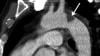
An emotional reunion with COVID-19 patient Crystal Gutierrez and the clinicians and cardiologist who saved her life at HCA Houston Healthcare Medical Center and Houston Heart. Gutierrez, a young mother who earlier in 2020 fell seriously ill from the effects of COVID-19 after delivering her son Matthew, spent 152 days in the hospital fighting again and recovering from COVID. Due to profound respiratory failure, she was put on extracorporeal membrane oxygenation (ECMO) therapy to take over the oxygenation of her blood from the lungs, and to unload the work of the heart by circulating her blood. The ECMO procedure was performed by Keshava Rajagopal, M.D., Ph.D., at Houston Heart.
Crystal was reunited February 12, 2021, with the doctors and nurses of HCA Houston Healthcare Medical Center and Houston Heart who helped to save her life.
DAIC's focus is coverage of cardiovascular technologies like ECMO, but this video drives home the message that these technologies are used to save lives and the work by clinicians and cardiologists has a profound effect on patients and their families. This is an impact is often academic in discussion and is rarely seen by people who do not work directly with patients in hospitals.
Many hospitals now "clap out" severe COVID patients at discharge. It has become a sort of rite of passage in honor of these patients overcoming adversity and surviving a very dangerous bout with the pandemic virus. It is also often a moral boost to clinicians who participate, having helped the patient fight and survive.
As of the publication of this video on DAIC Feb. 16, 2021, more than 487,000 Americans have died from the COVID-19. Worldwide there have been more than 2.41 million deaths.
Read more in the article COVID Mother Reunited With Caregivers After Saving Her Live With ECMO.
Related ECMO Use in COVID-19 Content:
FDA Approves ECMO to Treat COVID-19 Patients
VIDEO: ECMO Support Effective in Sickest COVID-19 Patients — Interview with Ryan Barbaro, M.D.
ECMO Used to Treat Adult Respiratory Distress Syndrome Case
ECMO Support Found Effective in Sickest of COVID-19 Patients
VIDEO: Multiple Cardiovascular Presentations of COVID-19 in New York — Interview with Justin Fried, M.D., explaining a case that used VV-ECMO abnd VAV-ECMO