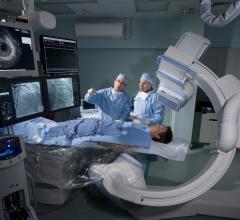
An example of a real-time patient radiation dose tracking system available for Canon's angiography imaging system. Systems like this can show cumulative dose to the patient's skin as a reminder to rotate the C-arm to new positions to prevent burns during long procedures. These types of systems also can help track patient dose and the location of that dose to be included as part of their electronic patient record. This data also enables quality assurance assessments.
A new consensus document on how to mitigate radiation exposure in cardiac imaging for both patients and staff was issued in May, and it advocates for greater use of radiation dose monitoring technologies.[1] The "2018 ACC/HRS/NASCI/SCAI/SNMMI/SCCT Expert Consensus Document on Optimal Use of Ionizing Radiation in Cardiovascular Imaging: Best Practices for Safety and Effectiveness" was issued jointly by the American College of Cardiology (ACC), Heart Rhythm Society (HRS), North American Society for Cardiovascular Imaging (NASCI), Society for Cardiovascular Angiography and Interventions (SCAI), Society of Nuclear Medicine and Molecular Imaging (SNMMI) and the Society of Cardiovascular Computed Tomography (SCCT). It includes input from experts from a total of nine cardiology societies and includes best practices for safety and effectiveness when using computed tomography (CT), nuclear imaging and angiographic/fluoroscopic imaging.
Here are some of the radiation dose monitoring highlights from the 40,000-word document.
Radiation Dose Monitoring and Tracking
The consensus document points out that technology exists to measure and track cumulative radiation dose for both patients and staff. "The importance of tracking the accumulated radiation dose of occupationally exposed healthcare workers is indisputable, as it is important for their protection and can indicate a need for corrective action when necessary," the authors stated.
However, they also noted patient medical exposure dose tracking is more complex and nuanced compared with occupational dose tracking. This is in part because of uncertainty surrounding the actual health impact of current medical radiation practices [3,4].
Current imaging systems and electronic medical records (EMRs) make patient dose monitoring and recording feasible. However, most states do not require radiation dose recording, so many hospitals do not even record basic dose information, turning this feature off on the scanners because it clutters the DICOM headers on the images. There are also many technical issues integrating information from older imaging and data reporting systems. Also, patients often have imaging performed at several locations that might not share the same patient record, so the dose record can be very fragmented or disconnected between providers.
To overcome these issues, the consensus document advocates for use of patient-level tracking technologies, such as an electronic “smart card” that would be updated following each medical exposure.[5] The American College of Radiology (ACR) and other societies developed the Image Wisely educational campaign. That program offers a medical imaging history card that patients can use to track an estimate of their personal accumulated radiation exposure.[6,7] However, it is questionable as to how many patients are this savvy about radiation dose recording.
Required Patient Radiation Exposure Monitoring
The authors of the consensus document note, at a national level, it is not routine practice to monitor and record doses received during each CT scan. However, they said trends are emerging in a few states toward more rigorous regulation. Since 2012, California has required that either volume CT dose index (CTDIvol) or dose length product (DLP), as displayed on the scanner console, be included in every radiology report.[7] The Joint Commission’s new diagnostic imaging standards from 2016 also required documentation of CT dose in a retrievable format for every patient examination.[8]
In order for cumulative radiation dose data to be meaningful, the consensus document authors state it must be compiled rigorously and completely. This should include:
1. Record radiation exposure from all medical tests and procedures involving radiation. This requires that radiation exposure metrics be included in all test and procedure reports in a standardized manner using discrete, uniform parameters that allow for the calculation of cumulative radiation exposure.
2. Compile standardized exposure data from all radiation-based modality procedures automatically in management systems and electronic medical records/electronic health records.
3. For occupationally exposed workers, compile occupational exposure data to include medical exposure data.
Program-level patient dose tracking provides potentially valuable quality assessment data that can demonstrate:
1. A program’s overall radiation-based cardiovascular procedures utilization rates.
2. The range of administered per-procedure radiation doses for comparison to national norms and identification of outliers.
"Consequently, for quality assessment and improvement purposes, a program should track, compile and analyze its radiation exposure data," the consensus document states.
Minimizing Patient Radiation Exposure in X-ray Fluoroscopy
There is agreement among the cardiology society experts in the consensus document that patient and staff dose could be better minimized in the cath lab by optimizing equipment performance and improving operator behavior. Physician education and increasing operator awareness of radiation dosing are seen as the key factors that can enable change.[9]
The document cites the success in reducing dose in the interventional cardiology laboratories of the Mayo Clinic, Rochester, Minn. Along with technical optimization of the equipment and fellow education, radiation exposure was announced during the case in air-kerma increments of 3,000 mGy. Procedures exceeding 6,000 mGy were referred to the radiation safety committee, and immediate physician feedback was provided. Over the course of three years, there was a 40 percent reduction in radiation dose achieved.[10]
The Mayo Clinic experience also provides benchmark data for fluoroscopy time and patient dose at the interventional reference point, which the consensus document states can be used as a baseline to measure other labs. The study reported a median fluoroscopy time for left heart catheterization and coronary arteriography of 5.8 minutes and for percutaneous coronary intervention of 15.7 minutes. The corresponding skin doses for coronary arteriography were median 467 mGy with a 75th percentile of 936 mGy. For percutaneous coronary intervention, the median skin dose was 952 mGy with a 75th percentile of 1,491 mGy. These values reflect a combination of operator proficiency and X-ray equipment quality and calibration, the consensus document cited.
When measuring angiography radiation dose, the document said there are two types of readily available patient exposure metrics used by the X-ray unit:
• Procedure fluoroscopy and cine acquisition time
• Patient exposure metrics: total air kerma at the interventional reference point and total procedure KAP
Patient dose and imaging time monitoring should be conducted with two purposes in mind, according to the consensus document authors:
• To identify trends for excessive dose and imaging times in group data from overall facility experience. This will enable identification of physician operators who employ excessive fluoroscopic and cine times.
• To identify individual outlier procedures that receive excessive exposures. This will enable recognition and prompt treatment of patients who are at risk of radiation skin injury.
Appropriate quality assurance surveillance should include both of these parameters, the consensus authors stated. In particular, patient interventional reference point doses that exceed the threshold for potential skin injury (5 Gy) should be reviewed and the affected patients should be counseled to be aware of the skin injury potential. A follow-up protocol should be in place for these patients. The Joint Commission has identified a skin entrance dose >15 Gy as a reviewable sentinel event.[11]
Role of Quality Assurance
"A robust quality assurance process is central to the safe and efficient operation of any clinical service and is particularly important when the service’s activities expose the patient and personnel to potential risk, as is the case with procedures that utilize ionizing radiation," the consensus document stated.
The authors said because radiation is undetectable by human senses, there is potential to undervalue its importance as a hazard, and for inadvertent or unrecognized excessive exposure either to patients or staff. So, they said quality assurance procedures need to be in place to act as a check to help minimize patient and personnel exposures. Quality assurance, guided by the as low as reasonably achievable (ALARA) principle, involves both examining current practices and monitoring exposures of patients and personnel.
The consensus states quality assurance programs should consider incorporating the following goals:
1. To survey a facility’s current operations with respect to the exposures being delivered to patients and personnel, and to compare them to benchmark values (where available).
2. To identify improvement opportunities to decrease exposures.
3. Establish requirements for user training.
4. Collaboration between the healthcare professional community and U.S. Food and Drug Administration (FDA) to develop diagnostic reference levels for CT, fluoroscopy, and nuclear cardiology procedures locally and also through a national radiation dose registry.
On this final point, it was noted that the American College of Radiology (ACR) has created a national dose index registry that permits participating sites to compare their dose indexes to regional and national values.[12] While this is a big step forward, the consensus authors note the registry currently is oriented toward diagnostic reference dose levels for CT abdominal and head examinations, with little emphasis on CT of the chest or X-ray fluoroscopy.
"Successful quality assurance involves monitoring and tabulating radiation exposure to patients and clinical staff," the document states. "These data should be monitored over time for trends as well as to identify individual outlier cases. Clinical staff and operators should receive feedback characterizing their individual performances and exposure."
The document also said quality assurance efforts need to be ongoing to continue to reduce patient and personnel exposure as new developments or practices emerge.
Read the complete report at www.onlinejacc.org/content/early/2018/04/30/j.jacc.2018.02.016
Related Cardiac Radiation Dose Content:
Dose-Lowering Practices for Nuclear Cardiology
Dose-Lowering Practices for Cath Lab Angiography
Defining the Cath Lab Workplace Radiation Safety Hazard
14 Ways to Reduce Radiation Exposure in the Cath Lab
Regulatory Requirements: The Impact on Cardiac Imaging and Dose Management
Role of Dose Tracking Systems in Radiation Safety Programs
References:
4. Rehani M., Frush D. (2010) Tracking radiation exposure of patients. Lancet 376:754–755.

 October 24, 2025
October 24, 2025