In this segment of our DAIC Thought Leadership Series, which features one-on-one conversations with cardiovascular leaders, we're talking with Dr. Jeffrey Soble. He serves both as a practicing cardiologist at Rush University Medical Group’s Cardiology Intensive Care Unit, and CEO of Ascend Cardiovascular. In this video he addresses some of the challenges related to collaborating in complex cardiology settings, and provides insight into ways telepresence and augmented reality can be used — from a clinical perspective, using a holistic approach to structured reporting.
Videos
DAIC Thought Leadership Series: Collaboration Challenges in Complex Cardiology Settings
In this segment of our DAIC Thought Leadership Series, which features one-on-one conversations with cardiovascular leaders, we're talking with Dr. Jeffrey Soble. He serves both as a practicing cardiologist at Rush University Medical Group’s Cardiology Intensive Care Unit, and CEO of Ascend Cardiovascular. In this video he addresses some of the challenges related to collaborating in complex cardiology settings, and provides insight into ways telepresence and augmented reality can be used — from a clinical perspective, using a holistic approach to structured reporting.
Information Technology
Industry trade shows and conferences seem to be making their comeback in 2024. And the Healthcare Information and Management Systems Society (HIMSS) Global Conference and Exhibition seems particularly poised to deliver the best of the best when it comes to digital transformation in both the delivery of healthcare, but also the delivery of a quality experience for those in this demanding, rapidly evolving industry. This month in our ongoing One on One series with industry leaders, we are talking with Hal Wolf, FHIMSS, president and CEO of HIMSS. He offered insights on the society’s new partnership with Informa Markets, key topics being covered at HIMSS24, AI’s impact on the industry, and his thoughts on healthcare sustainability.
Find more HIMSS24 conference coverage here
A New Partnership for Growth
Last August, Informa Markets and HIMSS announced a landmark partnership to propel the growth and evolution of the HIMSS Global Health Conference and Exhibition, recognized as the most influential healthcare technology event of the year, and in North America. It draws 40,000 health professionals, tech leaders, providers and governmental organizations from across the globe. Informa Markets, the world’s largest exhibition organizer, took on management of the HIMSS Exhibition, while HIMSS continues to oversee developing expert content and programming.
Exciting New Features at HIMSS24
At HIMSS2024, with this new collaboration comes new features, including:
- A Digital Health Technology Theme Park, filled with innovations that revolve around AI, workforce and the business of healthcare;
- The Government Connections Plaza, featuring the latest rundown from Washington;
- A reimagined Interoperability Showcase for a deeper dive into the inner workings of healthcare;
- Hot topics will be featured on the exhibition Main Stage; and
- A Hosted Buyer Program, facilitating focused meetings between providers and trusted companies in healthcare technology.
Related content:
Find more HIMSS24 conference coverage here
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
HIMMS is working to bring empirical knowledge and evidence of value and impact of digital maturity measured by the HIMSS maturity models and the Digital Health Indicator (DHI), which is a blueprint for digital health advancement. The maturity models provide prescriptive frameworks to healthcare organizations to help build their digital health ecosystems. DAIC spoke with Anne Snowdon, RN, PhD, FAAN, professor of strategy entrepreneurship, Odette Business School, University of Windsor, CEO of SCAN Health and Chief Scientific Research Officer, HIMSS Analytics, to find out more about these models, and what the latest scientific research is telling us.
Dr. Anne Snowdon is a Professor of Strategy and Entrepreneurship at the Odette School of Business, University of Windsor. Currently, Dr. Snowdon is the Chief Scientific Research Officer for HIMSS, Vice Chair of the Board of the Directors for Alberta Innovates, and member of the Health Futures Council of Arizona State University (ASU). She is an Adjunct Faculty at the Department of Computer Science at the University of Windsor, the School of Nursing at Dalhousie University and the Centre for Innovative Medical Technology (CIMT), at the University of Southern Denmark. Dr. Snowdon is leading a national Community of Practice to advance supply chain resilience across Canada, she has published more than 150 research articles, papers and cases, has received over $24 million in research funding, holds patents and has commercialized a highly successful booster seat product for children traveling in vehicles and is a Fulbright Scholar. She holds a PhD in Nursing from the University of Michigan, an MSc from McGill University, and BScN from Western University.
Find more HIMSS23 coverage here
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
Related Digital Transformation Content:
Robocath Launches New Robotic Platform R-One+
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
New ACC President Defines Priorities for Year Ahead
Health That Connects + Tech That Cares at HIMSS 2023
ACC22: Transforming Cardiovascular Care
Healthcare is constantly evolving, finding new ways to innovate and advance digital tools and technology. With this comes the need for transformation to keep up with these advancements. DAIC spoke with Anne Snowdon, RN, PhD, FAAN, professor of strategy entrepreneurship, Odette Business School, University of Windsor, CEO of SCAN Health and Chief Scientific Research Officer, HIMSS Analytics, to find out more about the steps needed for this transformation and what we can expect to see in the future of healthcare.
Dr. Anne Snowdon is a Professor of Strategy and Entrepreneurship at the Odette School of Business, University of Windsor. Currently, Dr. Snowdon is the Chief Scientific Research Officer for HIMSS, Vice Chair of the Board of the Directors for Alberta Innovates, and member of the Health Futures Council of Arizona State University (ASU). She is an Adjunct Faculty at the Department of Computer Science at the University of Windsor, the School of Nursing at Dalhousie University and the Centre for Innovative Medical Technology (CIMT), at the University of Southern Denmark. Dr. Snowdon is leading a national Community of Practice to advance supply chain resilience across Canada, she has published more than 150 research articles, papers and cases, has received over $24 million in research funding, holds patents and has commercialized a highly successful booster seat product for children traveling in vehicles and is a Fulbright Scholar. She holds a PhD in Nursing from the University of Michigan, an MSc from McGill University, and BScN from Western University.
Find more HIMSS23 coverage here
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
Related Digital Transformation Content:
Robocath Launches New Robotic Platform R-One+
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
New ACC President Defines Priorities for Year Ahead
Successfully creating and implementing artificial intelligence (AI) and analytic solutions in general requires a number of key factors, including data quality and a certain level of expertise. DAIC had a conversation with Julius Bogdan, a leading expert in Digital transformation, Data and analytics, and Artificial intelligence and machine learning, to learn more about the key components needed to create and implement AI and digital transformation solutions.
Julius is Vice President and General Manager, Digital Health Advisory Team for the Healthcare Information and Management Systems Society (HIMSS). In that role, he leads sales, business development, product management, product marketing and advisory services teams across the continent on digital health transformation. He is responsible for the growth of the HIMSS Analytics portfolio adoption, channel strategy, and cultivating relationships across the provider, payer and public sector health landscape. He also serves on the advisory council of various start-ups and early stage firms in finance and healthcare on technology trends, architecture and market analysis.
Find more HIMSS23 content here
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
Related Digital Transformation Content:
Robocath Launches New Robotic Platform R-One+
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
New ACC President Defines Priorities for Year Ahead
With the help of artificial intelligence, cutting-edge technology is being developed that will help improve patient outcomes and build efficiencies in healthcare, which will help transform the future of healthcare delivery. DAIC sat down with Julius Bogdan, a leading expert in Digital transformation, Data and analytics, and Artificial intelligence and machine learning, to find out more about the inroads AI is making.
Julius is Vice President and General Manager, Digital Health Advisory Team for the Healthcare Information and Management Systems Society (HIMSS). In that role, he leads sales, business development, product management, product marketing and advisory services teams across the continent on digital health transformation. He is responsible for the growth of the HIMSS Analytics portfolio adoption, channel strategy, and cultivating relationships across the provider, payer and public sector health landscape. He also serves on the advisory council of various start-ups and early stage firms in finance and healthcare on technology trends, architecture and market analysis.
Find more HIMSS23 content here
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
Related Digital Transformation Content:
Robocath Launches New Robotic Platform R-One+
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
New ACC President Defines Priorities for Year Ahead
This year at HIMSS, the theme is Health That Connects + Tech That Cares, and cybersecurity is indeed a part of this picture. ITN spoke with Lee Kim, who is the Senior Principal, Cybersecurity and Privacy at the Healthcare Information and Management Systems Society (HIMSS), on cybersecurity and how healthcare is at risk. In the video, Lee also discusses the 2022 HIMSS Healthcare Cybersecurity Survey, which reflects the opinions of healthcare cybersecurity professionals. You can more information about the survey results here.
Find more HIMSS23 content here
2022 HIMSS Healthcare Cybersecurity Survey Report Results Published
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
Related Digital Transformation Content:
Robocath Launches New Robotic Platform R-One+
VIDEO: Using Maturity Models to Measure Digital Health
VIDEO: Moving Digital Transformation Forward in Healthcare
VIDEO: Key Components to Creating and Implementing AI and Digital Transformation Solutions
VIDEO: The Benefits and Pitfalls of Artificial Intelligence in Healthcare
VIDEO: A Look at Cybersecurity and How Healthcare is at Risk
New ACC President Defines Priorities for Year Ahead
Artificial intelligence and general consolidation were two top cardiology trends at RSNA22. ITN/DAIC spoke with Val Kapitula, partner, Paragon Consulting Partners LLC, about some of the trends he is seeing emerge in this field.
Related content:
RSNA 2022 Theme in Action: Empowering Patients and Partners in Care
Photo Gallery of Radiology Technology, Highlights from RSNA 2022
RSNA 2022 Day 4: Back to Basics on AI, ABUS Training, and ML in RO
RSNA 2022 Plenary Speaker Omary Urges Radiologists to Support Patients, Communities and the Planet
RSNA 2022: Innovative Solutions on Display, Leadership Addresses Value of Imaging
RSNA 2022 Day 2: Focus on Breast Screening & AI, Future of Patient Care
At TCT 2022, Jane Leopold, MD, a cardiologist at Brigham and Women’s Hospital; Director, Women's Interventional Cardiology Health Initiative; and Associate Professor, Harvard Medical School, presented on Precision Cardiovascular Medicine. She spoke with DAIC about some of the goals of precision medicine and how this data can be used.
Related TCT 2022 Coverage:
VIDEO: 3-Year Follow-up of the SYMPLICITY HTN-3 Trial
VIDEO: Unique Features of Coronary Artery Disease in Women
Cardiovascular Research Foundation’s (CRF) TCT 2022 in Review
Photo Gallery Highlighting TCT 2022
Cardiovascular Research Foundation’s (CRF) TCT 2022 in Review
TCT 2022 Honors Recipient of Thomas J. Linnemeier Young Investigator Award
TCT 2022 Announces Winner of Shark Tank Innovation Award
Educational Leaders Join Forces on Educational Opportunities
Top TCT 2022 Award Recipients announced by Cardiovascular Research Foundation (CRF)
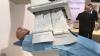
Here are two examples of artificial intelligence (AI) driven pulmonary embolism (PE) response team apps featured by vendors Aidoc and Viz.AI at the 2021 Radiological Society of North America (RSNA) 2021 meeting.
The AI scans computed tomography (CT) image datasets as they came off the imaging system and looked for evidence of PE. If detected by the algorithm, it immediately sends an alert to the stroke care team members via smartphone messaging. This is done before the images are even loaded into the PACS. The radiologist on the team can use a link on the app to open the CT dataset and has basic tools for scrolling, windowing and leveling to determine if there is a PE and the severity. The team can then use the app to send messages, access patient information, imaging and reports. This enabled them all to be on the same page and can communicate quickly via mobile devices, rather than being required to use dedicated workstations in the hospital.
Both vendors showed similar apps for stroke at RSNA 2019. That idea for rapid alerts, diagnosis and communications for acute care teams has now expanded to PE and also for aortic dissection and abdominal aortic aneurysms (AAA). AI.Viz and Aidoc are looking at expanding this type of technology for other acute care team rolls, including heart failure response.
Read more about this technology in the article AI Can Facilitate Automated Activation of Pulmonary Embolism Response Teams.
Advancements in analytics and data visualizations are helping to streamline operations and improve productivity at cath labs across the country. Kootenai Health in Coeur d'Alene Idaho has a single cath lab performing more than 2,000 cases per year. Diane Penkert, executive director of heart and vascular services, discusses how the implementation of the Philips Performance Bridge analytics platform has enabled them to better leverage cardiovascular procedure data.
The vendor Radiaction introduced a new type of scatter radiation protection shielding system that mounts to the angiography system in the cath lab. It was shown for the first time at the 2021 Radiological Society of North America (RSNA) annual meeting.
The system uses a motorized series of tungsten-polymer radiation shield plates that extend down from the detector, and up from the X-ray source, to the patient and bottom of the table. This greatly reduces scatter radiation in the lab, by as much as 92% according to the company's research.
The shields are deployed using a table-side controller. The shield has sensors to stop extending when it comes close to the patient or the table. The shield can be partly pulled back to enable panning the table. The company said the shield can be mounted on existing angiography C-arms.
It has CE mark and is installed clinically in two cath labs in Israel. The company hopes to submit for U.S. FDA review in 2022.
Related Cath Lab Radiation Dose Reduction Content:
Defining the Cath Lab Workplace Radiation Safety Hazard
VIDEO: Minimizing X-ray Exposure to Physicians During Interventional Procedures With the ControlRad System — Interview with Dr. Simon Dixon
Medical Imaging Radiation Levels in U.S. Dropped Over Past Decade
Philips Developing X-ray Free Cath Lab Imaging to Replace or Supplement Angiography
VIDEO: Reducing Cath Lab Radiation Dose at Henry Ford Hospital
VIDEO: Technologies and Techniques to Reduce Radiation Dose in the Cardiac Cath Lab — Interview with Akshay Khandelwal, M.D.
Dose-Lowering Practices for Cath Lab Angiography
5 Technologies to Reduce Cath Lab Radiation Exposure
VIDEO: Heart Surgeon Shares Effects of Fluoroscopic Radiation Exposure
Helping Interventional Cardiologists Reduce Exposure to Ionizing Radiation
Dr. Simon Dixon, MBChB, chair of the Department of Cardiovascular Medicine at Beaumont Hospital Royal Oak, the Dorothy Susan Timmis Endowed Chair of Cardiology, and a professor of medicine at Oakland University William Beaumont School of Medicine, spoke at the 2021 Transcatheter Cardiovascular Therapeutics (TCT) meeting about a study Beaumont performed to lower radiation dose in the cath lab by more than 50%.
Using a new angiographic collimation technology from ControlRad, it helped cut radiation dose to interventional cardiologists by 57%. The device collimates the area of interest where the physicians are working, and reduces the dose significantly to peripheral areas in the image. This reduces exposure to ionizing X-ray radiation scatter from the imaging system. It is one of two new radiation protection systems used at Beaumont.
The ControlRad device, approved for commercial cath lab use by the FDA in December 2020, is retrofitted to X-ray equipment in the catheterization lab. It creates a type of aperture that collimates the image area being viewed. By using a touch pad attached to the table side rail, the cardiologist controls the aperture to narrow or widen the field of view on the X-ray, which in turn reduces the amount of radiation used to produce the images. It works with gloves on.
For the study, cath lab workers wore radiation-detecting badges near their thyroid and inside their lead apron during procedures. Another badge was placed on a wall inside the lab. The study detected a 55% to 57% decrease in radiation exposure at the thyroid position of the main cardiologist, or lead operator, and a 49% decrease in radiation exposure to the cardiologist assisting, or operator 2. The badge on the wall detected a 38% decrease in radiation exposure, reflecting the dose savings to other cath lab staff further away from the imaging system.
Beaumont is also using the the Protego system, which places a barrier wall between the imaging equipment and the operator and staff in the cath lab. While it does not protect the patient from radiation during their procedure, it is designed to allow staff to work in the cath lab without wearing a heavy lead apron.
One of the trends in cardiovascular information system (CVIS) and radiology PACS at the Healthcare Information Management Systems Society (HIMSS) 2021 conference was the deeper integration of third-party image analysis software and artificial intelligence (AI) into these systems. This eliminates software sitting on top of the CVIS or PACS, separate logins or needing to us a different screen or manually transferring information from the third-party app in into the final report.
A good example of this was Siemens Healthineers, which demonstrated a deep integration with Epsilon Imaging’s echocardiography strain imaging analysis software. The integration eliminates the need for a separate login to the software, and automated quantification and images are carried over directly into the syngo echo report.
Strain can be used to assess cardiac function more precisely than regular cardiac ultrasound exams. It has grown in its use for cardio-oncology programs, assessing a baseline cardiac function and the. Performing serial exams over the course of a cancer patient’s chemotherapy. Strain has seen growing interest and has been a hot topic the past couple years at the American Society of Echocardiography (ASE) meeting. Interest also has expanded greatly recently with reimbursement now available in the U.S.
Siemens said there also has been increased interest in strain this past year because it can show early indicators of cardiac issues in COVID-19 patients and can be used to help monitor COVID myocarditis patients.
Related Strain Echo and HIMSS Content:
VIDEO: An Overview of Echo Strain Imaging — Interview with Marielle Scherrer-Crosbie, M.D.
Strain Imaging Improves Cardiac Surveillance of Certain Breast Cancer Patients
VIDEO: Assessing Cardiotoxicity Response With Cardio-Oncology Echo Imaging — Interview with Federico Asch, M.D.
Assessing Cardiotoxicity Due to Cancer Therapy
Advances in CVIS and Enterprise iImaging at HIMSS 21
VIDEO: Cardiology AI Aggregates Patient Data and Enables Interactive Risk Assessments
Photo Gallery of New Technologies at HIMSS 2021
VIDEO: Importance of Body Part Labeling in Enterprise Imaging — Interview with Alex Towbin, M.D., at HIMSS21
VIDEO: Coordinating Followup for Radiology Incidental Findings — Interview with David Danhauer, M.D., at HIMSS21
The vendor MediCardia demonstrated smart software to aggregate cardiology patient data from numerous locations into one place at the 2021 Healthcare Information Management Systems Society (HIMSS) conference. This enables one dashboard view of the patient's relevant cardiac history, prior exams, imaging, ECGs, labs and procedures. It also uses artificial intelligence (AI) to pull key data elements about the patient to automatically create risk assessments based on current guidelines in a graphical format.
The interactive system also allows the cardiologist to adjust parameters in the patient risk score to immediately show the patient any impact on their score. This includes if they stopped smoking, began taking statins, etc. The dynamic graphics of the system are also designed to be more engaging with a patient during consultations, rather than plain white pages of reports.
MediCardia HeartChart is a cardiology-focused virtual care platform that serves as a unified and common interface for EHRs and remote technologies including wearables, consumer home medical devices, and implanted cardiac rhythm devices.
Related HIMSS CVIS and PACS Content:
Read about more advances in PACS and enterprise imaging at HIMSS 21.
VIDEO: Example of Epsilon Strain Imaging Deep Integration With Siemens CVIS
Photo Gallery of New Technologies at HIMSS 2021
VIDEO: Importance of Body Part Labeling in Enterprise Imaging — Interview with Alex Towbin, M.D.
VIDEO: Coordinating Followup for Radiology Incidental Findings — Interview with David Danhauer, M.D.
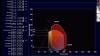
A new ultrasound imaging technology that may offer novel ways to diagnose and better understand cardiac diseases using dynamic blood flow imaging. This allows imaging of individual blood cells or contrast bubbles as they travel through the heart and vessels, showing detail in how the blood moves and swirls. These motions, including the formation of vortices, may offer new insight into different disease states and allow earlier diagnosis and a understand better when to intervene.
The examples shown in this short video are from Hitachi and GE Healthcare, both of which have highlighted this technology at the American Society of Echocardiography (ASE) annual meetings over the past four years.
Ultrasound vendors use different technology approaches, including vector flow imaging, particle imaging velocimetry and blood speckle tracking. All of them show small lines or arrows to indicate the direction the blood cells or bubbles are traveling, and color codes to indicate velocity. Some vendors offer quantification for some new measures of blood flow, but as of yet, there are no guidelines or standardized indexes as to what these numbers mean.
This technology has been discussed in research sessions at the IEEE and the ASE over the past several years. However, more research is needed to show the prognostic value of the technology. Research to date shows it is possible that the swirling of blood can indicate less efficient flow, which may have implications in the development of heart failure, pulmonary hypertension and advancement of valvular disease. In the coronary arteries, research has shown there may be a connection between sheer stresses and disrupted blood flow in the formation of plaques on artery walls.
Companies that have developed echo blood flow dynamics imaging on their ultrasound systems to date include Hitachi, GE Healthcare, Fujifilm, Mindray and BK Medical.
Read more about this technology from ASE 2021 in the article Development of Echo Blood Flow Dynamics Imaging.
Related Dynamic Blood Flow Echo Imaging Content:
Aurora St. Luke’s Medical Center in Milwaukee Adopts Latest Echocardiography Imaging Software
A Glimpse Into the Future of Cardiac Ultrasound
Analogic Introduces New Premium Cardiac Imaging Software for bk3500 Ultrasound System
Improving Stent Designs With Computational Fluid Dynamics
VIDEO: Editor's Choice of Most Innovative New Cardiac Ultrasound Technology at ASE 2017
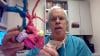
Tom Jones, M.D., director, cardiac catheterization laboratories, Seattle Children’s Hospital, explains some of the new technologies being used to treat congenital heart disease. He discusses the recent trial he served as principle investigator for the new Harmony transcatheter pulmonary valve, the development of a bioresorbable transcatheter septal occluder device, development of large bioresorbable stents for use in pediatric cases, and use of virtual and augmented reality to better understand and guide very complex congenital heart procedures. Jones also explains a patient case where a 3-D printed heart and vessels from the patient helped the heart team understand all the options and how to tackle a valve replacement in a child with a single ventricle.
Jones shared some of these advances in congenital heart intervention sessions at the Society of Cardiovascular Angiography and Interventions (SCAI) 2021 meeting.
Recent Technology Advances in Congenital Heart:
FDA Clears First Device to Treat Right Ventricular Outflow Tract Congenital Heart Disease
VIDEO: Harmony Transcatheter Pulmonary Valve Has Good Outcomes at 1 Year — Interview with Tom Jones, M.D.
FDA Expands Indication for Melody Transcatheter Valve for Failed Surgical Valves
VIDEO: Use of Virtual Reality to Aid Congenital Heart Disease — Interview with David M. Axelrod, M.D.
Bioresorbable Pulmonary Valve Replacement May Enable Cardiovascular Regeneration
VIDEO: Transcatheter Closure of Holes in the Heart — Interview with Ziyad Hijazi, M.D.
Nemours Children's Health System Uses 3-D Printing to Deliver Personalized Care
Bioresorbable ASD Occluder Prepares to Enter U.S. Clinical Trial
FDA Approves Abbott's Amplatzer Piccolo Occluder
Critical Need for Pediatric Electrophysiology Devices is Focus of Medical Device Competition
Lab-created Heart Valves Can Grow With the Patient
Abbott Receives European CE Mark for Two Pediatric Heart Devices
ASE Releases Guidelines for Transesophageal Echo in Congenital Heart Disease
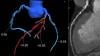
This is an example of the Medis Medical Imaging Quantitative Flow Ratio (QFR) system that offers a fractional flow reserve (FFR) blood flow measure in coronary vessels based on angiography imaging analysis alone. The FDA-cleared product allows the FFR-angio derived analysis to be performed table side in the cath lab when the patient is on the table for a procedure to determine if a patient requires a stent.
The QRF technology uses two angiography images with contrast, shot from different angles are used to create a 3-D model of the vessel segment and calculate FFR flow past a lesion. The model also can help plan for stenting.
This example was recorded by DAIC Editor Dave Fornell at the 2019 Transcatheter Cardiovascular Therapeutics (TCT) meeting.
Nick West, M.D., chief medical officer for Abbott, explains the details from a survey of 1,400 patients, physicians and healthcare executives in an effort to understand the high-level issues regarding the use of technology in medicine, the gaps in communication, and patient perceptions to guide future technology development.
Four high-level observations emerged from our study:
1. Patients are frustrated by the level of care they’re receiving – they understandably want a personalized healthcare experience “tailored for me,” across the care continuum.
2. Physicians lament the lack of time they have to spend with patients, their limited visibility into patient adherence to treatment and lifestyle changes, and challenges with other key factors that influence the quality of care they can provide.
3. Administrators are pressured to deliver patient satisfaction and reduce costs across multiple departments.
4. Diagnostic and data-driven technology holds the promise to move care from a point-in-time, intervention-only focus to a more holistic “whole patient” view by improving the accuracy of
diagnosis, appropriate interventions as required, and evidence-based post-procedural care.
Read more about the survey in the article "Emerging Technology and Data Key to Closing Treatment Gaps to Improve Cardiovascular Care."
See Part 2 of this video where West describes the how AI might be used in interventional cardiology in the VIDEO: Artificial Intelligence May Improve Cath Lab Interventions.
Enterprise viewers are designed to provide fast and easy access to a patient’s imaging history, and today’s modern healthcare systems require a clinical viewer capable of meeting the diverse needs of a large group of users. GE Healthcare’s Zero Footprint Viewer can quickly and easily display digital images, video clips and cine loops from any department and on many different devices.
It provides access to images and reports from anywhere, whether it’s on the hospital floor, in surgery, in clinic or at home, to allow clinicians to access and develop clinical insights that deliver patient results and drive operational efficiencies.
Learn more at https://www.gehealthcare.com/products/healthcare-it/enterprise-imaging/centricity-universal-viewer-zero-footprint
Advanced visualization company Medis recently purchased Advanced Medical Imaging Development S.r.l. (AMID), which developed software to automatically track and measure strain in echocardiograms. That technology is now being adapted for strain imaging in CT and MRI. Using this imaging data, the software also can noninvasively derive pressure gradient loops and curves, similar to using invasive pulmonary arterial (PA) hemodynamic pressure catheters. This information is useful in monitoring critically ill patients on hemodynamic support and to monitor worsening severity of heart failure.
The technology was discussed at the 2020 Society of Cardiovascular Computed Tomography (SCCT) virtual meeting. Examples of this technology are presented in this video.
Find more news and video from SCCT 2020
VIDEO: Photon Counting Detectors Will be the Next Major Advance in Computed Tomography
Todd Villines, M.D., FACC, FAHA, MSCCT, explains how coronary plaque assessment will become a new risk assessment tool in cardiac CT. This was a key take away during the Society of Cardiovascular Computed Tomography (SCCT) 2020 virtual meeting in July. He is the Julian Ruffin Beckwith Professor of Medicine, Division of Cardiovascular Medicine, University of Virginia; editor-in-chief of the Journal of Cardiovascular CT (JCCT), and SCCT past-president.
While basic plaque assessments have been available for several years on CT vendor and third-party advanced visualization software, it lacked automation standardization for what various values meant and clinical evidence it was relevant. However, several speakers in SCCT sessions said that is now changing, with more specific analysis being tested clinically and automation using artificial intelligence.
Several key opinion leaders in cardiac CT said this new information and automation will likely lead to a revision of the current CAD-RADS scoring system used by radiologists and cardiologists when assessing the coronary event risk of patients. They are calling for the new CAD-RADS 2.0 to include a detailed plaque assessment.
Related SCCT Key Trends and New Technology Content:
Low-attenuation Coronary Plaque Burden May Become Next Big Cardiac Risk Assessment
Top 9 Cardiovascular CT Studies in Past Year
VIDEO: Increased Use of Cardiac CT During the COVID-19 Pandemic
VIDEO: Key Cardiac CT Papers Presented at SCCT 2020
VIDEO: Photon Counting Detectors Will be the Next Major Advance in Computed Tomography
VIDEO: Artificial Intelligence to Automate CT Calcium Scoring and Radiomics
Regina Druz, M.D., FASNC, a member of the American Society of Nuclear Cardiology (ASNC) Board of Directors, chairwomen of the American College of Cardiology (ACC) Healthcare Innovation Section, and a cardiologist at Integrative Cardiology Center of Long Island, N.Y., explains the rapid expansion of telemedicine with the U.S. spread of novel coronavirus (COVID-19, SARS-CoV-2).
Druz spoke on the unprecedented expansion of telemedicine in the U.S. under COVID-19, seeing more use in the last two months, as opposed to the past two decades. The Centers for Medicare and Medicaid Services (CMS) previously only reimbursed for Telehealth in rural areas it determined had a shortage of doctors. However, in early March 2020, CMS dropped the geographic requirements and allowed Telehealth usage across th country as a way to mitigate person-to-person contact and keep vulnerable, older patients at home for routine check ups with doctors.
Druz has subspecialty certifications in nuclear cardiology, adult echocardiography and cardiac computed tomography (CT) and explains how Telehealth can be used to pre-screen patients and get patient sign off on procedures prior to coming in for an exam, helping speed the process in the hospital and limit personal contact.
Concerns about the rpaid spread of COVID-19 also has driven many radiology departments to convert to wider use of teleradiology to allow more radiologists to work from home and reduce person-to-person contact within the hospitals.
The U.S. Federal Communications Commission (FCC) adopt a $200 million telehealth program to support healthcare providers responding to the
ongoing coronavirus pandemic on April 2, 2020. Read more from the FCC.
CMS Expand Medicare Telehealth Benefits During COVID-19 Outbreak, including dropping requirements for rural health locations only, opening telehealth for use across the United States.
Watch the related VIDEO: Use of Teleradiology During the COVID-19 Pandemic — an interview with John Kim, M.D., chairman, Department of Radiology, THR Presbyterian Plano, Texas, and chief technology officer at Texas Radiology Associates.
Recommendations from Druz are also included in the Best Practices for Nuclear Cardiology Laboratories During the Coronavirus (COVID-19) Pandemic
Related COVID-19 Content:
VIDEO: Imaging COVID-19 With Point-of-Care Ultrasound (POCUS) — Interview with emergency physician Mike Stone, M.D.,
VIDEO: How China Leveraged Health IT to Combat COVID-19 — Interview with Jilan Liu, M.D., CEO for the HIMSS Greater China
Study Looks at CT Findings of COVID-19 Through Recovery
Experts Stress Radiology Preparedness for COVID-19
ACR Recommendations for the Use of Chest Radiography and CT for Suspected COVID-19 Cases
VIDEO: What Cardiologists Need to Know about COVID-19 — Interview with Thomas Maddox, M.D.
The Cardiac Implications of Novel Coronavirus
James Udelson, M.D., chief of the division of cardiology, Tufts Medical Center, explains how cardiac computed tomography (CT) scans are being used to create image-derived fractional flow reserve (FFR) values to determine if a coronary lesion is flow limiting. The FFR-CT can help determine if the patient needs a stent, or if the disease can be treated with medication. Tufts uses FFR-CT evaluations on non-emergency chest pain patients to reduce the need for diagnostic catheterizations.
Related FFR-CT Content:
Image-based FFR May Replace Pressure Wires and Adenosine
New Technology Directions in Fractional Flow Reserve (FFR)
8 Cardiovascular Technologies to Watch in 2020
VIDEO: Using FFR-CT in Everyday Practice
FFR-CT is Ready for Prime-time Evaluation of Coronary Disease
6 Hot Topics in Interventional Cardiology at TCT 2019
FFR-CT: Is It Radiology or Cardiology?
Find more news and video from Tufts Medical Center
DAIC/ITN Editor Dave Fornell takes a tour of some of the most innovative new medical imaging technologies displayed on the expo floor at the Radiological Society of North America (RSNA) 2019 meeting.
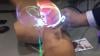
Technology examples include a robotic arm to perform remote ultrasound exams, integration of artificial intelligence (AI) to speed or automate radiology workflow, holographic medical imaging display screens, a new glassless digital radiography (DR) X-ray detector, augmented reality for transesophageal echo (TEE) training, moving DR X-ray images, 3-D printed surgical implants created from a patient's CT imaging, DR X-ray tomosynthesis datasets, radiation dose management and analytics software, and new computed tomography (CT) technologies.
Find more videos and news from RSNA 2019
The Consumer Electronic Show (CES) is the world's gathering place for consumer technologies, with more than 175,000 attendees and more than 4,400 exhibiting companies. New healthcare technologies are among the top trends at CES. This video offers a quick look at the trends specific to healthcare technology.
Artificial intelligence (AI) is one of the hottest technology trends across all product across the CES floor this year. There is also discussion by key note speakers that the internet-of-things (IOT) concept introduced at CES nearly a decade ago is now morphing into a new meaning for the interconnectivity-of-things. This can be seen in healthcare products shown here and across all types of consumer and business products.
The device technology at CES include many examples of how integrated wearables can digitally enable healthcare. The future of healthcare will include system where consumers are continuously monitored with sensors, software and services that can pinpoint digital biomarkers — earlier warning signs that predict health events. This is the prediction of Leslie Saxon, M.D., executive director of the University of Southern California (USC) Center for Body Computing (CBC), is speaking as a panelist about digital health trends and challenges in the session “Proving the Impact of Transformative Technology.”
Saxon is a board-certified cardiologist and digital health expert who understands how developing technologies can more accurately assess wellness and human performance among elite athletes, military personnel and patients. She explained this digital healthcare model of the future is a vast contrast to the current point-of-care model.
Richard Botto, CVT, RCSA, chief cardiovascular technologist, division of cardiology, cardiac cath lab, and Melissa Smith, RT, at Tufts Medical Center, Boston, explain the use of technology to remotely access data and waveforms on patients' temporary hemodynamic support system control consoles.
Tufts Medical Center was one of the first hospitals to begin using the Abiomed Impella Connect technology, which enables remote smartphone access to Impella consoles. This allows a quick, remote check on patients using temporary hemodynamic support. The technology also is connected to a support center at Abiomed, so if a console or patient is experiencing issues out of the ordinary, techs can remote into the patient's Impella control console to take a look. Tuft's intensivists in the cardiac care unit (CCU) use the app to check on their patients' consoles without needing to walk into each room.
Find VIDEOS and articles on Tufts cardiology program
Mahadevappa Mahesh, Ph.D., chief of medical physicist and professor of radiology and medical physics, Johns Hopkins University, Baltimore, treasurer of the American Association of Physicists in Medicine (AAPM),a board member of the American College of Radiology (ACR), presented a late-breaking study on how medical imaging radiation dose has started to drop over the past decade. He is the co-chair of the National Council on Radiation Protection and Measures Report (NCRP), and presented the most recent NCRP data analysis at the 2019 Radiological Society of North America (RSNA) meeting.
The new NCRP 184 report covers the period between 2006 and 2016, the period of the most current CMS data. It shows a decrease of about 20 percent in the radiation dose the U.S. population receives from medical imaging, compared to the NCRP 160 that covered the period of up to 2006.
Key findings of the study include:
• CT dose dropped about 6 percent, despite a 20 percent increase CT scans since 2006;
• Drop of more than 50 percent for nuclear imaging scans, mainly due to fewer procedures begin performed;
• A 15-20 percent decrease across X-ray imaging modalities.
Mahesh says this shows the impact of using "as low as reasonably achievable" (ALARA) principals, new dose guidelines outlined jointly by numerous medical societies, and dose reduction initiatives like Image Wisely, Image Gently, and the American College of radiology (ACR) Dose Index Registry.
He said there was growing concern a decade ago when the last council report was published, which show a steep increase in radiation dose. This was mainly due to a rapid increase in the use of computed tomography (CT) and other types of X-ray based and nuclear radiotracer medical imaging. This prompted the ACR top create the Image Wisely program and push for the use of more thoughtful imaging doses based on patient size, using the "as low as reasonably achievable” (ALARA) principle. While CT dose was lowered, he said the biggest decline was in nuclear imaging.
DAIC Editor Dave Fornell and Imaging Technology News (ITN) Consulting Editor Greg Freiherr offer a post-game report on the trends and technologies they saw on the expo floor of 2019 Radiological Society of North America (RSNA) annual meeting. This includes artificial intelligence (AI), augmented reality, holographic imaging, cybersecurity, and advances in digital radiography (DR) with a glassless detector plate, X-ray tomosynthesis, dual-energy X-ray and dynamic DR imaging.
Piotr J. Slomka, Ph.D., FACC, research scientist in the Artificial Intelligence in Medicine Program, Department of Medicine at Cedars-Sinai, and professor of medicine in-residence of the David Geffen School of Medicine, UCLA. He explains how his team at Cedars-Sinai is working on intelligent patient risk prediction algorithms that will automatically extract information from medical imaging. He spoke on artificial intelligence (AI) development for medical imaging in sessions at the 2019 American Society of Nuclear Cardiology (ASNC) annual meeting.
Find more articles and video on AI
Interview with John Carroll, M.D., director of interventional cardiology, Robert Quaife, M.D., director of advanced cardiac imaging, and James Chen, Ph.D., associate professor of medicine and director of the 3-D imaging lab at the Cardiac and Vascular Center at the University of Colorado Hospital. They discuss how the structural heart program was created and how they invested in advanced imaging to grow into one of the most advanced programs in the country. They explain how the program now incorporates transcatheter aortic valve replacement (TAVR), transcatheter mitral valve repair, transcatheter mitral valve replacement (TMVR), left atrial appendage (LAA) occlusion and transcatheter closure of holes in the heart.
The heart team in this video stressed the need for advanced imaging to plan and guide the procedures. They explain how the center developed its own 3-D imaging software and worked with Philips healthcare to commercialize some of the technologies, including the EchoNavigator system used to fuse live angiography with live transesophageal echo (TEE).
Related University of Colorado Hospital Content:
Highlighting Innovation at the University of Colorado Hospital Cardiology Program
VIDEO: Evolution of Transcatheter Mitral Valve Repair at the University of Colorado — Interview with John Carroll, M.D., and Robert Quaife, M.D.
VIDEO: The Role of Advanced Imaging in Structural Heart Interventions — Interview with Robert Quaife, M.D.
VIDEO: Advice For Hospitals Starting a Structural Heart Program — Interview with John Carroll, M.D.
VIDEO: The Evolution of Complex PCI at University of Colorado — Interview with John Messenger, M.D., and Kevin Rogers, M.D.
VIDEO: Developing New Cath Lab Technologies With Real-time Collaboration Between Industry, Doctors
360 View of the TEE Echo Workstation During a MitraClip Procedure
VIDEO: Walk Through of a Hybrid Cath Lab at the University of Colorado Hospital
VIDEO: Cath Lab Walk Through at the University of Colorado Hospital
VIDEO: The Cardiac Surgeon Perspective on Transcatheter Mitral Valve Repair — Interview with Joe Cleveland, M.D.
VIDEO: An Overview of PFO Closure to Treat Cryptogenic Stroke — Interview with Karen Orjuela, M.D.,
(This video was originally posted in May 2019 and was updated Oct. 2, 2019)
A discussion with Nicolas Bevins, Ph.D., vice chair, physics and research, and Jessica Harrington, RCIS. They explain the use of shields, technique and use of newer angiography technologies to reduce X-ray radiation dose in the cardiac cath labs at Henry Ford Hospital, Detroit.
Watch the VIDEO: Technologies and Techniques to Reduce Radiation Dose in the Cardiac Cath Lab — Interview with Akshay Khandelwal, M.D., director of medical operations at the Henry Ford Heart and Vascular Institute
Additional articles and videos on Henry Ford Hospital
For more on how to reduce dose in the cath lan, read these related articles:
Cardiology Societies Call for Better Radiation Dose Tracking
Defining the Cath Lab Workplace Radiation Safety Hazard
Dose-Lowering Practices for Cath Lab Angiography
5 Technologies to Reduce Cath Lab Radiation Exposure
VIDEO: Heart Surgeon Shares Effects of Fluoroscopic Radiation Exposure
Helping Interventional Cardiologists Reduce Exposure to Ionizing Radiation
14 Ways to Reduce Radiation Exposure in the Cath Lab
(Editor's note - this video was originally published in September 2018 and was revised September 2019)
Akshay Khandelwal, M.D., director of medical operations at the Henry Ford Heart and Vascular Institute, Detroit, and associate professor of cardiology at Wayne State University, explains how his center has reduced X-ray radiation dose in the cardiac catheterization labs.
Watch the related VIDEO: Reducing Cath Lab Radiation Dose at Henry Ford Hospital — Discussion with Nicolas Bevins, Ph.D., vice chair, physics and research, and Jessica Harrington, RCIS, Henry Ford Hospital.
Additional articles and videos on Henry Ford Hospital
For more on how to reduce dose in the cath lan, read these related articles:
Cardiology Societies Call for Better Radiation Dose Tracking
Defining the Cath Lab Workplace Radiation Safety Hazard
Dose-Lowering Practices for Cath Lab Angiography
5 Technologies to Reduce Cath Lab Radiation Exposure
VIDEO: Heart Surgeon Shares Effects of Fluoroscopic Radiation Exposure
Helping Interventional Cardiologists Reduce Exposure to Ionizing Radiation
14 Ways to Reduce Radiation Exposure in the Cath Lab
(Editor's note - this video was originally published in November 2018 and was revised September 2019)
An example of Siemens' photo-realistic Cinematic image reconstruction. This image is from a CTA exam from a Siemens Force CT scanner.
Vendors who offer this realistic type of CT image rendering say it is not used for diagnostics. However, the technology can be helpful when explaining things to the patient and their family, educating physicians and staff, and for surgeons, since it offers a realistic view of the anatomy that is easier for most people to understand who are not familiar with cardiac anatomy as it appears in traditional CT multiplanar reconstruction (MPR) images.
This example of software was demonstrated on the expo floor at the 2019 Society of Cardiovascular Computed Tomography (SCCT) meeting.
This is a quick video example of a cardiac computed tomography (CT) exam showing a Medtronic CoreValve transcatheter aortic valve replacement (TAVR) device implanted. The image was reconstructed using Canon Medical’s Global Illumination photo-realistic rendering advanced visualization post-processing software. Vendors who offer this realistic type of CT image rendering say it is not used for diagnostics. However, the technology can be helpful when explaining things to the patient and their family, educating physicians and staff, and for surgeons, since it offers a realistic view of the anatomy that is easier for most people to understand who are not familiar with cardiac anatomy as it appears in traditional CT multiplanar reconstruction (MPR) images.
This example of software was demonstrated on the expo floor at the 2019 Society of Cardiovascular Computed Tomography (SCCT) meeting.
Joao Cavalcante, M.D., FSCCT, director of structural heart CT and cardiac MRI, Minneapolis Heart Institute, discusses transcatheter mitral valve replacement (TMVR) imaging requirements at the Society of Cardiovascular Computed Tomography (SCCT) 2019 meeting. SCCT held its first TMVR planning hands-on workshop, which he was involved in. TMVR is expanding with currently FDA cleared valve-in-valve (VIV) and valve-in-ring (VIR) procedures.
Related TMVR Content:
Interventional Imagers: The Conductors of the Heart Team Orchestra
VIDEO: The Importance of the Neo-LVOT in Transcatheter Mitral Valve Replacement — Interview with Dee Dee Wang, M.D.
VIDEO: Transcatheter Structural Heart Procedure Navigation Technology Advances — Interview with Stephen Little, M.D.
Recent Advances in Transcatheter Valve Technology
Abbott Begins Tendyne Transcatheter Mitral Valve U.S. Pivotal Trial
VIDEO: The Essentials of CT Transcatheter Valve Imaging — Interview with Jonathon Leipsic, M.D.,
New LAMPOON Technique Reduces LVOT Obstruction in Transcatheter Mitral Valve Replacement
This is a quick example of how artificial intelligence (AI) is being integrated on the back end of cardiac ultrasound systems to help automate and speed workflows. This video segment is from the expo floor of the 2019 American Society of Echocardiography (ASE) meeting. It shows AI-based AFI automation features incorporated into the GE Vivid E95 echo system.
Read a blog about how AI will help advance cardiac ultrasound imaging, Combatting the No. 1 Cause of Death With the Help of Artificial Intelligence and Advanced Technology.
Marielle Scherrer-Crosbie, M.D., Ph.D., director of echocardiography at the Hospital of the University of Pennsylvania, and chair of the 2019 American Society Of Echocardiography (ASE) sessions, explains how cardiac ultrasound strain imaging is being used and where the technology is at the ASE 2019 meeting. She is an expert in echo strain, which is gaining wider usage in echocardiography, especially for cardio-oncology assessments. She spoke at the 2019 American Society of Echocardiography (ASE) meeting.
Related Cardio-oncology Content:
VIDEO: Echocardiography Strain Fundamentals Made Easy
Strain Imaging Improves Cardiac Surveillance of Certain Breast Cancer Patients
Assessing Cardiotoxicity Due to Cancer Therapy
VIDEO: Assessing Cardiotoxicity Response With Cardio-Oncology Echo Imaging — interview with Federico Asch, M.D.
New Echo Protocol Aids Monitoring Children’s Heart Abnormalities Due to Chemotherapy
Strain Imaging Improves Cardiac Surveillance of Certain Breast Cancer Patients
VIDEO: Characterization of Cardiac Structural Changes and Function Following Radiation Therapy
Study Demonstrates Strain Imaging Utility With Contrast-Echo Studies
VIDEO: Echocardiography Strain Fundamentals Made Easy
Strain Imaging Improves Cardiac Surveillance of Certain Breast Cancer Patients
Automation Enhances, Streamlines Echocardiography
Roberto Lang, M.D., director of cardiac imaging at the University of Chicago, has been working with TomTec for the past three years on a project to use virtual reality (VR) to edit and view 3-D cardiac ultrasound and CT scans. He spoke at a couple sessions this week at the 2019 American Society Of Echocardiography (ASE) meeting, where doctors were able to view the session using VR headsets. The hands-on demonstration of this technology in the TomTec booth at ASE 2018 and 2019 was one of the most popular exhibits with attendees both years.
Read more about this technology in Top Technology Trends in Echocardiography at ASE 2018
See examples of VR technology for echo in the VIDEO: Editor’s Choice of the Most Innovative Echo Technology at ASE 2018
Here is a video example of this technology being demonstrated at ASE19.
Jacques Kpodonu, M.D., FACC, cardiac surgeon, Beth Israel Deaconess Medical Center, and professor at Harvard Medical School, explains how medical devices and wearables that interface with smartphones and apps might be used to eliminate healthcare disparities in rural areas of the developed world and help raise the level of care in the developing world. He spoke at the 2019 AI-Med Cardiology conference.
Related Smartphone and Wearable Content:
VIDEO: Use of Wearable Medical Devices for Cardiac Rehabilitation — Interview with Robert Klempfner, M.D.
VIDEO: Use of Wearables to Track Electrophysiology Patients — Interview with Khaldoun Tarakji, M.D.
Smartphones Used to Successfully Screen More than 60,000 for Atrial Fibrillation
VIDEO: The Future of Wearables in Healthcare — Interview with Karl Poterack, M.D.
VIDEO: Artificial Intelligence Applications for Cardiology — Interview with Anthony Chang, M.D.