January 5, 2009 - The University of California, San Diego Medical Center is the first hospital in California to enroll patients in a multi-center clinical trial, sponsored by Angioblast Systems Inc., to examine the safety and feasibility of administering adult stems cells to treat congestive heart failure.
The cells, derived from bone marrow, are injected by a catheter directly into the heart muscle. Sixty patients will be recruited for this clinical trial through UC San Diego Medical Center and hospitals nationwide.
The University of California, San Diego Medical Center is the first hospital in California to enroll patients in a multi-center clinical trial, sponsored by Angioblast Systems Inc., to examine the safety and feasibility of administering adult stems cells to treat congestive heart failure. The cells, derived from bone marrow, are injected by a catheter directly into the heart muscle. Sixty patients will be recruited for this clinical trial through UC San Diego Medical Center and hospitals nationwide.
“This Phase 2 clinical trial will evaluate whether or not adult stems cells can be targeted to the heart muscle to repair and help improve cardiac function in patients with severe heart disease,” said Anthony DeMaria, M.D., director of the Sulpizio Family Cardiovascular Center at UC San Diego Medical Center. “The hope is to identify an effective, minimally-invasive treatment for the growing numbers of patients in the U.S. who suffer from advanced heart failure and have no other treatment alternatives.”
Heart failure, which affects more than five million patients in the U.S., is a condition in which the heart progressively loses its ability to pump blood throughout the body. Heart failure patients often have a history of prior heart attack and underlying disorders such as narrowing and hardening of the arteries, high blood pressure, and arrhythmia or irregular heartbeat.
The stem cells used in this clinical trial are derived from the bone marrow of an adult donor. Angioblast Systems Inc. of New York has identified a population of stem cells which may stimulate the regrowth of a patient’s own heart muscle cells and blood vessels. This cell type is selected and prepared from a universal donor, expanded into large numbers, and injected into a recipient. The cells can be used in unrelated recipients because they do not activate the immune system.
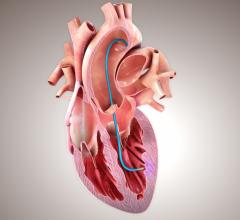
Before the cells are injected into the patient’s heart, a three-dimensional color-coded map is made of the heart’s left ventricle, where the pumping action takes place. Using a technology called the NOGA XP Cardiac Navigation System, a visual is created which identifies the electric signals of the heart. By assessing the living and scarred areas, physicians can identify diseased tissue and then guide the injection catheter with pinpoint accuracy to the desired location.
Upon completion of the map, the patient undergoes a one-hour procedure in which a long catheter, a thin tube, is threaded through the femoral artery in the leg and then up into the heart. This procedure, performed by Nabil Dib, M.D., associate professor and co-investigator of the trial, uses a series of tiny needle injections to deliver millions of cells to the areas of the heart surrounding the scar tissue.
“The concept is that the adult stem cells will either directly or indirectly rebuild the patient’s blood vessels and damaged heart muscle,” said Dr. DeMaria, principal investigator of the trial. “What we would like to see in six months is that the heart will have more exertional capacity, and increased contractility, and blood flow. Only through testing will we know for certain.”
This is a randomized, placebo-controlled clinical trial. Three out of four patients in the trial will receive the adult stem cells in different doses. Patients who are eligible for the trial must have symptoms of heart failure, such as shortness of breath, and be ineligible for any other form of medical or surgical therapy.
All patients are followed for a period of one year following the procedure. Exercise tests, echocardiograms, and blood tests will be performed periodically to evaluate changes in the heart’s function. At the conclusion of a three-year period, patients will be informed as to whether or not they received the stem cell treatment.
Ron Ferstadt, 71, of Los Angeles is one of the first patients to enroll in the clinical trial. After suffering four heart attacks, he is looking to new frontiers in science to offer a possible improvement in his heart’s function.
“I waited two years to participate in a study like this one. It’s worth a try,” said Ferstadt, a retired machinist and former competitive ballroom dancer. “The world of medicine will change dramatically in the next decade. I may or may not see it, but it is studies like this that will help offer new treatments.”
For more information: http://health.ucsd.edu/specialties/heart


 November 19, 2021
November 19, 2021