnight for a nuclear perfusion study or diagnostic cath in the morning.
Next on the FFR technology horizon is the use of intravascular optical coherence tomography (OCT) to predict FFR values and assess if OCT parameters may predict clinical outcome in patients with negative FFR. This was the subject of a late-breaking study at the Society for Cardiovascular Angiography and Interventions (SCAI) 2020 Scientific Sessions Virtual Conference in May.
Related FFR Technology Content:
Image-based FFR May Replace Pressure Wires and Adenosine
New Technologies Take Cardiac CT to the Next Level
OCT May be Able to Show FFR Without Need for Pressurewire
DEFINE GPS Study Assesses PCI Guided by Integrated iFR and Angiography
CathWorks FFRangio System Receives U.S. FDA Clearance
FFR-CT: Is It Radiology or Cardiology?
Medis QAngio XA 3D Receives FDA 510(k) Clearance
Find more news and new technology in the FFR Technology Channel

 October 24, 2025
October 24, 2025