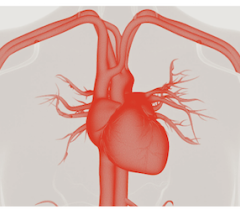
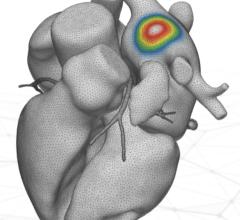
An example from the study of the Biosense Webster NuVision 3D/4D ICE imaging capability showing the left atrial appendage (LAA) visualization on 3D ICE. The system allows the user to place a false lighting source to be placed in different positions to change the lighting and shadows to better visualize the anatomy.
August 5, 2021 — A prospective, non-randomized, multicenter, first-in-human clinical study found good diagnostic and procedural guidance value using a new 3D/4D intracardiac echo (ICE) imaging catheter in radio frequency and cryo-ablation procedures, and left atrial appendage (LAA) occlusion procedures. The study of the new Biosense Webster NuVision ICE catheter was presented at the 2021 Heart Rhythm Society (HRS) meeting.
The catheter effectively guided transeptal puncture in all attempts, and image quality and catheter performance were rated by operators as very good in 82% of patients, explained lead author Vivek Y. Reddy, M.D., director, cardiac arrhythmia service, Icahn School of Medicine at Mount Sinai, New York. Overall, he said the 4D ICE catheter is a safe and effective visualization tool to guide a variety of electrophysiology procedures with multiplanar imaging.
The novel 4D ICE catheter is capable of real-time volumetric imaging with a 90° x 90° field of view, both 2D and 4D Color Doppler flow ability, independent distal tip rotation and penetration depth up to ~15 cm. The catheter was designed to allow multiplanar visualization of target cardiac structures with facile, minimal catheter manipulation.
"Our data support a growing shift in the electrophysiology field toward multiplanar imaging catheters that can offer operators a clearer look at a patient's heart and enhance their field of view when performing life-saving procedures," Reddy explained. "For patients, this technology provides the most comprehensive look at their heart, helping to ensure their physician can provide optimal outcomes."
3D/4D ICE is a New Imaging Technology
For years, 2D ICE has been a standard imaging technology in the electrophysiology (EP) and cath labs, because it enables light sedation compared to full sedation required for use of transesophageal echo (TEE). However, until now it has been limited to only 2-D imaging, while TEE has offered live 3D/4D imaging, so it was easier in understand the anatomy being imaged. This new version of ICE offers live 3D/4D imaging using the Biosense Webster NuVision Ultrasound Catheter that operates using GE Healthcare Vivid Ultra Edition ultrasound systems.
Philips in 2021 also released the new VeriSight Pro ICE catheter, which offers superior 2-D and 3-D live image guidance for EP and structural heart procedures, which recently saw first use in the United States at Mayo Clinic and Northwestern Medicine.
Biosense Webster 4D Ice First-in-Human Study
The study was conducted by 9 operators at 2 European clinical sites. The 10 French catheter was introduced into the right atrium (RA) via femoral vein access, and imaging was performed from the RA, coronary sinus, or directly from within the left atrium, after manipulating the catheter through a transeptal puncture hole dilated with a 12 French sheath (n=2). Primary and secondary safety endpoints were absence of: i) unanticipated AEs or procedure/device related AEs, and ii) all device or procedure-related AEs.
Primary and secondary performance endpoints were ability to provide adequate imaging for procedural completion. Secondary performance endpoint was positive user questionnaire responses of 2D/3D images.
In 28 patients (age 59±15 yrs, 25% F), the 4D ICE catheter was used to guide either LAA closure (n=2: one each - Watchman-FLX and Amulet) or catheter ablation of AF (cryoballoon, n=8; RFA, n=12) or other arrhythmias (PVC / VT / SVT / WPW; n=6). All safety and performance endpoints were met in all patients.
Reddy said the next steps are to gather further data on reproducible image acquisition, safety outcomes, and hospital resource utilization will be collected.
The study researchers included Vivek Y. Reddy, M.D., Icahn School of Medicine at Mount Sinai, New York; Petr Neuzil M.D., Na Homolce Hospital, Prague, Czech Republic; Shephal K. Doshi, M.D., Pacific Heart Institute, Santa Monica, Cailf; Brett Gidney, M.D., Santa Barbara Cottage Hospital, Santa Barbara, Calif.; Andrea Natale, M.D., and Amin Al Ahmad, M.D., St. David’s Medical Center, Austin, Texas; Miguel Valderrabano, M.D., Ph.D., Houston Methodist Medical Center, Houston, Texas; Gediminas Rackauskas, M.D., Ph.D., and Audrius Aidietis, M.D., Ph.D. Centre for Cardiology and Angiology, Department of Cardiovascular Diseases, Vilnius University, Lithuania.
Related Intra-cardiac Echo Content:
Northwestern Medicine First in U.S. to Use Live 3D Intracardiac Echo for EP Procedure
Mayo Clinic First to Use Next Generation 4D ICE System to Guide Structural Heart Procedures
Trends and Advancements in Intra-cardiac Echo Imaging Systems
Intra-Cardiac Echo Aids EP Ablations, Structural Heart Procedures
Intracardiac Echo Should be More Widely Adopted to Minimize Radiation in Catheter Ablations


 April 24, 2026
April 24, 2026