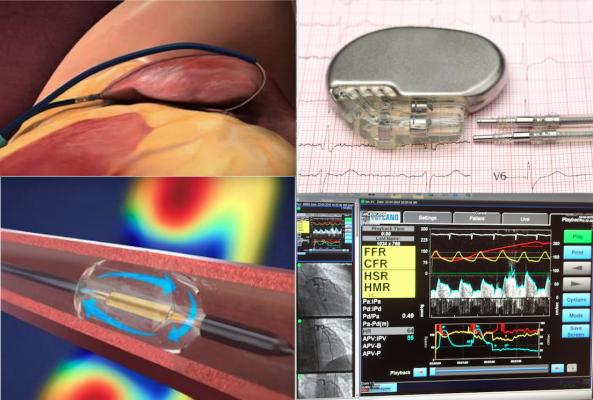
Some of the top technology news from ACC 2021. Top left, the LAAOS III trial showed benefit when surgeons seal off the LAA during other open heart procedures. Bottom left, the ReCor Paradise renal denervation system helped lower blood pressure in patients who did not respond to medication. Top right, for patients with both heart failure and AFib it makes no difference if therapy is focused on controlling the heart rhythm or heart rate. Bottom right, the FLOWER-MI trial found no benefit to FFR-guided PCI in STEMI with multi-vessel disease.
Here are the top 10 takeaways from the late-breaking studies on cardiovascular technologies presented at the 2021 American College of Cardiology (ACC) scientific sessions.
1. Left Atrial Appendage Occlusion Reduces Stroke After Heart Surgery
The LAAOS III trial will likely have the most immediate impact on patient care out of the device trials presented at ACC this year. Some some cardiac surgeons on ACC session discussion panels at the meeting said they planned to suggest on the Monday morning after ACC that all their surgical patients with atrial fibrillation (AFib) undergo left atrial appendage occlusion (LAAO) during open heart procedures.
The study showed surgical closure of the LAA as an add-on procedure during other open heart surgeries lowered the risk of stroke or systemic embolism, the primary endpoint, by 33 percent overall in patients with AFib or atrial flutter. After the first 30 days following the procedure, patients who received LAAO were 42 percent less likely to suffer a stroke over long-term follow-up than those who did not receive LAAO. The trial was stopped early due to the strength of the observed benefits from the procedure.
“This study confirms a new paradigm for stroke prevention for patients with atrial fibrillation,” said Richard Whitlock, M.D., Ph.D., a cardiac surgeon at McMaster University in Ontario, Canada, and the study’s lead author. “The additive benefit of surgical LAAO on top of blood thinners has now been proven. There is no question that patients who are undergoing heart surgery and have elevated stroke risk and atrial fibrillation should have their atrial appendage occluded in their cardiac surgery.”
2. AFib Rhythm Control Versus Rate Control Strategy in Heart Failure Showed No Differences
There is a lot of debate on treatment strategies for patients with both heart failure and AFib. The question is whether to focus treatment on controlling the heart rhythm using catheter ablation, or on controlling the heart rate using drugs and/or a pacemaker. The RAFT-AF study showed no significant differences in terms of death from any cause or progression of heart failure.
The trial is the first of its kind to include patients with AFib and who had heart failure of either reduced ejection fraction (HFrEF) or preserved ejection fraction (HFpEF). However, the trial was stopped early and, as a result, has limited statistical power to reveal differences between the two treatment approaches. But trends observed in the study suggest the type of heart failure a patient has may influence which approach is optimal, researchers said.
it is highly suggestive that ablation-based rhythm control appears to reduce the primary outcome measures, along with secondary outcomes of quality of life and heart failure markers, in patients who have heart failure with reduced ejection fraction,” said Anthony S.L. Tang, M.D., a cardiologist and professor of medicine at Western University in London, Canada, and the study’s lead author. “It’s not quite as conclusive as I’d like it to be, but I think it still is useful to help individual physicians determine treatment strategies. I would be less inclined to use the rhythm control strategy for heart failure with preserved ejection fraction and more likely to use it in people with reduced ejection fraction.”
3. GALACTIC-HF Shows Omecamtiv Mecarbil Brings Greater Benefits for Severe Heart Failure
The experimental heart failure drug omecamtiv mecarbil reduced heart failure hospitalizations by a greater margin among patients with more severely reduced ejection fraction compared with those who had moderately reduced ejection fraction. This was the finding of the GALACTIC-HF trial. Several ACC session panelists felt this trial was one of the most important presented this year at ACC.
Omecamtiv mecarbil works by improving the ability for heart muscle cells to contract and operates through a different biological pathway than any of the current heart failure medications. The research is an extended analysis of data from GALACTIC-HF, a trial involving more than 8,200 participants that found the drug significantly improved outcomes in terms of a composite of cardiovascular death or heart failure events among patients with heart failure with reduced ejection fraction. The new analysis focused on how patient outcomes varied based on the level of severity of their reduced ejection fraction.
“This is a drug that will potentially help the very group of patients that are most difficult to care for,” said John R. Teerlink, M.D., a cardiologist at the University of California, San Francisco and the San Francisco VA Medical Center, and the study’s lead author. “While the results from GALACTIC-HF show omecamtiv mecarbil brought improvements overall, these new findings point to a group of patients with more severe heart failure in whom there is even greater benefit.”
4. No Benefit Found for FFR-guided vs. Angio-guided Multivessel Revascularization In ST-Elevation Myocardial Infarction Patients
There has been debate in interventional cardiology over the need to perform catheter-based fractional flow reserve (FFR) hemodynamic measurements to determine if and where a coronary stent is needed in ST-elevation myocardial infarction (STEMI) heart attack patients. The FLOWER-MI trial looked at the use of FFR vs. angiography image guidance alone for the placement of a second stent in STEMI patients to determine if FFR improves outcomes in these patients.
The data show if a second stent is needed, FFR did not improve outcomes and was more costly than just using angiography. The study found guiding procedures with angiography X-ray imaging alone was more effective.
“The strategy of using FFR to guide the stenting procedure is not superior to the standard technique of using angiography to treat additional partially blocked arteries,” said Etienne Puymirat, M.D., professor of cardiology at the University of Paris, director of intensive care at the Georges Pompidou Hospital in Paris and principal investigator of the study. “In addition to having no benefit, we have also shown that, based on costs in France, the FFR-guided strategy is more expensive.”
5. TAVR Anticoagulation With Apixaban Not Superior to Standard Care
Transcatheter aortic valve replacement (TAVR) carries a risk of adverse events related to bleeding and blood clots, and previous studies have offered conflicting findings regarding the best strategy for preventing these complications. Researchers have also struggled to determine the benefits and risks of antiplatelet or anticoagulation medications in patients who require them for managing heart conditions like atrial fibrillation that are not related to the TAVR procedure compared with patients who would not otherwise need anticoagulants.
The 1,500-patient ATLANTIS trial tried to answer this question and found the anticoagulant apixaban (Eliquis) was not superior to current standard of care following TAVR. While apixaban reduced the formation of thrombosis around the implanted valve with no increased bleeding risk, a subset of patients taking apixaban who did not have an indication for anticoagulation apart from the TAVR procedure showed a tendency toward a higher rate of non-cardiovascular death, a finding researchers said deserves further exploration.
“Our results do not suggest we can routinely use apixaban as the default antithrombotic treatment after successful TAVR,” said Jean-Philippe Collet, M.D., a professor of medicine and interventional cardiologist at Groupe Hospitalier Pitié-Salpêtrière in Paris, France, and the study’s lead author. “Although the safety of apixaban is the same as standard care and it better prevents valve thrombosis, we observed an unexplained signal on non-cardiovascular mortality among patients who do not need oral anticoagulation."
6. Lower Temperature Therapeutic Hypothermia Did Not Improve Outcomes After Cardiac Arrest
Therapeutic hypothermia has been used for years in out-of-hospital cardiac arrest patients to improve survival and reduce brain damage. There has been a question if cooler temperatures were used if it would further improve outcomes in these patients. This ACC late-breaker cooled patients below 31 degrees Celsius (about 88 degrees Fahrenheit) for 24 hours, but it showed no difference in terms of death or poor neurological outcomes at six months compared with patients receiving guideline-recommended cooling of 34 C (about 93 F).
“The results of our trial do not support the use of moderate therapeutic hypothermia of 31 C to improve neurological outcomes in comatose survivors of out-of-hospital cardiac arrest,” said Michel R. Le May, M.D., interventional cardiologist at the University of Ottawa Heart Institute and the study’s lead author. “These findings do not support changing the current guidelines; we need to look for other strategies that can improve outcomes for these patients who currently have a poor prognosis.”
7. Renal Denervation Lowers Blood Pressure in Medication-resistant Hypertension
The RADIANCE-HTN TRIO trial tested the efficacy of the ReCor Paradise renal denervation (RDN) system in patients with high blood pressure who did not respond to treatment with multiple medications. The therapy had a greater reduction in daytime systolic blood pressure than patients who did not receive RDN, with no difference in major adverse effects.
“This study has shown for the first time that RDN can effectively lower blood pressure in patients in whom it is uncontrolled despite standardized treatment with three guideline-recommended medications,” said Ajay Kirtane, M.D., professor of medicine at Columbia University Vagelos College of Physicians and Surgeons and an interventional cardiologist at New York-Presbyterian/Columbia University Irving Medical Center, and co-principal investigator. “RDN offers an additional tool that we could use to help these patients, hopefully achieving better overall control of hypertension, especially if longer-term data support the durability and safety of the procedure.”
Patients in this trial who received ultrasound ablation RDN saw a median reduction of 8 mmHg in their daytime ambulatory systolic blood pressure compared with their level prior to treatment. They also had a 4.5 mmHg greater drop in median blood pressure compared with those who received the sham procedure, despite both groups receiving the same three guideline-recommended antihypertensive medications as background therapy. The benefit of RDN was consistent regardless of sex, ethnicity, age, waist size or blood pressure level at study entry.
8. AI Derived Cardiac Echo Measurements Able to Predict COVID-19 Mortality
Artificial intelligence (AI) derived heart measurements were able to predict COVID-19 mortality on echocardiograms in the Echocardiographic Correlates of in-hospital Death in Patients with Acute COVID-19 Infection: The World Alliance Societies of Echocardiography (WASE-COVID) Study of COVID-19 patients. This international effort was supported in partnership by the American Society of Echocardiography (ASE), MedStar Health, University of Chicago and AI-vendor Ultromics.
"Our original WASE Study first set out to see the state of healthy normal hearts across the world. It took us a few years to manually review all of that data," said Federico Asch, M.D., director of the cardiovascular and echo core labs at MedStar Health Research Institute. "When the pandemic began, we knew that the clinical urgency to learn as much as possible about the cardiovascular connection to COVID-19 was incredibly high, and that we had to find a better way of securely and consistently reviewing all of this information in a timely manner."
"Knowing we had to move quickly to figure out if there was anything about heart health that we could associate with COVID-19 outcomes, we were motivated to secure an industry partner to help accelerate our analysis timeline," explained Roberto Lang, M.D., director of the University of Chicago's noninvasive cardiac imaging laboratory. "Using Ultromics' software to anonymize echocardiograms, upload them to a cloud platform, and use artificial intelligence to quickly and accurately analyze each exam was hugely beneficial in bringing this report forward while the world is still fighting this virus."
Compared to previous studies that have identified coronary artery disease, hypertension and diabetes as cardiovascular comorbidities, this study validated those findings and identified which cardiac measurements and biomarkers were the best predictor of adverse outcomes.
9. NCDR LAAO Registry Shows Left Atrial Appendage Occlusion Associated With Low Rate of Stroke
Real-world data from more than 36,000 procedures recorded in the ACC’s National Cardiovascular Data Registry (NCDR) LAAO Registry, a registry that includes almost all LAAO procedures performed in the U.S., showed transcatheter LAA occlusion with Boston Scientific Watchman device was associated with a low rate of stroke at one year. This benefit was even seen among older patients with atrial fibrillation who faced a high risk for stroke or bleeding.
This study found that in practice, the rate of ischemic stroke (the study’s primary endpoint) was generally on par with rates seen in clinical trials leading to the device’s FDA approval. The findings offer reassurance that LAAO with the Watchman device is likely effective for the patient population currently receiving it, according to the researchers.
“Based on these data, it seems like we’re doing the right thing,” said Matthew J. Price, M.D., director of the cardiac catheterization laboratory at Scripps Clinic in La Jolla, California, and the study’s lead author. “The rate of ischemic stroke was low and supports the clinical effectiveness of transcatheter LAAO as it is currently applied in the U.S.”
10. SAFE-PAD Study Shows No Safety Issues With Paclitaxel-coated Devices in Peripheral Artery Disease
A couple years ago a meta-analyses of small trials showed a mortality safety signal in patients who underwent peripheral artery disease (PAD) revascularization with paclitaxel drug-coated devices. This immediately raised alarm with the U.S. Food and Drug Administration (FDA) and the interventional community, and prompted numerous studies to confirm if there was a mortality signal, or if the findings were just coincidence. The latest study is SAFE-PAD, which showed drug-coated devices are noninferior to non-drug-coated devices for all-cause mortality in Medicare beneficiaries who had femoropopliteal revascularization.
This study adds to the growing list of those showing there does not appear to any issue with increased mortality associated with paclitaxel drug-coated devices.
The initial report from the SAFE-PAD study examined the records of 168,553 Medicare fee-for-service beneficiaries. Results showed that after weighting, cumulative all-cause mortality over the median 2.72 years of follow-up (longest, 5.16 years) was 53.8% with drug-coated devices and 55.1% with non-drug-coated devices (hazard ratio, 0.95; 95% confidence interval, 0.94-0.97; noninferiority p<0.001).
Eric A. Secemsky, M.D., MSc, FACC, et al., designed this retrospective cohort study with feedback from the FDA to provide a longitudinal assessment of the safety of the drug-coated devices in this setting. Secemsky said SAFE-PAD will continue until the median follow-up of all patients surpasses 5 years and the data will provide the FDA a mechanism for the ongoing safety evaluation of these devices.
COVID Has Doubled Rate of Clinician Burnout
Another late-breaking study presentation that was not technology related, but has had a large impact of cardiology this past year, was a an ACC survey that shows the burnout rate among cardiology clinicians doubled in the past year due to the pandemic.
Among those surveyed, burnout increased from 20 to 38 percent during the peak of the pandemic. Rates of burnout pre- and peak COVID-19 pandemic increased across all members of the cardiology care team and was particularly striking among cardiovascular team members, which researchers said may be because they were more likely at the bedside as patients were dying. Among all cardiovascular clinicians – cardiologists, physician assistants, nurse practitioners, nurses, pharmacists and imaging technologists – half provided direct care to patients with COVID-19, and yet one of five reported not having adequate personal protective equipment (PPE). Not surprisingly, the rate of burnout was higher in this group.
For some, COVID-19 is the key influencer for these decisions, with 17 percent of clinicians planning to reduce their clinical work hours, 12 percent planning to leave their current practice and 11 percent planning to retire due to COVID-19.
The survey also revealed financial stressors exacerbated by the COVID-19 pandemic, with 41 percent of respondents reporting that their salary had been reduced to some degree.
Find links to all the ACC 2021 Late Breaking Cardiology Study Results.
SCAI 2021 Interventional Cardiology Late-breaking Clinical Study Results


 April 02, 2026
April 02, 2026 









