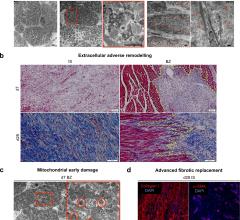
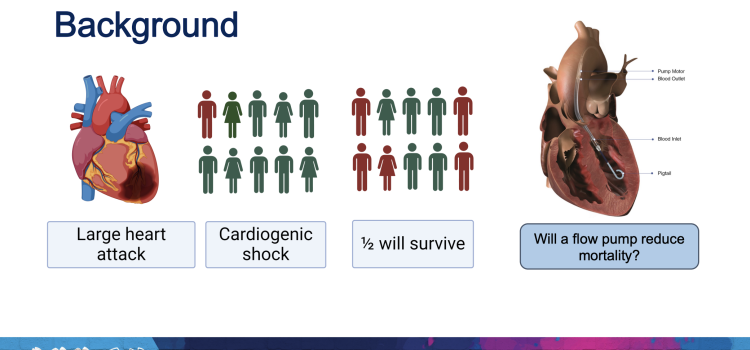
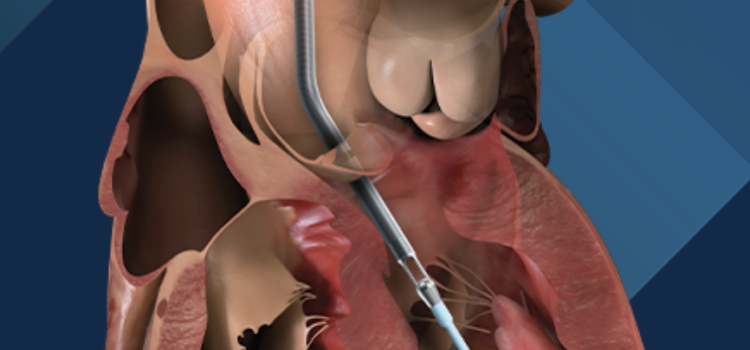
April 8, 2024 — Implantation of the Impella CP micro-axial flow pump in the hours after a heart attack significantly increased the rate of survival at six months among people suffering cardiogenic ...
STEMI
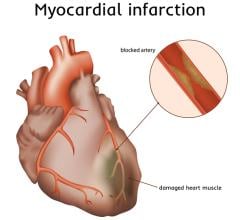
Acute ST-segment elevation myocardial infarction (STEMI) is the one of the most dangerous types of heart attack where there is a serious blockage in one of the major coronary arteries in the heart. The "ST" reference identifies the section of electrocardiogram (ECG) (between the S and T segments on the ECG waveform readout) where there is an abnormality shown as an elevated waveform on the 12-lead ECG.
Minimally invasive, cath lab-based primary percutaneous coronary intervention (PCI) is the preferred treatment for STEMI. This includes use of balloon angioplasty and coornary stent placement to prop open the artery. Centers without a cath lab will usually start an an IV bag with thrombolytic agents to begin dissolving the clot causing the heart attack. This includes use of aspirin and heparin, and in some cases, antiplatelet agents such as ticagrelor. This is usually followed by transport of the patient to the closest hospital with a cath lab.
The conventional standard of care works on the idea that the longer it takes to reopen a STEMI lesion to restore blood flow to the heart muscle, the more damage will likely occur. Lack of oxygen can cause an infarct, where part of the heart muscle dies. This can lead later to heart failure. There is a direct relationship between the length of time a coronary artery is blocked, the amount of permanent damage to the heart, and odds of survival or full recovery.
This has led to the term “time is muscle” and great emphasis has been placed on reducing door-to-balloon (D2B) times at hospitals with cath labs. D2B refers to the amount of time it takes between the patient coming through the door of the hospital to the time an angioplasty balloon can be used to reopen the artery. The national standard is to achieve D2B times of 90 minutes or less. Some centers count D2B time from the arrival of emergency medical services (EMS) by the patient's side to angioplasty.
Hospitals that work to reduce door-to-balloon times are often most successful if they create a STEMI alert system. This requires close coordination between EMS, the hospital emergency department (ED, or emergency room, ER), cath lab staff and the interventional cardiologists. When paramedics detect a suspected STEMI patient with their defibrillator-monitors, a call is immediately made to the ED to start a STEMI alert, or STEMI code. The ED doctor who received the pre-hospital ECG confirms the STEMI, and sends it on to the interventional cardiologist on call for further validation. During daytime hours the cath lab staff prepare a room for the patient, or after-hours are called in to prep the cath lab. The heart team meets the patient at the ambulance dock and transports them directly to the cath lab to save time.
Links to more STEMI Information:
Why STEMI Heart Attacks are so Deadly
ECG in STEMI - Importance and Challenges
Acute Myocardial Infarction ST Elevation (STEMI)
April 8, 2024 — Implantation of the Impella CP micro-axial flow pump in the hours after a heart attack significantly ...
February 27, 2023 — CÚRAM SFI Research Centre for Medical Devices researchers have published in Nature Communications a ...
December 22, 2022 — Johnson & Johnson today announced it has completed its acquisition of Abiomed, Inc. Abiomed is now ...
December 15, 2022 — Doctors from the Emory Heart & Vascular Center are joining forces with the Family Heart Foundation ...
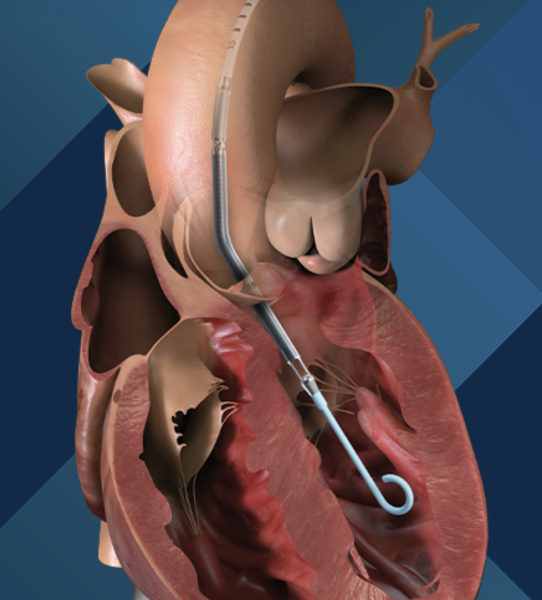
November 1, 2022 — Johnson & Johnson and Abiomed, a world leader in breakthrough heart, lung and kidney support ...
September 13, 2022 — ZOLL Medical Corporation, an Asahi Kasei company that manufactures medical devices and related ...
July 1, 2022 — Despite overall improvements to care for a heart attack, women are less likely to receive timely ...
June 23, 2022 — Despite overall improvements to care for a heart attack, women are less likely to receive timely ...
June 1, 2022 — Recardio's Phase 2 trial results demonstrated the excellent safety profile of its lead drug Dutogliptin ...
May 23, 2022 — New findings from the Ascension Health System’s internal National Cardiovascular Data Registry (NCDR) ...
May 20, 2022 — Results from a retrospective analysis reveal significantly higher mortality rates for low-income ...
May 19, 2022 — The latest analysis from The North American COVID-19 STEMI (NACMI) was presented today as late-breaking ...
May 10, 2022 — Faraday Pharmaceuticals, Inc., today announced the enrollment of the first patient in its Iocyte AMI-3 st ...
April 12, 2022 – The Minneapolis Heart Institute Foundation (MHIF) has announced the first presentation and simultaneous ...
April 7, 2022 – The American College of Cardiology’s Global Heart Attack Treatment Initiative (GHATI) reports continuing ...



 April 08, 2024
April 08, 2024