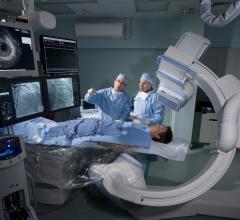
A MitraClip case underway at the University of Colorado Hospital hybrid cath lab. Left to right are doctors John Carroll, Edward Gill and Dominik Wiktor. (Photos by Dave Fornell)
 I recently had the opportunity to conduct an onsite visit to the University of Colorado Hospital Heart and Vascular Center at the Anschutz Medical Campus in Aurora, Colo., which is part of UCHealth. The DAIC team spent two days there to shoot 11 video interviews and sit in on MitraClip and chronic total occlusion (CTO) cases. This is part of a new format DAIC is using to highlight luminary cardiology programs. We wanted to go beyond a single article to instead spotlight the numerous elements that make up a top-notch cardiac center.
I recently had the opportunity to conduct an onsite visit to the University of Colorado Hospital Heart and Vascular Center at the Anschutz Medical Campus in Aurora, Colo., which is part of UCHealth. The DAIC team spent two days there to shoot 11 video interviews and sit in on MitraClip and chronic total occlusion (CTO) cases. This is part of a new format DAIC is using to highlight luminary cardiology programs. We wanted to go beyond a single article to instead spotlight the numerous elements that make up a top-notch cardiac center.
The center performs about 3,000 interventional and structural heart cases per year. Of these, 400 are coronary procedures and 75 percent of those are for acute coronary syndromes. The difficult percutanenous coronary interventions (PCI) performed include complex high-risk and indicated patients (CHIP), including about 50 cases that require Impella support and 25-50 CTO procedures per year. All the physicians who care for patients at this center are also faculty with the University of Colorado (UC) School of Medicine’s Division of Cardiology. Through their CU faculty positions, these physicians have researched and developed the clinical trials and innovative technologies being used today.
 I spoke with John Messenger, M.D., FACC, FSCAI, director of the cardiac cath labs and director of the cardiovascular ICU/stepdown unit, and Kevin Rogers, M.D., director of vascular medicine at the University of Colorado Hospital, about their complex PCI program. They explained how they minimize X-ray and contrast dose during these longer procedures, the tools they use and offered advice for centers expanding into complex PCI. You can watch the interview in the VIDEO: The Evolution of Complex PCI at University of Colorado.
I spoke with John Messenger, M.D., FACC, FSCAI, director of the cardiac cath labs and director of the cardiovascular ICU/stepdown unit, and Kevin Rogers, M.D., director of vascular medicine at the University of Colorado Hospital, about their complex PCI program. They explained how they minimize X-ray and contrast dose during these longer procedures, the tools they use and offered advice for centers expanding into complex PCI. You can watch the interview in the VIDEO: The Evolution of Complex PCI at University of Colorado.
Here is a 360 degree photo of Messenger and Rogers working together during a CTO procedure.
 UCHealth also has a robust structural heart program that has been involved in several key pivotal trials for new technologies. I spoke with John Carroll, M.D., FACC, FSCAI, director of interventional cardiology, and Robert Quaife, M.D., director of advanced cardiac imaging, and James Chen, Ph.D., director of the 3-D imaging lab in the indepth interview VIDEO: Overview of University of Colorado Structural Heart Program about how they developed their transcatheter aortic valve replacement (TAVR) and mitral valve repair programs.
UCHealth also has a robust structural heart program that has been involved in several key pivotal trials for new technologies. I spoke with John Carroll, M.D., FACC, FSCAI, director of interventional cardiology, and Robert Quaife, M.D., director of advanced cardiac imaging, and James Chen, Ph.D., director of the 3-D imaging lab in the indepth interview VIDEO: Overview of University of Colorado Structural Heart Program about how they developed their transcatheter aortic valve replacement (TAVR) and mitral valve repair programs.
You can hear what they had to say on the formation of their MitraClip program in the VIDEO: Evolution of Transcatheter Mitral Valve Repair at the University of Colorado. This includes footage from one of their MitraClip procedures.
 Carroll offered advice to hospitals planning to start a structural heart program based on his own experience in this VIDEO.
Carroll offered advice to hospitals planning to start a structural heart program based on his own experience in this VIDEO.
Beyond his own program, Carroll also has been involved in the Society of Thoracic Surgeons and American College of Cardiology Transcatheter Valve Therapy (STS/ACC TVT) Registry. He offered a good history and overview of the TCT registry, explaining how it is being used to accelerate advancement of transcatheter valve repair and replacement technology in the VIDEO: Tracking Transcatheter Valve Outcomes in the STS-ACC TVT Registry.
 The key to successful structural heart programs is the creation of a close-knit heart team. One of those members at UCHealth is heart failure specialist Andreas Brieke, M.D., director of mechanical circulatory support. He served as the site principal investigator for the COAPT Trial and we spoke about the impact of that study's use of MitraClip in the VIDEO: Impact of the COAPT Trial on Heart Failure Patients With Functional Mitral Regurgitation.
The key to successful structural heart programs is the creation of a close-knit heart team. One of those members at UCHealth is heart failure specialist Andreas Brieke, M.D., director of mechanical circulatory support. He served as the site principal investigator for the COAPT Trial and we spoke about the impact of that study's use of MitraClip in the VIDEO: Impact of the COAPT Trial on Heart Failure Patients With Functional Mitral Regurgitation.
Carroll was the principal investigator for the RESPECT Trial, which helped clear the way for U.S. Food and Drug Administration (FDA) clearance of the Amplatzer device for transcatheter closure of patent foramen ovale (PFO) in patients with cryptogenic stroke. UCHeath's Stroke and Brain Aneurysm Center is where cryptogenic stroke patients are referred and assessed to see if they are candidates for PFO closure. Carrol collaborates closely with neurologist Karen Orjuela, M.D., assistant professor of neurology at the University of Colorado, as part of the heart-brain team. Hear her insights about this team approach in the VIDEO: An Overview of PFO Closure to Treat Cryptogenic Stroke.
 Imaging plays a key role in complex PCI and structural heart procedures. When Carroll started to develop the structural heart program in the 1990s, he brought in Quaife to become director of advanced imaging and James Chen, Ph.D., to become director of the newly created 3-D Imaging Lab. They helped create imaging techniques to enable several structural heart procedures, including working with Philips Healthcare to develop the EchoNavigator technology that allows fusion of both live fluoro with live transesophageal echo (TEE). The EchoNavigator technology is a foundation in all the structural heart procedures performed at UCHealth. Quaife shared his insights on the need for and development of advanced imaging with a step-by-step presentation in the VIDEO: The Role of Advanced Imaging in Structural Heart Interventions.
Imaging plays a key role in complex PCI and structural heart procedures. When Carroll started to develop the structural heart program in the 1990s, he brought in Quaife to become director of advanced imaging and James Chen, Ph.D., to become director of the newly created 3-D Imaging Lab. They helped create imaging techniques to enable several structural heart procedures, including working with Philips Healthcare to develop the EchoNavigator technology that allows fusion of both live fluoro with live transesophageal echo (TEE). The EchoNavigator technology is a foundation in all the structural heart procedures performed at UCHealth. Quaife shared his insights on the need for and development of advanced imaging with a step-by-step presentation in the VIDEO: The Role of Advanced Imaging in Structural Heart Interventions.
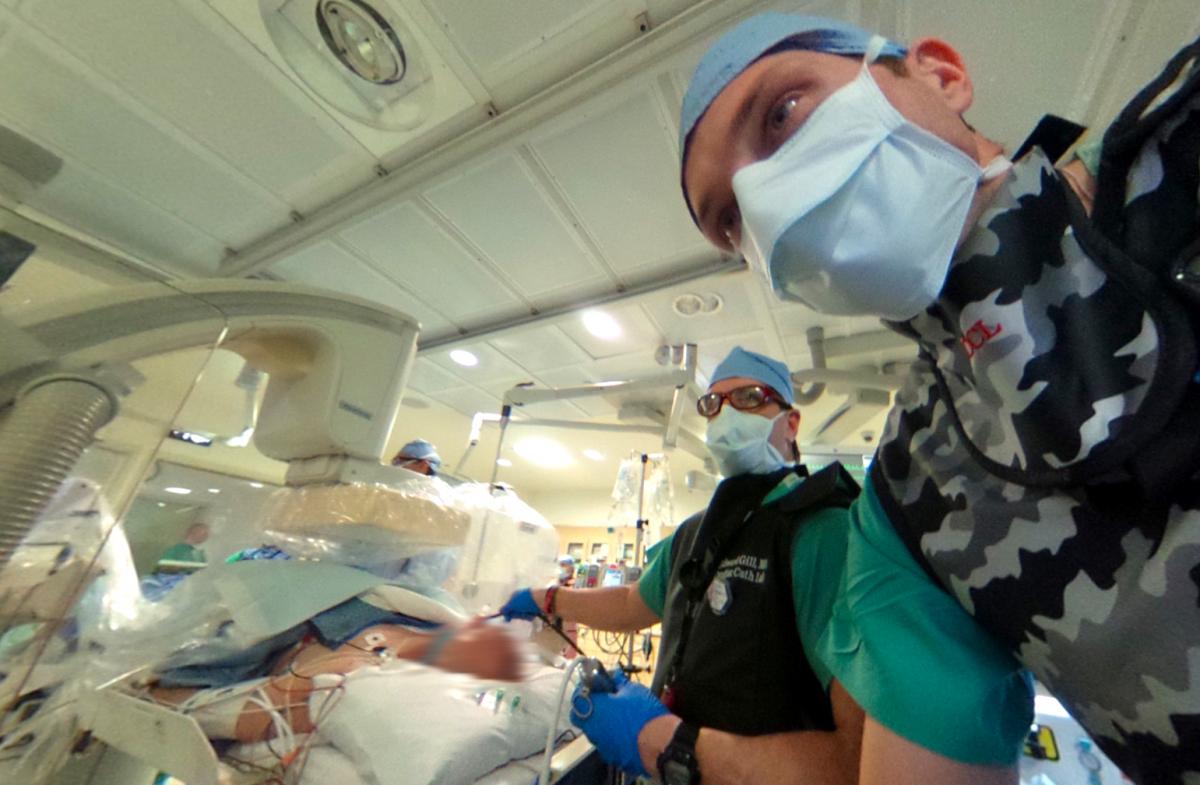 The University of Colorado Hospital 3-D Lab has developed several advanced imaging technologies on its own, but has partnered with Philips Healthcare very closely to commercialize some of these. We spoke to Alexander Haak, Ph.D., clinical scientist at Philips Healthcare, who is permanently based at the hospital. He explains the close, in-the-cath-lab collaboration between the University of Colorado and Philips in the VIDEO: Developing New Cath Lab Technologies With Real-time Collaboration Between Industry, Doctors.
The University of Colorado Hospital 3-D Lab has developed several advanced imaging technologies on its own, but has partnered with Philips Healthcare very closely to commercialize some of these. We spoke to Alexander Haak, Ph.D., clinical scientist at Philips Healthcare, who is permanently based at the hospital. He explains the close, in-the-cath-lab collaboration between the University of Colorado and Philips in the VIDEO: Developing New Cath Lab Technologies With Real-time Collaboration Between Industry, Doctors.
Here is a 360 degree photo showing the echo team in the cath lab during a MitraClip procedure. Haak is seen in the gray camouflaged lead working with the cath lab staff, including Edward Gill, M.D., who is performing the TEE, on how to control novel display features for a new version of the EchoNavigator being tested at the University of Colorado.
 Another thought leader we spoke to was Frederick Masoudi, M.D., FACC, FAHA, professor of cardiology at the University of Colorado Hospital, and a physician leader of the National Cardiovascular Data Registry (NCDR). The NCDR is the American College of Cardiology's suite of cardiovascular data registries helping hospitals and private practices measure and improve the quality of care they provide. He spoke on the value of the NCDR in the VIDEO: The Role of the NCDR in Boosting Cardiology Quality Improvement.
Another thought leader we spoke to was Frederick Masoudi, M.D., FACC, FAHA, professor of cardiology at the University of Colorado Hospital, and a physician leader of the National Cardiovascular Data Registry (NCDR). The NCDR is the American College of Cardiology's suite of cardiovascular data registries helping hospitals and private practices measure and improve the quality of care they provide. He spoke on the value of the NCDR in the VIDEO: The Role of the NCDR in Boosting Cardiology Quality Improvement.
Videos and articles created from this visit will be loaded as they are completed to DAIC's website on a dedicated University of Colorado Hospital landing page.
Take a Virtual Tour of the Cath and EP Labs
Part of the site visit were tours of their newest cath lab, hybrid OR and an electrophysiology lab. You can watch a walkthrough video of these three rooms in:
• VIDEO: Cath Lab Walk Through at the University of Colorado Hospital
• VIDEO: Walk Through of a Hybrid Cath Lab
• VIDEO: Walk Through of an EP Lab at the University of Colorado Hospital
Other Hospital Landing Pages
In 2018, DAIC conducted five on-site hospital visits. Here are the landing pages for some of these:
• Baylor Scott and White Heart Hospital
• Northwestern Medicine — Central DuPage Hospital
(Editor's note: this article was originally published in May 2019 and was revised on Oct. 2, 2019)


 October 24, 2025
October 24, 2025