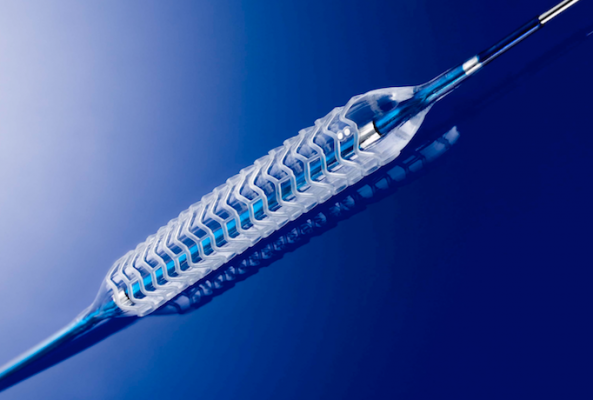
The Abbott Absorb Bioresorbable Vascular Scaffold (BVS).
There was no shortage of interest in bioresorbable stent technologies at the many sessions offered on this topic or based on the number of start-up bioresorbable stent companies presenting at the 2017 Transcatheter Cardiovascular Therapeutics (TCT) meeting. However, there was noticeable apprehension at the meeting about what the future of the technology will be.
Over the past several years at TCT, there has been a focus away from traditional metallic drug-eluting stents (DES) to these bioresorbable scaffold technologies as the next step in stent evolution. However, recent trial data, especially from the ABSORB III Trial, and the first commercial bioresorbable stent being pulled off the market on Sept. 14, 2017, has dampened that view.
The latest round of trial data for the Abbott Absorb everolimus-eluting bioresorbable vascular scaffold (BVS) at TCT shed light on why the company announced last September it was pulling the stent off the market. Data from several ABSORB trials statistically showed good performance compared to the market-leading Xience everolimus-eluting metallic stent. However, there was signal in the data for slightly poorer outcomes, negating any long-term benefits the stent might offer. Experts involved in the trials said Absorb saw a very low usage rate, with estimates of U.S, usage of less than 5 percent.
It was known the Absorb bioresorbable stent had its limitations, but the goal with the new technology was its expected late benefits when the stent dissolves after three years. However, these benefits have not been demonstrated yet in the ABSORB III Trial, while the device carries several disadvantages, including the demonstrated poorer outcomes, said Ajay Kirtane, M.D. SM, director of the cardiac catheterization laboratories at New York-Presbyterian Hospital/Columbia University Medical Center, who has been involved in the ABSORB trials. Earlier clinical data on the stent showed late benefits such as the return of vasomotion to treated vessels, the elimination of a metallic implant to preserve future surgical options, and the elimination of a vessel prosthesis that could cause late stent thrombosis or restenosis.
“The key thing with this technology is that you have a tax to pay (trade-offs in deliverability) that was hopefully going to be offset by a late benefit with these devices,” Kirtane explained. “Unfortunately, when you look at the results of the ABSORB III Trial, although not statistically significant, there is a higher incidence of target lesion failure, and target vessel failure is certainly greater when compared to the Xience stent. And even things like target lesion stent thrombosis and MI [myocardial infarction] are higher with this device. This is not a tax we want to pay, either as physicians or for our patients.”
Kirtane said the safety is always a foremost concern with any new technology and the data has raised concerns.
“The real question is if this device is as safe in the short term, even out to two or three years, as conventional metallic drug-eluting stents. I think that is one of the reasons why operators stopped using this device to a large degree and why ultimately Abbott stopped commercializing the device,” Kirtane said. “Even with better technique (used in the ABSORB IV Trial) it still does appear the stent compares to our current generation of metallic stents. That is why we have seen global utilization as a whole drop.”
 Data from the other ABSORB trials presented at TCT, including an overall analysis, showed the stent is technically challenging to implant, and outcomes differ depending on the experience of the operator and the techniques used to implant the device.
Data from the other ABSORB trials presented at TCT, including an overall analysis, showed the stent is technically challenging to implant, and outcomes differ depending on the experience of the operator and the techniques used to implant the device.
“The hypothesis was that by using the best implantation techniques, we could mitigate these results, but it does not appear to me that if you use the Absorb only in larger vessels you are going to be immune to some of the undesirable effects of the stent,” Kirtane explained. “This stent does not even the playing field. Our current generation stents are so good that even operators that don’t use superb technique can still get good outcomes. Whereas this device, because it is harder to put in, it’s bulkier and other factors, the outcomes are further subject to technique plus the device itself with its thicker struts.”
Despite data showing slightly poorer outcomes with Absorb, Kirtane and other key thought leaders at TCT did not think this spells the end of development for bioresorbable stent technology. They all said it just needs to be further refined into a device that can at least match current metallic stents for ease of implantation and show at least as good as, or better, clinical outcomes.
“The idea [of bioresorbable stents] has promise,” Kirtane said. “If you have a device that goes away over time, then perhaps you can lower late events. That is something that intuitively makes sense and perhaps will be proven. These trials are not dead, we are going to follow these patients for longer and will see what the results are. The challenge though is that you had to study thousands of patients with massive investments with this technology, and then to see it fail, in a sense, this way really puts a damper on the field. But that doesn’t mean we can’t make a better stent that will have thinner struts and potentially will work better.”
Abbott Continues Absorb Development
Abbott said it will continue its research into bioresorbable technologies. Abbott’s Chief Medical Officer Charles Simonton, M.D., FACC, FSCAI, spoke in the FDA townhall meeting at TCT 2017. He said the company is working on a new 99 micron strut bioresorbable stent. The Absorb BVS was 150 microns, which caused delivery issues and problems in small vessels.
“There is definitely a future for this technology,” Simonton said. “The adverse event rates are so low (with modern stent technology) there is not much room for problems early on, even if late-term results might be better. We are going to work on a small strut device and work on reducing target lesion failure in the first year.”
Abbott Restarts Bioresorbable Stent Clinical Trials With New Esprit Below-the-knee Scaffold
Is There Any Risk to Patients With Implanted Absorb Stents?
The trend toward poorer outcomes from the ABSORB III Trial presented at TCT 2017 prompted the U.S. Food and Drug Administration (FDA) to issue a warning letter to healthcare providers on Oct. 31, 2017. The FDA stated the interim three-year study results from the ABSORB III pivotal trial continued to show increased rates of major adverse cardiac events and stent thrombosis in patients receiving the Absorb compared to Xience.
“I don’t think there should be any alarm for patients who already have one of these stents, there are things that can be done, such as an extension of dual-antiplatelet therapy, and even just close medical monitoring,” Kirtane said. “These are not high risks, just marginally increased risks over the current-generation DES.”
ABSORB III Trial Data Raised Concerns
The ABSORB III trial two-year results were presented at the American College of Cardiology (ACC) 2017 meeting and showed mixed results for Absorb, which may have made some clinicians more apprehensive about its use earlier in 2017. The 2,008-patient trial showed Absorb had results comparable to Xience, but had a slightly higher percentage of poor outcomes. This raised concern about Absorb’s slightly higher rates of target lesion failure, poor outcomes in 2.5 mm or smaller vessels, and a few cases of late-stent thrombosis.
“What we presented was really the difference between year one and year two of the study. The event rates were actually quite low in both groups, slightly higher with Absorb,” explained Stephen Ellis, M.D., professor of medicine and director of interventional cardiology at Cleveland Clinic, who presented the ABSORB III data at ACC.17.
With the ABSORB II and ABSORB Japan studies, there were findings of late scaffold thrombosis. Ellis said this was the key safety signal that researchers paid more attention to in the ABSORB III and IV trials. In ABSORB III, Ellis said there were four patients out of 1,300 who received the Absorb stent that had late-stent thrombosis. Ellis said two patients were off of dual-antiplatelet therapy and none of them received what would be considered contemporary implantation technique. He said Absorb can be implanted safely with comparable results to Xience, but it requires special handling, careful patient selection and use of specific techniques only applicable to the Absorb. User experience with the device also plays a role, he said.
Optimal Implantation Technique for Bioresorbable Stents
One of the issues when the Absorb stent was first released into the market was that many operators thought it could be used just like the metallic stents they were used to implanting. Ellis said many of the ABSORB trial operators felt this way too, but it was found different techniques were needed because they do not behave exactly like conventional DES.
“One of the mechanisms by which metallic drug-eluting stents work is that they can actually score the vessel,” Ellis explained. “It’s a little bit like stepping on snow with a cross-country ski as opposed to a snow shoe. But, you cannot embed the Absorb as easily into the vessel wall, and the device is thicker, so it tends to protrude quite a way into the lumen, and that is inherently thrombogenic.”
Ellis said the principle way to get around this issue is vessel wall preparation with aggressive pre-dilatation and high-pressure post-dilatation with a slightly oversized balloon. “Those techniques seem to lead to better results,” Ellis said.
Vessel sizing also is more critical with bioresorbable stents, because they will not overexpand as easily or as well as metallic stents.
Also, the Absorb does not perform well in smaller vessels and cannot as easily be snaked through tortuous vessels like its metallic DES counterparts. Both issues are related to the thick stent struts.
The ABSORB IV trial took many of these lessons into consideration, incorporating what is now considered optimal bioresorbable implantation technique. “I don’t think we will have a good comparison between the Xience and the Absorb when we get the one-year results of the ABSORB IV Trial, which was carried out with fewer small vessels and using better implantation techniques,” Ellis said at ACC last March.
However, while the first 30-day results from ABSORB IV presented at TCT 2017 in October found Absorb to be noninferior to Xience, it was associated with higher rates of target lesion failure and device thrombosis than current metallic DES, even with optimal implantation techniques.
Bioresorbable Stent Dismantling May Lead to Late Thrombosis
Stent strut apposition firmly against the vessel wall has long been viewed as optimal implantation technique. Solid apposition allows the stent to be endothelialized and incorporated into the vessel wall over time. However, the Absorb, being made of a pliable plastic as opposed to metal, means it has limitations on how much it can be expanded before the struts break. It also can recoil after expansion because it is not as rigid as metal. Ellis said this is one of the issues with the Absorb, where good apposition is sometimes difficult to achieve. He said this may lead to what is now termed as dismantling over time, as the degrading bioresorbable stent struts droop into the lumen.
“If the device is not well apposed to the vessel wall, when the vessel wall heals, it does not heal around the device to encompass it, the device is sort of left dangling," Ellis explained. "That’s all well and fine if the device has some level of structural integrity, but when it starts to lose that structural integrity, kind of like a hard noodle going to a wet noodle, it flops into the vessel lumen, which is inherently thrombogenic.”
Ellis said metallic stents do not lose their structural integrity, so this phenomenon has not been observed with previous-generation stents and is specific to bioresorbable scaffolds.
What the Future Holds for Bioresorbable Stents
Ellis said metallic stent trials have traditionally concentrated on the one-year outcomes, but the future of stent technology is turning toward improving long-term outcomes, years after implantation. He said this is where bioresorbable technology still holds a lot of promise. As evidenced by the large number of TCT attendees at bioresorbable sessions and the numerous companies working on developing new bioabsorbable stents, the technology has had a setback but is not being abandoned.
“The Xience stent that we compared Absorb against is a very good second-generation device,” Ellis said. “In about 650 patients in the ABSORB III trial who received a Xience, we saw no stent thrombosis at all, which was a little unexpected.” He said it is normal for patients who receive a Xience and other current-generation metallic DES to have a 2-3 percent event rate after the first year, year after year. “It is hoped by having the device go away it will be better, but we have to prove it,” he concluded.
Related Content on Bioresorbable Stents:
VIDEO: Poor Outcomes for Bioresorbable Stents in Small Coronary Arteries — interview with Gregg Stone, M.D., at ACC 2016
Abbott Will End Sales of Absorb Bioresorbable Stent
VIDEO: What Went Wrong With the Absorb Stent? — interview with Ajay Kirtane, M.D., at TCT 2017
Abbott Restarts Bioresorbable Stent Clinical Trials With New Esprit Below-the-knee Scaffold (2020 article)
VIDEO: Bioresorbable Stent Comparable to Xience at Two Years, With Concerns — interview with Stephen Ellis, M.D., at ACC 2017
Tempering the Bioresorbable Stent Euphoria Following FDA Clearance of the Absorb
VIDEO: Bioresorbable Stent Failure Modes, Technique, Patient Selection and Future Development — a discussion with Juan Granada, M.D.
Bioresorbable Stent Comparable to Xience at Two Year, But With Adverse Trends
VIDEO: Key Bioresorbable Stent Technology Presented at TCT 2015 — an interview with Dean Kereiakes, M.D.
FDA Approves First Totally Bioresorbable Stent
The Future of Stent Development Depends on Bigger Improvements in Outcomes


 May 06, 2026
May 06, 2026 









